The surgical team performed the first total facial skeleton resection, reconstruction and rehabilitation in the world for free, but the custom titanium implants for Lucy Gathoni’s surgery were imported from Belgium and cost Ksh6.8 million.
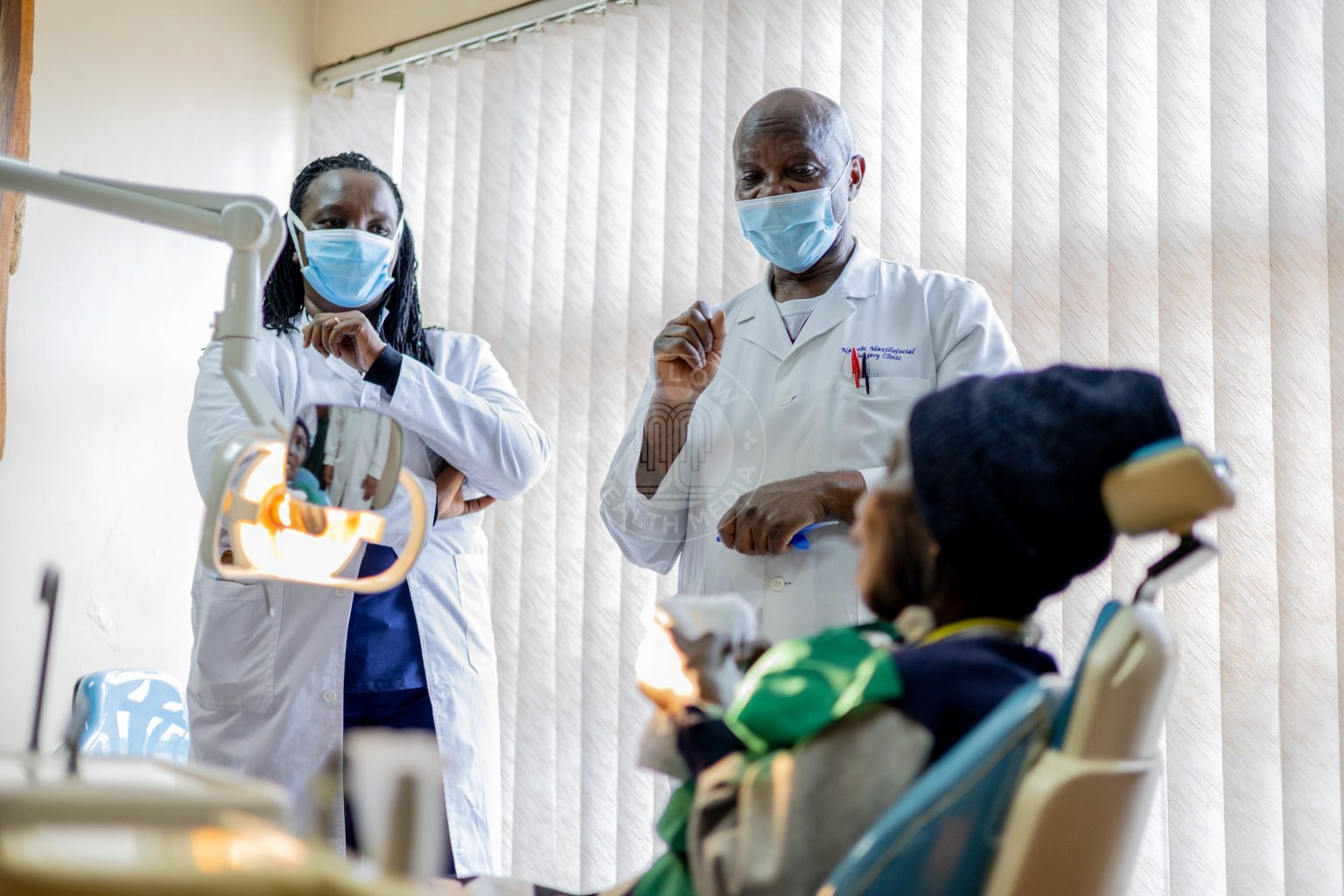
Behind closed doors of the operating theatre at Nairobi Hospital, a surgical team is attempting a medical first ever documented for Kenya and Africa: Rebuilding a face. Not repairing. No, rebuilding the 29-year-old face of Lucy Gathoni.
It all started with a small swelling on Lucy’s jaw. She was 12. They didn’t think much of it. But it shortly began to grow. It had to be removed. See, for 17 years, Lucy struggled with the growing tumour that limited her speech and massively distorted her face.

Medics at Othaya Subcounty Hospital referred Lucy to Nyeri Provincial General Hospital (PGH), but “Every time it was removed, it grew back bigger,” recalls her mother, Peris Mwaura.
The swelling grew, distorting her jaw, stealing her breath, eventually erasing the face she was born with. “We initially thought it was cancerous,” says her uncle, James Mwaura.
The tumours were benign, and the relief that came with negative cancer results was short-lived as the growth was such that “I cannot breathe well,” Lucy said at the family’s Othaya home.
“I breathe through the mouth. I eat soft meals,” she told Willow Health Media in January, 2025. The operation was in April. Willow has been documenting her surgery journey ever since, in a medical case riddled with escalating and disrupted domestic life.
In 2017, Rev Fr Joseph Waithaka walked into Lucy’s life and refused to walk out
“My marriage was affected because of Lucy’s illness,” says her mother. “Her father said we should leave his home because they don’t have sick people where he comes from. He left in 2008 and has never returned.”
Single, broke and asthmatic, Peris carried the weight alone. “It stresses me,” she says. “I ask God for strength. I have to be strong for my child. What else can I do?”
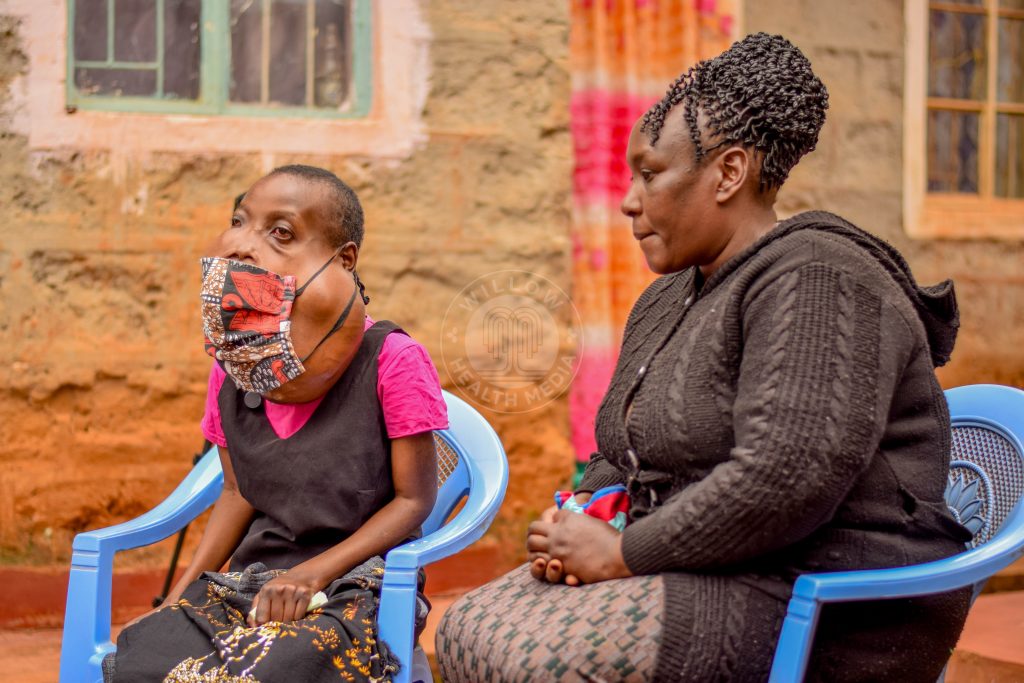
But in 2017, Rev Fr Joseph Waithaka walked into Lucy’s life and refused to walk out. “Lucy is my friend,” says Fr Waithaka. “I saw her condition, and I requested to see the background, then we organised a harambee. I met Prof Symon Guthua and explained to him. We made a decision to assist Lucy.”
They also reached out to Dr Margaret Mwasha, a prosthodontist, and brought Lucy’s case to Archbishop Anthony Muheria, who approached the Nairobi Hospital through Prof Guthua.
Prof Guthua explains the magnitude was what was at stake as “Nobody has done this, so we want to make sure that we do it the right way and reconstruct her back.” Lucy’s small body frame also meant “There’s no place you can start going for bones to reconstruct her. It’s not there. Right? And you make her even weaker. You make her disabled. So, we have patient-specific implants made according to how she is now.”
The hospital’s Director of Medical Services and Research, Mr Samuel Odede, remembers the challenge of “Trying to get the funds to perform this corporate social responsibility, but we managed.”
Digitally mapping and isolating the exact shape of the patient’s skull and bone
But first, the surgical team needed custom-made titanium implants to reconstruct her face. These alone had to be flown from Belgium and designed specifically for Lucy’s reconstructed face. It cost Ksh5 million. Next came planning the surgery, “A gruelling 18 hours, pro bono, bless them,” Odede says. “These are our true heroes and heroines.”

The surgery was Lucy’s fifth and, if successful, would be her last. The surgical team guided her through the surgery using a 3D model, detailing each cut and reconstruction, her mother absorbing every word.
Michael Mwasha, the biomedical engineer behind the implant’s designs, explains how the process starts by digitally mapping and isolating the exact shape of the patient’s skull and bone. Next, the damaged or diseased portion of bone is virtually identified and removed from this digital model. Finally, a custom implant is designed and created to precisely fit the space left after the virtual removal.
Though Kenya produces raw titanium in Kwale and Kilifi, it cannot manufacture the complex medical implants required. The titanium plates were thus engineered and sent from Belgium. Base Titanium recently completed its final bulk shipment in February 2025, ending eleven years of mining operations after depleting ore reserves.
Operating theatre filled with rhythmic clinking as specialists moved with precision
Her mother, Peris Mwaura, sits gazing blankly in the waiting bay, eyes fixed on the doors that opened up for her second-born daughter. The surgery took place after morning prayers on Good Friday, April 18, 2025.
8:35 am: The surgeons made the first incision.
But the size of the tumour caused breathing challenges as “We could not contain her airway,” said the anesthesiologist, Dr Kinyua Gathukia. “The whole face was disfigured. Airway was a primary problem.”
9:00 am: They had performed a tracheotomy, inserted feeding and urinary tubes, and sterilised her skin. With eye drops applied and surgical lines marked on her face, the stage was set for the marathon surgery.
9:55 am: The theatre was filled with the rhythmic clinking of instruments and the steady beeping of machines. Each specialist moved with precision.

The upper jaw tumour, 1.1 kgs, came out first. It had been pressing against Lucy’s cranial base. Then out came the larger one from the lower mandible, a 2.2 kg tumour. The third was smaller but significant and added to the horror. Combined, the tumours weighed 3.3kgs roughly 10 per cent of Lucy’s entire body weight.
For perspective, imagine carrying a newborn baby attached to your face.
Together, the tumours distorted both her upper and lower jaws, a complexity no Kenyan surgeon had faced before.
3:40 pm: All the tumours were out.
When the final mass was lifted from Lucy’s face, the operating room erupted in applause. But the hardest work was just beginning.
Upper tumour had grown into her skull base, the lower one was a dense web of blood vessels
Prof Symon Guthua led the resection. Dr Mwasha guided the placement of Lucy’s prosthesis. Both jaws were reconstructed using patient-specific implants designed through virtual resections and 3D modelling.
“Usually, the tumour affects only one jaw,” explained Prof Guthua. “But here, it was both, and the growth was highly complex.”
The upper tumour had grown into her skull base. The lower one was a dense web of blood vessels, posing a severe bleeding risk. “That was something that worried us,” Prof Guthua recalls. “But we were able to control the bleeding.”
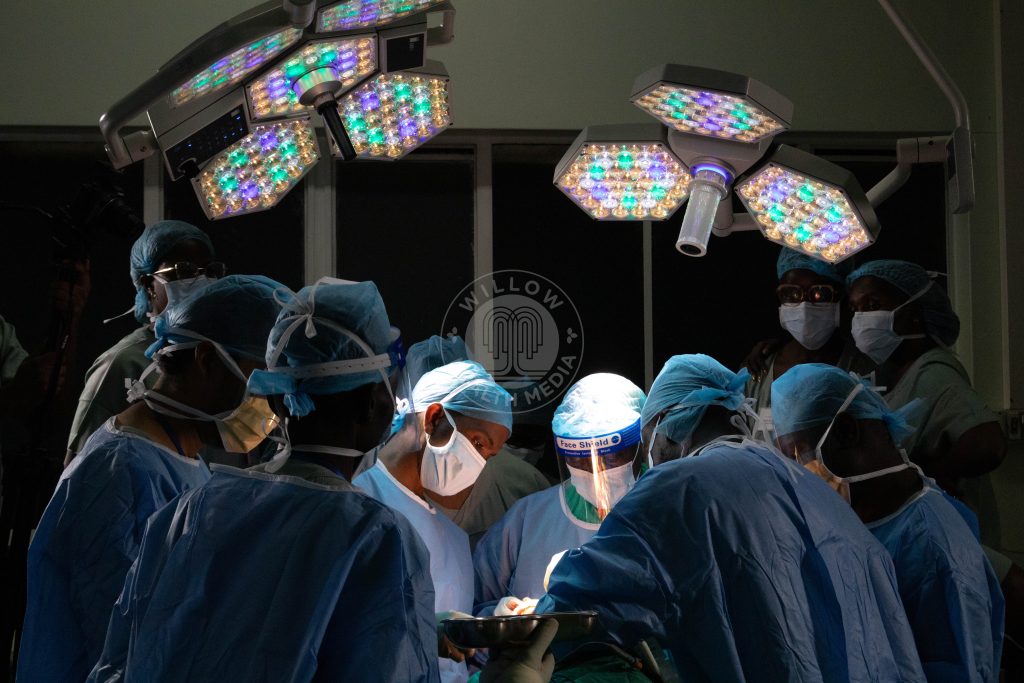
5:15 pm: The reconstruction began as surgeons inserted titanium plates into the left upper jaw first, then the right. They placed the upper denture and secured it with screws. Then the mandible.
Late into the night, they closed the incisions and wired her jaw shut. This stabilised the new titanium framework and allowed her facial muscles to reattach properly.
1:20 am, Saturday: 18 and a half hours later, Lucy’s head was wrapped in gauze.
1:40 am: Lucy was wheeled out of the operating theatre.
This was a historic surgery. Only one other person in the world had ever come close. The patient had received a complete lower jaw replacement. And that design was different.
Prof Guthua’s version included special attachments where Lucy’s jaw muscles could grip and move the new titanium bone. Every detail was designed to last, to move smoothly, to work with her body. Every cut, every stitch, every placement of the titanium plates had to be perfect.
“It’s about changing one patient at a time,” Dr Mwasha says quietly. “Really, the whole life. Because she’s a young lady who has struggled. Breathing was interfered with, feeding had been interfered with, and how she looks. It has interfered with the quality of her life.”
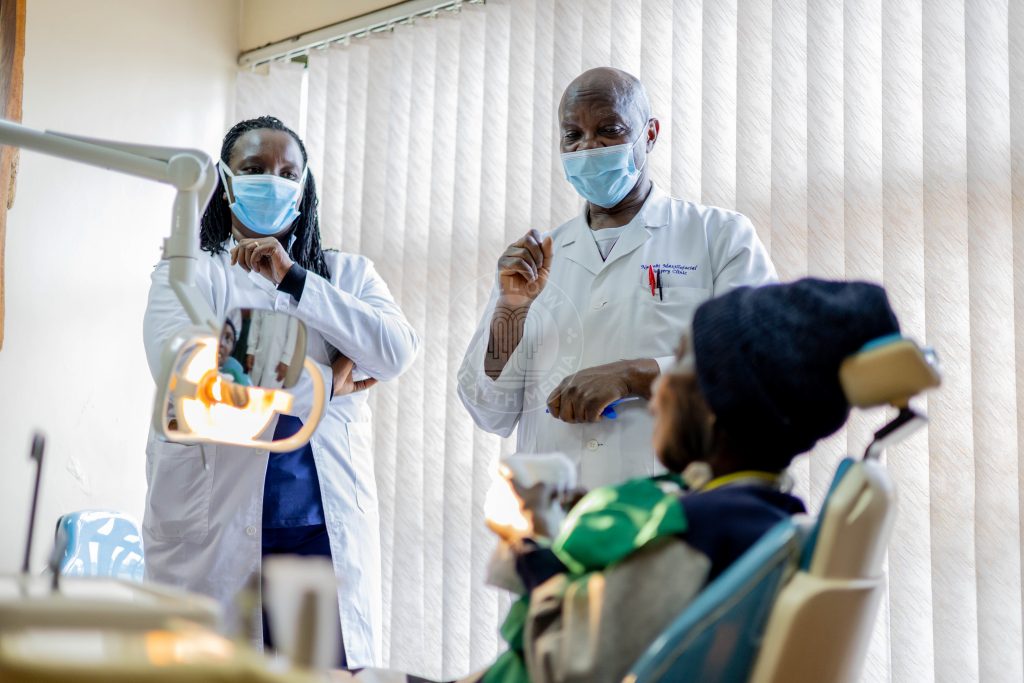
Her jaw was rebuilt, though still fed by a tube, she was finally gaining weight
After a two-day recovery in the ICU instead of the expected four, Lucy remained in the hospital for another two weeks before discharge.
At her first review, Prof Guthua handed her a mirror, revealing her new face. The tumour that had defined her was gone, her jaw was rebuilt, and her muscles were working. Though still fed by a tube, she was finally gaining weight.
Her transformation was so profound that she will likely need a new national ID or identification documents. The face in the mirror is no longer the face on her documents.
Friends remember the cheerful cashier Lucy once was, hidden behind her burden. Now, they dream with her.

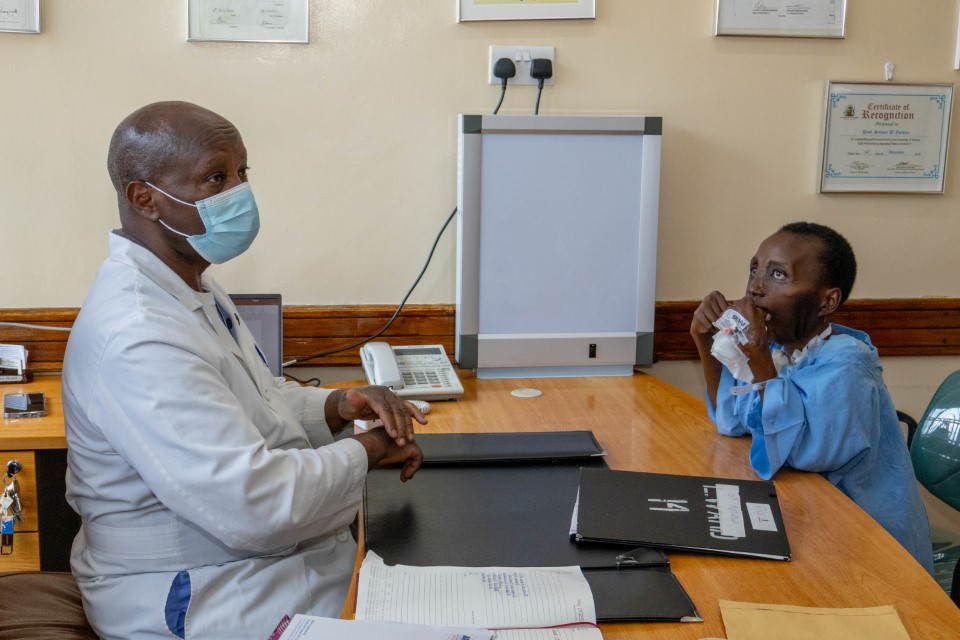
Lucy Gathoni is now learning to live in a body that finally feels like her own
Susan Wamaitha from her church longs to see Lucy’s full smile and potential restored, since at 29, “She is still young, has her whole life ahead of her.” Her best friend Peninah Mugure laughs as Lucy shares new dreams of travel, to the US, to everywhere, and a simple, normal life.
A normal life. Such a small phrase for such an enormous dream.
In Kenya today, while the Social Health Authority now covers the surgical procedure itself for complex cases like Lucy’s maxillofacial reconstruction, including hospital admission, ICU care, and anaesthesia under specialised tariffs reaching up to 392,000 shillings, a critical gap remains. The patient-specific titanium implants essential for facial reconstruction, valued at 5 million shillings and flown in from Belgium, fall outside SHA coverage. This forces families into fundraising through harambees and community support.

Lucy’s life-changing surgery only became possible through extraordinary circumstances: the Catholic Church under Archbishop Anthony Muheria’s leadership, over 20 specialists at Nairobi Hospital donating their expertise, and an 18-and-a-half-hour operation performed entirely pro bono. Her case highlights both the promise of universal health coverage and the sobering reality that for the most critical interventions, Kenyans still depend on charity and goodwill rather than guaranteed access to care.
Lucy Gathoni is now learning to live in a body that finally feels like her own. She is learning to eat without pain, to breathe without a struggle and look in the mirror without flinching.
She is also appreciating that miracles happen even where medicine, faith, and engineering are needed the most.
“We are not yet there, but we believe with God’s grace and guidance, we shall be there,” said Fr Waithaka.
Lucy isn’t there yet, but she’s walking toward it one reconstructed step at a time. “I am so happy. I will invite you to a Thanksgiving Mass. And you must come and celebrate with me,” she told the Willow Health Media team during a post-surgery shoot in Othaya, where she continues her recovery, surrounded by family, faith and the second chance at life, with a new face.
















This is an inspiring, touching story.
This is an inspiring, touching story. Yes, we can!