While Ethiopia’s extensive health post network and comprehensive primary care facilities reach rural populations, such access in Kenya is still constrained by distance in underserved regions.
At a time when many African countries are still grappling with how to translate policy into measurable health outcomes, Ethiopia is positioning itself as a case study in how sustained investment in primary healthcare can deliver tangible gains, particularly for mothers and newborns.
This was the central focus of a high-level session at the 2026 International Maternal and Newborn Health Conference (IMNHC) in Nairobi. Drawing from over two decades of reforms, Ethiopia’s health leaders and global partners outlined a model built on political commitment, community systems, and targeted innovation, one that offers both inspiration and caution for countries like Kenya.

Dr Dereje Duguma, Ethiopia’s Minister of Health, said the country’s progress is neither accidental nor recent; it is the result of deliberate, long-term investment in a primary care system anchored in communities.
“At the centre of our success is the health extension program,” he said. “Over 40,000 health extension workers have been deployed across villages and districts, forming the backbone of service delivery at the household level.”
These workers conduct home visits, provide basic services, and identify high-risk pregnancies early. According to Dr Duguma, “more than 60 per cent of their work is focused on maternal and child health.”
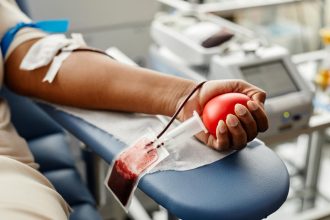
Blood banks in more than 100 hospitals have improved maternal and child health
The results are measurable. According to Ethiopian Ministry of Health data, the maternal mortality ratio declined from 871 deaths per 100,000 live births in 2000 to 412 in 2016 and to 141 in 2024–2025. The country now targets fewer than 70 deaths per 100,000 by 2030.
“This progress is driven by leadership commitment at every level,” Dr Duguma noted, pointing to sustained investments in infrastructure, workforce, and essential commodities. “We have established blood banks in more than 100 hospitals, and these are some of the government’s commitments in the primary care system that have improved maternal and child health.”
With a population exceeding 120 million, 76 per cent of whom live in rural areas, Ethiopia’s health system prioritises proximity. Yonas Zula, senior technical advisor to the minister, outlined the structure: “Over 15,000 health posts, nearly 4,000 health centres, and 275 primary hospitals form a three-tiered system in which 80 per cent of services are delivered at the primary care level.”
Strong community engagement mechanisms, including women’s development groups, village health leaders, and male and youth engagement strategies, create a dense network linking households to the formal system. Institutional deliveries have risen from five per cent in 2000 to around 61 per cent. “Assisted skilled deliveries have similarly increased, contributing to a reported 83 per cent reduction in maternal mortality over the past 25 years,” said Zula. More than 1,900 maternity waiting homes help women from remote areas stay near facilities as they approach delivery.
Dessalew Altaye, Project Director at JSI, highlighted the “network of care” model, which links community services and facilities into a coordinated system, improving referrals and resource sharing. Early data shows a 40 per cent reduction in perinatal mortality in pilot areas.
Ethiopia has deployed 40,000 volunteer village health leaders for home visits to ensure continuity of care
Another major intervention is the E-MOTIVE bundle for postpartum haemorrhage, the leading cause of maternal death globally. Implemented in primary care settings, it has increased detection rates fourfold. “These are not parallel systems,” Altaye emphasised. “They are embedded within the national strategy and scaled through government structures.”
Community-level innovations are equally central. Ethiopia has deployed around 40,000 volunteer village health leaders who conduct home visits and ensure continuity of care, fostering trust and local ownership.

For Abiy Seifu Estifanos of Addis Ababa University, Ethiopia’s approach is defined by a “diagonal investment strategy” that simultaneously strengthens the health system while targeting high-impact interventions. This includes expanding surgical capacity, with over 200 health centres now equipped to perform caesarean sections and plans to scale further. Neonatal care is also being decentralised, with primary hospitals handling nearly half of all neonatal admissions.
A critical enabler has been data. Ethiopia has invested in integrated digital systems that track maternal and newborn outcomes from admission to discharge for real-time clinical decision-making. “Data is not just for retrospective analysis; it is a tool to save lives,” Estifanos said.
Services at primary level are largely free in Ethiopia. According to Dr Lidiya Tefera of the Gates Foundation, the country’s progress reflects a careful balance between donor support and increasing government ownership.
Ethiopia combines broad health system strengthening with targeted investments in high-impact innovations
“All investments must align with government priorities,” she said, cautioning against parallel systems that collapse when external funding ends. Ethiopia combines broad health system strengthening, including financing and supply chains, with targeted investments in high-impact innovations. Domestic commitment is growing through increased budget allocations and pooled funding mechanisms. “The gap needs to be addressed now,” Tefera added. “We cannot wait until 2030 for solutions.”
The Ethiopian experience offers a useful contrast to Kenya, where primary healthcare reforms are ongoing but uneven in implementation.
Kenya has made significant policy strides, including the establishment of the Social Health Authority and a primary healthcare fund. Like Ethiopia, Kenya has 107,000 Community Health Promoters (CHPs) and a tiered system. However, differences emerge at execution.
While Ethiopia delivers 80 per cent of services through primary care, Kenya’s system remains more hospital-centric, with patients bypassing lower-level facilities due to quality gaps. Community health systems are less deeply embedded, facing challenges with remuneration, supervision, and retention.
Kenya’s capitation-based approach aims to reduce out-of-pocket costs, but delays and stock-outs ruin patient experience
Infrastructure also diverges. Ethiopia’s extensive health post network and comprehensive primary care facilities reach rural populations. In Kenya, access is still constrained by distance, particularly in underserved regions.
Financing models differ too. Kenya’s capitation-based approach under the SHA aims to reduce out-of-pocket costs, but delays, stock-outs, and administrative bottlenecks undermine patient experience. Ethiopia’s largely publicly funded model, while also facing constraints, appears more streamlined at the point of care in many rural settings.
Perhaps most notably, Ethiopia’s emphasis on community ownership through volunteer networks has created a level of engagement that Kenya is still working to achieve.
The session underscored that there is no single blueprint for strengthening primary healthcare. However, Ethiopia’s experience highlights several critical principles: sustained political commitment, deep community engagement, integration of innovation into national systems, and simultaneous investment in both infrastructure and outcomes.