The convergence of political will, financing reforms, digital tools and local manufacturing capacity strategically positions the continent for transformation and reduced dependence on external aid.
Africa’s push to manufacture its own medicines, secure sustainable health financing and translate data into real community impact took centre stage at the World Health Summit Regional Meeting (WHSRM) 2026, which opened in Nairobi on Monday with a forceful call to end the continent’s dependence on external health systems.
The summit brings together more than 2,000 global health leaders, policymakers, researchers and development partners under the theme Reimagining Africa’s Health Systems: Innovation, Integration and Interdependence. Speakers were united in one message: Africa must stop being a spectator in global health discussions and become the architect of its own solutions.
President William Ruto, while officially opening the summit, put the crisis in blunt terms.

“We remain heavily dependent on external supply chains for essential commodities such as medicines and vaccines, producing less than two per cent of what we consume,” he said. That dependency, he warned, leaves Africa exposed during global disruptions and weakens its ability to respond to health emergencies, a lesson the Covid-19 pandemic drove home painfully.
The statistics framing the summit were stark. According to the World Health Organization (WHO), Africa accounts for over 20 per cent of the global disease burden, amounting to more than 629 million disability-adjusted life years (DALYs) lost, while representing less than three per cent of global health expenditure.
The continent bears 94.5 per cent of global malaria cases and 40 per cent of the burden of neglected tropical diseases. Acute respiratory infections, HIV/AIDS, diarrhoea, malaria and tuberculosis account for nearly 80 per cent of the continent’s infectious disease load.
A recurring theme was the urgent need to build local manufacturing and research capacity. President Ruto called for increased investment in biotechnology, genomics and vaccine development, arguing that the continent must stop importing solutions it has the potential to create.
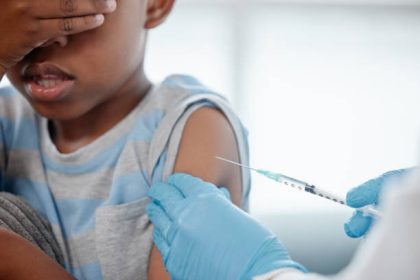
Africa’s inability to manufacture its own vaccines resulted in delayed access and preventable Covid-19 related deaths
“Africa must position itself at the forefront of biotechnology and advanced research, thereby transitioning from a consumer of innovation to a producer of globally relevant solutions,” he said.
Professor Lukoye Atwoli, International President of WHSRM and Dean of the Medical College East Africa at Aga Khan University, framed the moment as a turning point for African-led health research and policy.

“For too long, Africa has been the subject of global health discussions held elsewhere by others. African institutions, researchers and policymakers are not consumers of global health policy; we are its co-authors,” he said.
Leaders drew sharp lessons from the Covid-19 pandemic, noting that Africa’s inability to manufacture its own vaccines resulted in delayed access and preventable deaths. Strengthening regional supply chains and reducing inequities in medicine access were identified as non-negotiable priorities going forward.
Beyond production, sustainable financing emerged as a critical pillar of discussion. Africa carries over 20 per cent of the global disease burden while accounting for less than three per cent of global health expenditure, a gap experts described as neither sustainable nor acceptable.
“This imbalance is neither sustainable nor tenable,” President Ruto said, calling for “a decisive and deliberate shift, financed through both domestic and international capital.”
He pointed to Kenya’s own reforms as a working model. The establishment of the Social Health Authority, launched in 2024 to expand Universal Health Coverage, has already seen nearly 30.7 million Kenyans register for coverage. The government has also mobilised Ksh169 billion across key health funds, a demonstration, Ruto argued, of how domestic financing can drive systemic change.
Financing reforms must be paired with strong primary healthcare systems
Dr Jean Kaseya, Director General of Africa CDC, reinforced the urgency of financial self-reliance. “Africa’s health security and sovereignty depend on our ability to finance and build resilient systems at scale,” he said, adding that the summit presents a platform to “mobilise investment, strengthen partnerships and advance African-led solutions.”
Dr Mohamed Yakub Janabi, WHO Regional Director for Africa, stressed that financing reforms must be paired with strong primary healthcare systems. “The themes being discussed are deeply interconnected and will result in a blueprint for a new Africa by building a coherent health ecosystem,” he said.

The consensus among leaders was clear: financing must shift from donor dependency to long-term, locally driven investment models that guarantee continuity, equity and resilience.
A third major pillar of the summit was the need to harness digital innovation and data systems to produce real-world health outcomes, with President Ruto highlighting Kenya’s investments in digital health infrastructure as a key enabler of transformation.
“Through sustained investment in digital health systems, we are integrating data, improving transparency and enhancing decision-making,” he said, stressing that data must directly influence service delivery, resource allocation and accountability.
“Effective health systems depend not only on infrastructure and personnel but also on reliable, real-time information,” he added.
Dr Sulaiman Shahabuddin of Aga Khan University acknowledged persistent challenges such as the digital divide but expressed optimism about the continent’s trajectory. “I see a sector more capable than ever, better positioned to integrate systems, harness technology and train the workforce needed for quality care,” he said.
Community Health Promoters reach individuals directly, enabling early detection, prevention and continuity of care at the household level
Leaders agreed that the value of data lies entirely in its application of connecting digital tools to frontline health services, and community-level impact is where the real work lies.
Throughout the summit, speakers were deliberate in anchoring every structural reform to its impact on ordinary people. President Ruto highlighted Kenya’s deployment of over 100,000 Community Health Promoters as a concrete example of building systems that reach individuals directly, enabling early detection, prevention and continuity of care at the household level.
Professor Axel Pries, President of the World Health Summit, framed the gathering’s purpose in direct terms. “Our role is to convene leaders and the goal is clear: to translate dialogue into practical action that strengthens health systems,” he said.
Dr Janabi described the meeting as a historic moment for continental collaboration. From reducing out-of-pocket costs to expanding medicine access in rural areas, the discussions repeatedly returned to a single test: does this reform change what happens to a patient in a community clinic?
The WHSRM 2026 closed its opening session with a mood of cautious but determined optimism. Speakers acknowledged that Africa has had many summits and many declarations, but insisted that the convergence of political will, financing reforms, digital tools and local manufacturing capacity makes this moment different.
The speakers unanimously agreed: Africa’s health future will be built at home through its own research, financed by its own systems and powered by data that delivers real impact where it matters most. The task now is to move from the language of intention to the architecture of implementation.