From antibiotics to opioids, Kenya’s unregulated drug market is engineering its own health emergency.
Across Kenya, a silent pandemic is unfolding, not in the sterile wards of hospitals, but over the counters of retail pharmacies, unlicensed chemists, cosmetic shops, and even local supermarkets.
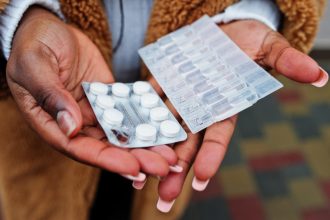
Potent antibiotics like Amoxiclav, painkillers such as Betapyn (which contains the addictive opioid codeine), and psychiatric medications like Diazepam are all available without a prescription. No doctor. No diagnosis. No questions asked.
This ease of access has quietly normalised a culture of self-diagnosis and drug misuse that is now threatening to become one of Kenya’s gravest public health emergencies.
At the heart of the problem is the commercialisation of healthcare. Many community pharmacies operate as retail businesses first and clinical outlets second. When daily survival depends on turnover, a prescription becomes an obstacle to a sale. Pharmacists are caught in an impossible position: uphold professional integrity or keep the lights on.
While proponents frame over-the-counter (OTC) access as a practical workaround for expensive consultations and overcrowded hospitals, it is a dangerous façade hiding three distinct, deeply connected crises.
When patients self-medicate, they take the wrong drug, wrong dose, for the wrong duration
The unregulated sale of antibiotics is the primary engine driving Antimicrobial Resistance (AMR), one of the most serious long-term threats to global health. In proper clinical practice, a Culture and Sensitivity (C&S) test identifies exactly which antibiotic will work against a specific infection. When patients self-medicate, they skip this step entirely, often taking the wrong drug, at the wrong dose, for the wrong duration.
A 2020 study by Maina, Mwaniki, Odira, and colleagues, published in BMC Public Health, found that self-medication with antibiotics was both widespread and poorly understood in Nairobi’s informal settlements. Community pharmacies were routinely dispensing antibiotics for viral infections like the common cold, where they are completely ineffective, and often providing only a few tablets at a patient’s request, far below a therapeutic dose.
Incomplete treatment is a classroom for bacteria. Weak strains die; resilient ones survive, adapt, and multiply, eventually developing defences that standard treatments can no longer overcome.
The human cost is tangible: a mother buys three Ciprofloxacin tablets from a local kiosk for her child’s fever. The child improves briefly, then deteriorates. By the time they reach a hospital, the child has a drug-resistant strain of typhoid requiring expensive injectable drugs, a far heavier burden than a single clinic visit would have been.
Kenya has a prescription drug problem. It is less visible than illicit drug abuse, but the consequences are just as devastating.
Prescription meds, available cheaply without oversight, are feeding addiction
A 2024 study by Kuria, Kiburi, Ochieng, Mburu, and Owiti, published in PLOS Mental Health, examined substance use patterns among patients on methadone treatment at a referral hospital in Nairobi. The findings were stark: opioid dependency in Kenya is not confined to street drugs. Prescription medications, available cheaply and without oversight, are feeding the same cycle of addiction.
Codeine, found in widely available products like Betapyn, is metabolised into morphine in the liver. Without medical supervision, tolerance builds quickly, and withdrawal becomes physically unbearable. The user is no longer taking the drug for pain relief; they are taking it to feel normal.
In urban centres, pill-shopping has become routine among young adults. A university student begins taking Betapyn for tension headaches. Within months, they are buying multiple packs a week to stave off withdrawal rather than manage pain. Academic performance collapses, and financial desperation follows.
Benzodiazepines like Diazepam follow the same pattern, intended for short-term use under clinical supervision but consumed without any monitoring. The open availability of these substances is quietly fracturing families and communities across Kenya.
Informal drug transactions leave no paper trail. Without a prescription and a licensed pharmacist verifying stock, the supply chain becomes porous. Research by Ochieng and colleagues (2024), published in Frontiers in Tropical Diseases, found that East Africa remains a key target for counterfeiters introducing inactive or toxic substances into the pharmaceutical supply.
Medicine may contain chalk or harmful contaminants like diethylene glycol
In chemists operating without a resident superintendent pharmacist, nobody is checking batch numbers, expiry dates, or wholesale origins. Medicine may contain nothing more than chalk or, in more dangerous cases, harmful contaminants like diethylene glycol. The patient has no way of knowing. They are gambling with their life.
The solution goes beyond crackdowns. It requires a structural rethink of how Kenya funds and delivers healthcare.
The Pharmacy and Poisons Board (PPB) must evolve from a reactive regulator into a proactive enforcement force. The 2023 Annual Regulatory Compliance Report acknowledged a systemic gap in rural inspections. Closing that gap requires a national e-prescription system linking every dispensed medicine to a registered clinician and a unique patient identifier, replacing anonymity with accountability.
Penalties under the Pharmacy and Poisons Act (Chapter 244) must also be overhauled. Nominal fines are not a deterrent. Persistent offenders should face permanent license revocation, and the illicit distribution of controlled substances should be prosecuted as a criminal matter.
Enforcement alone, however, will not solve this. The informal drug market thrives because the formal system is too expensive and too inaccessible for millions of Kenyans. Self-medication is, for many, a survival strategy born of economic necessity rather than ignorance.
Chronic misuse of paracetamol-codeine can trigger acute liver failure
The most powerful intervention is therefore a well-funded primary healthcare system. As Njoroge and colleagues established in 2022, when primary care is insurance-backed and affordable, patients choose the professional pathway because it becomes the easiest one. Strengthening Universal Health Coverage (UHC) through the Social Health Insurance Fund (SHIF) would remove the financial barrier driving people to the chemist counter in the first place.
According to “Approaches to implementing and financing primary health care in Kenya: A case of seven counties” by Karimi and fellow researchers published in BMJ Global Health in 2025, shows that when primary healthcare is well funded and insured, people are more likely to go to trained health providers.
When consultation fees are removed, formal care becomes the easiest and cheapest option. By covering outpatient costs through approaches like capitation, the system reduces the need for self-treatment, making professional diagnosis the normal choice for everyone.
There is also a cultural dimension. The “Prescription-Only” label is widely treated as a suggestion rather than a safeguard. Public education must reframe this clearly: these restrictions exist because potent medicines, taken without proper guidance, cause serious harm.
Chronic misuse of paracetamol-codeine combinations, for instance, can trigger acute liver failure, a lethal outcome from a medicine sold casually over a shop counter.
Selling prescription-only medication over the counter in Kenya is a game of Russian roulette. While it may save a few hundred shillings today, the long-term cost, measured in superbugs, addiction, counterfeit poisonings, and preventable deaths, is one the nation cannot afford.
Medication without professional guidance does not cease to be medicine. It becomes a poison, sold with a smile and no receipt.
It is time to return these tools to the hands of professionals trained to use them, and to build a health system that makes doing so the easiest, most affordable choice for every Kenyan.
Dr Madeline Iseren is a pharmacist and commentator on topical medical and health issues.