A key inclusion in the unit is a Kangaroo Father Care (KFC) suite where fathers can spend quality time with their premature babies as mothers rest.
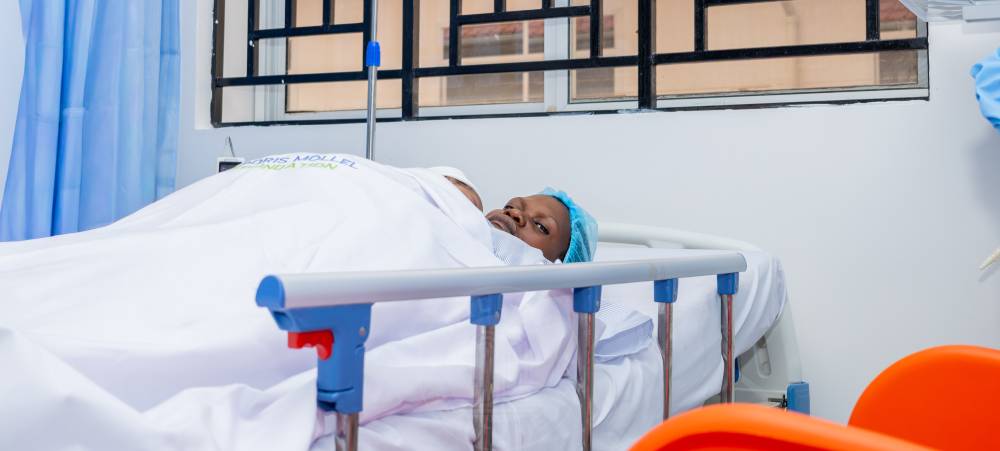
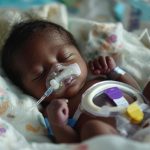
Gardensia Lucas Mayanzani sits on a plastic chair, gently rocking back and forth; her newborn baby quietly lying on her chest. The infant, one of a pair of twins born prematurely, weighing less than 1.5 kilograms, is nestled beneath a warm blanket.
His tiny heartbeat rises and falls against his mother’s, the rhythm of his fragile life synchronised with hers as she practices Kangaroo Mother Care; skin-to-skin contact that helps stabilise premature babies at the new Kwimba Neonatal Care Unit in Mwanza, Tanzania.

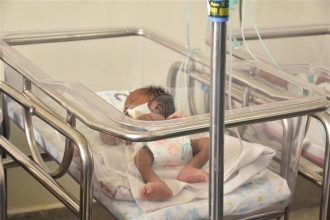
A few feet away, Mayanzani’s second twin rests in a small hospital cot covered with bright white sheets. He moves his limbs slowly as the soft blue glow of a phototherapy machine falls across his fragile skin, treating newborn jaundice without invasive procedures. Above him, a heating element provides warmth while a small temperature probe attached to his abdomen continuously monitors his body heat.
A few weeks ago, Mayanzani’s fate and that of her babies would have been completely different. Living in rural Mwanza means that the nearest referral hospital facility offering specialised care for premature newborns like hers was over 100 kilometres away in Bugando, an arduous two-hour journey through rough terrain, harsh rainy weather and possibly on a boda boda (motorcycle taxi), a desperate race against time.
Doris Mollel, a Tanzanian advocate, was herself born preterm at just 900 grams
But thanks to Doris Mollel, a Tanzanian advocate who herself was born preterm, weighing just 900 grams several decades ago, mothers and newborn babies in Mwanza, Tanzania, will now have access to faster, safer and more skilled health care following the opening of a fully equipped maternal and neonatal care unit in Kwimba District.

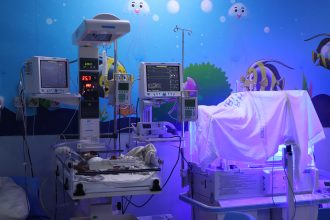
The hospital, which is the largest neonatal facility in Tanzania, is equipped with 15 specialised neonatal beds with incubators and warming equipment, Kangaroo Mother and Father Care suites, and a dedicated breastfeeding and nutrition support centre.
Speaking during the launch last week, Director for the World Health Organization (WHO) Africa Region, Prof Mohammed Janabi, described the facility as a “historic milestone” that could significantly reduce maternal and child deaths in a region long cut off from critical health care.
“Kwimba is the answer to a question we have asked for too long: how do we reach the unreachable?” Prof Janabi posed. “Not with grand policy alone, but with district-level infrastructure that puts care where the mothers are.”
Kwimba, like many districts in Tanzania, faces high maternal and neonatal mortality rates. The scale of the challenge is stark: of the about 18,073 babies born each year in the district, over 1,200 arrive with low birth weight, according to Deputy Minister of Health Dr Florence George Samizi. Until now, there has been no single neonatal intensive care bed in the entire district.
The mother travelled on a boda boda across rough terrain seeking emergency care
Families with struggling newborns often faced a desperate 100-kilometre journey along unpaved roads to the nearest Neonatal Intensive Care Unit (NICU) in Bugando. For many, that journey proved fatal.

Prof Janabi recounted a tragic case from 2006 involving a young mother in Mwanza who had just delivered a premature baby. The mother was forced to travel on a boda boda across rough terrain to seek emergency care, desperately clinging to her newborn. Tragically, the baby did not survive.
“Today, we have hope that things will improve with the new facility,” Prof Janabi said. “Our goal is to ensure that no family goes through what I witnessed in 2006. This facility is a blueprint for every rural community across Africa still waiting for its first NICU.”
Salome Malale, a Nursing Officer at the facility, said maternal and neonatal deaths in the region are driven by multiple factors, including lack of access to skilled care, delays in seeking treatment, and cultural beliefs that sometimes stigmatise mothers of premature babies.
Among the traditional Sukuma community, preterm babies and babies born in breech position were historically viewed as cursed, and “the mother and baby had to be cleansed immediately after birth in order to be accepted back in the community.”
Kwimba Neonatal Care Unit could save 1,300 premature babies annually
Such cleansing ceremonies often delayed hospital care and exposed both mother and baby to serious risk, sometimes resulting in complications or death.
The Kwimba Neonatal Care Unit (NCU) aims to end that deadly wait. Kwimba Member of Parliament Cosmas Bulala said the facility could save up to 1,300 premature babies annually who might otherwise not survive.
“It is the first patient-centred neonatal facility of its kind in Tanzania and is intended to serve as a replicable blueprint for district-level neonatal care across the continent,” he said.
Speaking during the launch, Doris Mollel said the facility was modelled on three premises: a parent-informed design whereby parents of premature infants helped shape the layout and model of care; a localised design around the realities of how families in Kwimba live and access care; and a zero separation care model where mothers and newborns remain together, enabling continuous Kangaroo Mother Care.
“It also has a Kangaroo Father Care suite where fathers can stay with their premature babies, as mothers rest,” said Mollel.
Community health workers from across the region receive on-site training in the facility. Outside, a solar-backed power system ensures uninterrupted care even during grid outages.
Neonatal deaths now account for nearly 40 per cent of all under-five deaths nationwide
The facility launches against a backdrop of significant but incomplete progress in child health. According to the Ministry of Health, Tanzania has reduced under-five mortality from 81 to 67 deaths per 1,000 live births between 2015 and 2022. However, neonatal deaths occurring within the first 28 days of life now account for nearly 40 per cent of all under-five deaths nationwide.
Mwanza region, home to more than 3.5 million people across eight districts, highlights these disparities. For years, specialised neonatal care has largely been concentrated in the regional capital, far from the rural communities where most births take place.
The Kwimba facility is the result of a partnership between civil society and the Tanzanian government. The Doris Mollel Foundation spearheaded the vision and fundraising, while Tanzania’s Ministry of Health provided regulatory support, land allocation, and a commitment to staff the unit with government-employed nurses and clinical officers.
For Mollel, who was born preterm of 900g and has long advocated for recognition of premature birth as a global health priority, the opening marks a turning point in her advocacy journey.
“I am proud of the collaborative work the Doris Mollel Foundation did hand in hand with the government in pushing for the recognition of World Prematurity Day as a WHO calendar day,” she said. Her vision for the day, marked annually on November 17, she says, “was to see every country in the globe marking the day by investment of care, making sure partners are mobilising enough funds, and that governments are capitalising national resources to invest in health care.”
Tanzania has included preterm birth in school biology and science curriculum
Other achievements made around reproductive health in Tanzania include the inclusion of preterm birth as a study unit in the school biology and science curriculum, and the provision of medical cover for preterm babies in the national health insurance scheme.
The Kwimba project has gained international support from partners like Keep A Child Alive, who view it as a key step toward fairer healthcare access.
During the launch, CEO Antonio Ruiz-Giménez Jr stressed this point: “KCA stands on the premise that no child should be left behind in accessing equal opportunity. This is not charity; this is justice.”
Ruiz-Giménez decided to support Mollel’s project after his own experience as a father of a preterm baby. He contributed an initial $95,000 and later over $600,000 to complete the unit.
We had a successful birth, yet for weeks, Benjamin was between life and death
He said his wife was rushed to the hospital for a preterm delivery. “We happened to be in New York under the best conditions, the best health care in the world. We had a successful birth. We had a lot of care, and yet for weeks, my son Benjamin was fighting between life and death,” he said.
“Every night that I was at that hospital, I could not stop thinking about the families that had to go through what I went through. My son Benjamin is very lucky to be here in this world, and I am very lucky to have him,” he said. “But right after that happened, walking out of the hospital, I said, ‘Doris, we’re going to build this unit together because every single family in Kwimba has the same right that I had in New York City for a safe and healthy delivery.”

Mollel said the ambition behind the Kwimba Neonatal Care Unit extends beyond the district itself. The facility is intended not only to serve the immediate community but also to act as a replicable model, demonstrating that district-level neonatal infrastructure can be built, staffed and sustained in rural African settings.