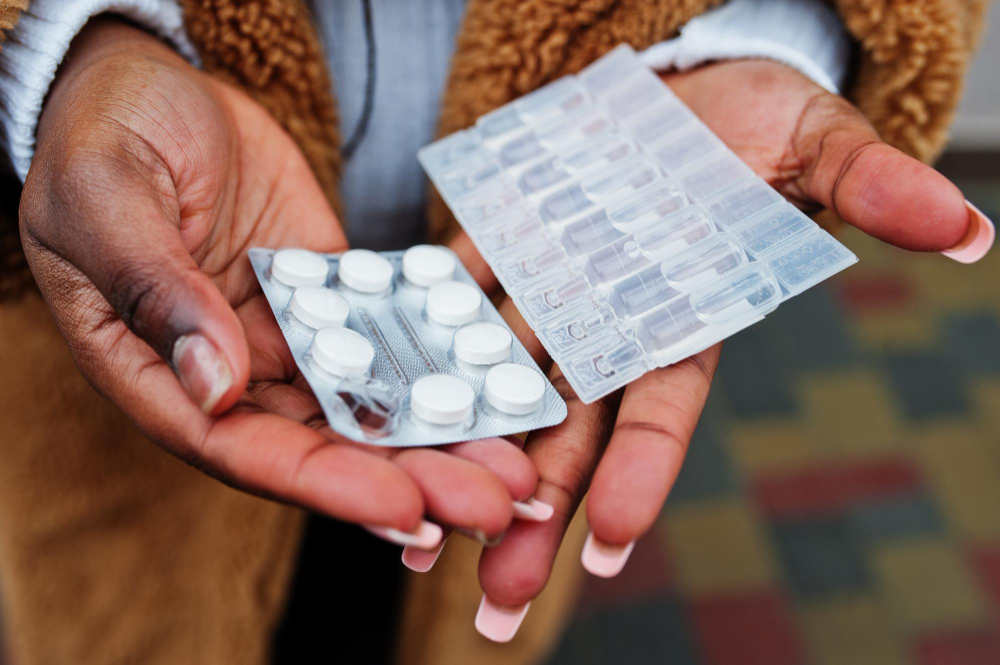
Antimicrobial resistance kills over one million people each year, but weak rules on prescriptions and easy access to self-medication are making the crisis worse.
When Dr John Kariuki, a veterinary surgeon, fractured his hip after a fall at home, his path seemed predictable: surgery, recovery, rehabilitation. Instead, it marked the beginning of a prolonged and life-altering encounter with antimicrobial resistance (AMR), a threat steadily undermining modern medicine.
After surgery, his wound failed to heal. Weeks passed, then months. Pain intensified, and persistent discharge signalled an infection that refused to respond to treatment. He was admitted multiple times, placed on different antibiotics, and subjected to repeated procedures. None worked.
A laboratory culture test eventually revealed the cause: the bacteria infecting him were resistant to almost all available drugs. Out of 18 antibiotics tested, only one remained effective.
Dr Kariuki survived, but with permanent consequences: extended hospital stays, heavy antibiotic exposure, and lasting disability. His experience illustrates a growing reality: once manageable infections are becoming increasingly difficult, and sometimes impossible, to treat.
Just what is Antimicrobial resistance?
Antimicrobial resistance occurs when bacteria, viruses, fungi and parasites evolve and stop responding to medicines used to treat them. The result is dangerous: infections persist, spread more easily, and become more likely to cause severe illness or death.
According to the World Health Organisation (WHO), AMR is already associated with an estimated 4.9 million deaths globally each year. If trends continue, this could rise to 10 million annually by 2050.
Yet as Prof Rodney Adam, Consultant Infectious Disease Specialist and Molecular Pathologist at the Aga Khan University Hospital, explains, the threat often remains invisible until a patient actually needs treatment. “You’ll never know about it until you need an antibiotic,” he said. “And when you do, the usual ones may not be effective.”
He describes AMR as a universal risk. “There’s a lot of reason to worry about it because it affects us all. We are more likely to have resistant bacteria now than before.
When treatment stops working: E. coli bacteria are resistant 60 per cent of the time
For clinicians, AMR becomes most visible when treatment does not work as expected. Prof Adam notes this extends beyond infections to procedures that depend on antibiotics for safety.
“Even for many kinds of surgery, there is prophylaxis: antibiotics given to prevent infection. That may not work as anticipated,” he explained. “You can have a condition that should be treated, but there is no good treatment available.”

In Kenya, numbers from the national surveillance data from 2025 are worrying. Take MRSA, a dangerous bacterium that causes wound infections. In 2023, 43 out of 100 people with this infection could not be treated with standard antibiotics. By 2025, that number jumped to 51 out of 100.
E. coli bacteria are resistant 60 per cent of the time. Imagine a woman who gets a urinary tract infection (UTI). For 60 out of every 100 women like her, the standard antibiotic used to treat UTIs will fail. Then there is Klebsiella pneumoniae bacteria, which are resistant 75 per cent of the time. If a newborn baby in a hospital catches pneumonia, for 75 out of every 100 babies like this, the first-choice antibiotic will do nothing.
The same goes for Acinetobacter bacteria, which are resistant 75 per cent of the time. Take a car crash victim on a breathing machine who develops a lung infection. For 75 out of every 100 patients like this, doctors have no simple antibiotic that works.
Prof Adam, who has worked in Kenya for over a decade, says the scale of local resistance is striking. “When I came here about 15 years ago, I was shocked by the level of resistance. Even today, it is much greater than what is being seen in North America and Europe.”
He points to a critical consequence: the loss of simple treatment options. “Very often, we have no oral antibiotics that will work. The only effective ones are intravenous, and they are expensive.” This creates barriers not only for patients but for the entire health system, particularly in resource-limited settings.
How resistance spreads: Upper respiratory tract infections shouldn’t be treated with antibiotics
While resistance develops naturally, human behaviour has significantly accelerated the process. Prof Adam identifies overuse of antibiotics, especially in outpatient settings, as a major driver.
“There is so much overuse of antibiotics on the outpatient side,” he said. “Almost never should upper respiratory tract infections be treated with antibiotics, yet it happens frequently.”
He describes a dual pressure: clinicians prescribing antibiotics to meet patient expectations, and patients demanding medication even when unnecessary. “We really have two sets of barriers. Doctors feel pressure to give antibiotics, and patients often expect them. If they don’t get them, they may go elsewhere.”
“Probably more than 90 per cent of those who are treated shouldn’t be,” Prof Adam said, referring to certain outpatient antibiotic use. “It’s much harder to convince people they don’t need antibiotics than to just give them.”
One common belief is that stopping antibiotics early causes resistance. Prof Adam challenges this directly. “That’s a common myth. The real problem is using antibiotics when they are not needed.” Keeping leftover antibiotics and using them later for unrelated illnesses, he explains, contributes more significantly to resistance.
Everyday conditions at risk: Some bacteria can be transmitted between animals and humans
AMR is already affecting the treatment of routine conditions: urinary tract infections, where resistance is increasingly high; pneumonia, which may require hospitalisation due to treatment failure; and sexually transmitted infections such as gonorrhoea, where options are narrowing.
“We’re running out of drugs for treating some of these infections,” Prof Adam said.
The problem extends into agriculture. “There are bacteria that can be transmitted between animals and humans,” he said. “If animals are given antibiotics, they are more likely to carry resistant bacteria.”
The larger concern, he emphasises, is not antibiotic residues in meat but the widespread use of antibiotics for growth promotion in livestock. “That’s a huge amount of antibiotic use. It likely contributes to resistance in the general population.”
A crisis with many drivers: In neonatal units, drug-resistant infections are particularly deadly
During the launch of World AMR Awareness Week 2025, Dr Emmanuel Tanui, Kenya’s National AMR Focal Point, stressed that AMR is already causing over one million deaths annually. “Low- and middle-income countries carry the greatest burden due to weak health systems, limited diagnostics, and poor access to effective antimicrobials,” he said.
Dr Loice Ombajo, an infectious disease specialist at the University of Nairobi, notes that resistance to ceftriaxone, a key hospital antibiotic, now exceeds 60 to 70 per cent, significantly narrowing treatment options. In neonatal units, drug-resistant Klebsiella pneumoniae infections are particularly deadly, with some outbreaks leading to extremely high mortality.
Dr Saumu Wayuwa, a paediatrician from Mombasa County, identifies self-medication as a major contributor, with patients often accessing antibiotics directly from pharmacies. Prof Sam Kariuki of the Drugs for Neglected Diseases Initiative describes AMR as one of the world’s deadliest but least visible health threats, noting that prevention through hygiene and vaccination can reduce the need for antibiotics entirely. “When people don’t get infected, they don’t need antibiotics. That alone slows resistance.”
Diagnosis, policy, and what lies ahead: Kenya has a National Action Plan on AMR
A key challenge in managing AMR is distinguishing infections that require antibiotics from those that do not. Prof Adam emphasises the need for proper laboratory testing. “The most common scenario is that there wasn’t an infection requiring antibiotics in the first place. That’s why a good laboratory workup is important.”
Kenya has a National Action Plan on AMR covering 2023 to 2027, focusing on surveillance, infection prevention, and responsible antibiotic use. Enforcement, however, remains inconsistent. “I was here for years before realising that a prescription is required for antibiotics,” Prof Adam said. “That regulation exists, but it is not enforced.”
The long-term implications are stark. “If antibiotics become ineffective, we are back to 100 years ago,” Prof Adam warned. “Simple infections, surgeries, childbirth: these all become high-risk.”
From hospital wards to community pharmacies and farms, AMR is being driven by everyday practices. It is no longer a future risk. It is a present and growing crisis.