Many women feel powerless asking a man to use a condom, get tested for HIV or say no to sex without protection. Poverty, limited education and sexual violence only worsen the situation.
Women are disproportionately vulnerable to HIV infection, a reality driven by both biological factors and deeply entrenched social inequalities.
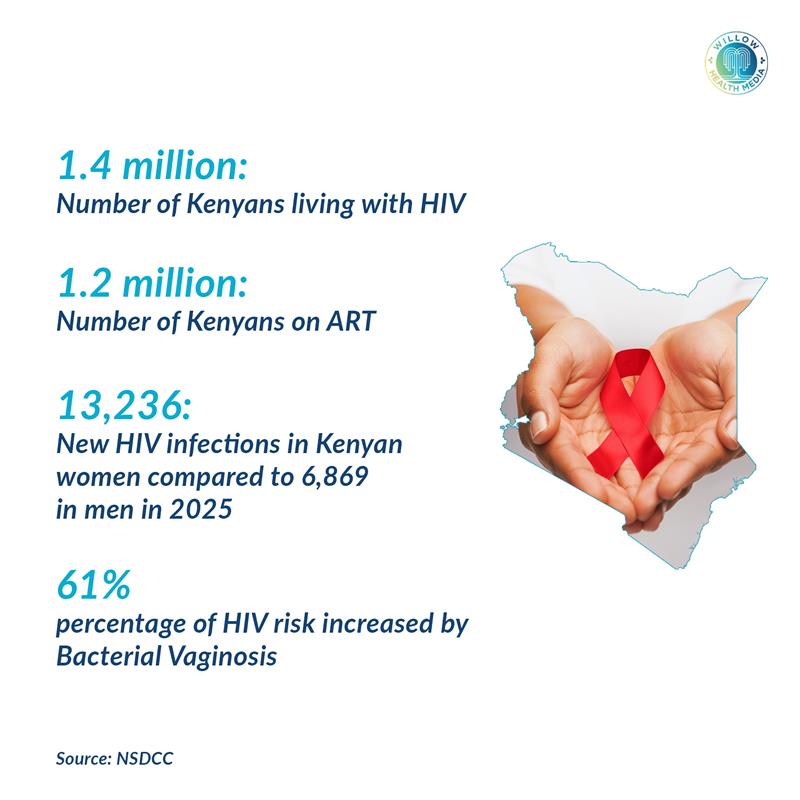
In Kenya alone, 2025 data from the National Syndemic Diseases Control Council (NSDCC) revealed that women accounted for nearly two-thirds of all new HIV infections. This reflects a global pattern where women are at a much higher risk of contracting HIV from heterosexual intercourse than men.
The disparity stems from a convergence of anatomical vulnerabilities and power imbalances that strip women of control over their sexual health. Understanding why requires confronting uncomfortable truths about both human biology and societal structures that perpetuate inequality.
The fundamental anatomical differences between male and female genitalia create inherent transmission disparities. The vaginal tract presents a vast, delicate mucosal surface area compared to the penis. When semen containing HIV is deposited during intercourse, it remains in contact with vaginal and cervical tissues for days, dramatically extending the virus’s opportunity to penetrate the mucosal barrier and locate its primary target: CD4 T-cells.
The cervix, particularly the transformation zone where different epithelial tissues meet, is densely populated with these immune cells that HIV specifically attacks. This concentration creates an efficient entry point for the virus.
Vigorous intercourse can cause microscopic tears that provide direct bloodstream access
The vaginal and cervical mucosa are thin and easily compromised compared to the tougher, keratinised skin of the penis exterior. Common conditions amplify this vulnerability.
Bacterial vaginosis, vaginal dryness from hormonal changes, menopause, or breastfeeding all cause inflammation that recruits more CD4 cells to the area, inadvertently creating a “welcome mat” for HIV. Even vigorous intercourse can cause microscopic tears that provide direct bloodstream access.
Research in sub-Saharan Africa has demonstrated that bacterial vaginosis is associated with a 61 per cent increased risk of HIV acquisition in women. Other sexually transmitted infections dramatically heighten risk. Ulcerative STIs like herpes, syphilis, or chancroid destroy protective barriers and create open sores. Non-ulcerative infections like chlamydia and gonorrhea trigger inflammation that draws vulnerable immune cells to infection sites.
The body’s hormonal fluctuations further elevate risk. Research has shown women are significantly more susceptible during pregnancy and the postpartum period, when dramatic hormonal shifts alter the vaginal microbiome, affect vaginal lining thickness, and change immune cell presence, all contributing to increased vulnerability.
While biology sets the stage, social structures often dictate the tragedy’s unfolding. For countless women, the greatest risk factor is not deliberate choice but pervasive power imbalances that leave them with limited agency over their bodies and health.
Transmission stems not from women’s ‘risky behaviour’ but from partners’ actions and social realities
Marriage offers no protection when gender inequality prevails. Women in patriarchal cultures frequently contract HIV from long-term partners whose undisclosed risk behaviours, combined with societal norms, deny women control over their sexual health. The transmission stems not from women’s “risky behaviour” but from partners’ actions and social realities that prevent negotiation of safer sex.
Gender Inequality and Power Dynamics: Deeply ingrained gender norms prevent women from negotiating condom use, demanding partner HIV testing, or refusing unprotected sex. When male partners refuse condoms, women’s “choice” to protect themselves often means refusing sex entirely, a decision that can trigger violence, abandonment, or loss of economic support.
Economic Vulnerability: Poverty and limited education force many young women into transactional relationships where older, wealthier men provide financial support in exchange for sexual favours. This power imbalance fundamentally prevents insistence on safer sex practices. Survival for the woman, and sometimes her family, depends on maintaining the relationship on the man’s terms.
Intimate Partner Violence: Sexual violence directly increases transmission risk through physical trauma and micro-tears. Women in abusive relationships are frequently isolated, unable to access health services, discuss HIV prevention, or carry medications like PrEP (Pre-Exposure Prophylaxis) without fear of blame, accusations of infidelity, or further violence. Fear of violence often forces women into unprotected sex.
Kenya’s 2025 statistics add to the burden of 1.4 million people already living with HIV in the country. Despite significant advances in treatment access (with over 1.2 million Kenyans receiving antiretroviral therapy) new infections persist at alarming levels, with women bearing the disproportionate burden.
Multiple factors contribute to this gender disparity, including biological vulnerability, gender inequality limiting access to resources and decision-making power, cultural pressures such as early marriage, and economic dependency, making women vulnerable to transactional relationships.
Addressing women’s HIV vulnerability requires holistic responses that tackle both biological realities and structural inequalities.
Female-Controlled Prevention: Oral PrEP and the dapivirine vaginal ring are transformative tools allowing women to protect themselves discreetly without partner permission, providing critical control over sexual health.
Economic Empowerment and Education: Investing in girls’ education and women’s economic opportunities breaks dependency cycles, giving women agency to negotiate safer sex, leave abusive relationships, and access health services.
Challenging Gender Norms: Societal-level interventions must shift patriarchal norms, promote open dialogue about sexual health, and dismantle stigma surrounding HIV and women’s sexuality.
Integrated Services: Recognising the deadly intersection of violence and HIV, health and support services must provide comprehensive care for women experiencing abuse, combining HIV prevention with intimate partner violence interventions.
Women’s disproportionate HIV susceptibility is not merely a scientific issue; it represents an urgent human rights and social justice crisis. The fight against HIV/AIDS for women is inextricably linked to the broader struggle for gender equality. When women gain equal power to control their bodies, finances, and health decisions, when societies truly value their autonomy, the unseen battle of disproportionate HIV risk will finally shift, paving the way for a healthier, more just world for all.
Dr Madeleine Iseren is a Pharmacist and an Essayist.