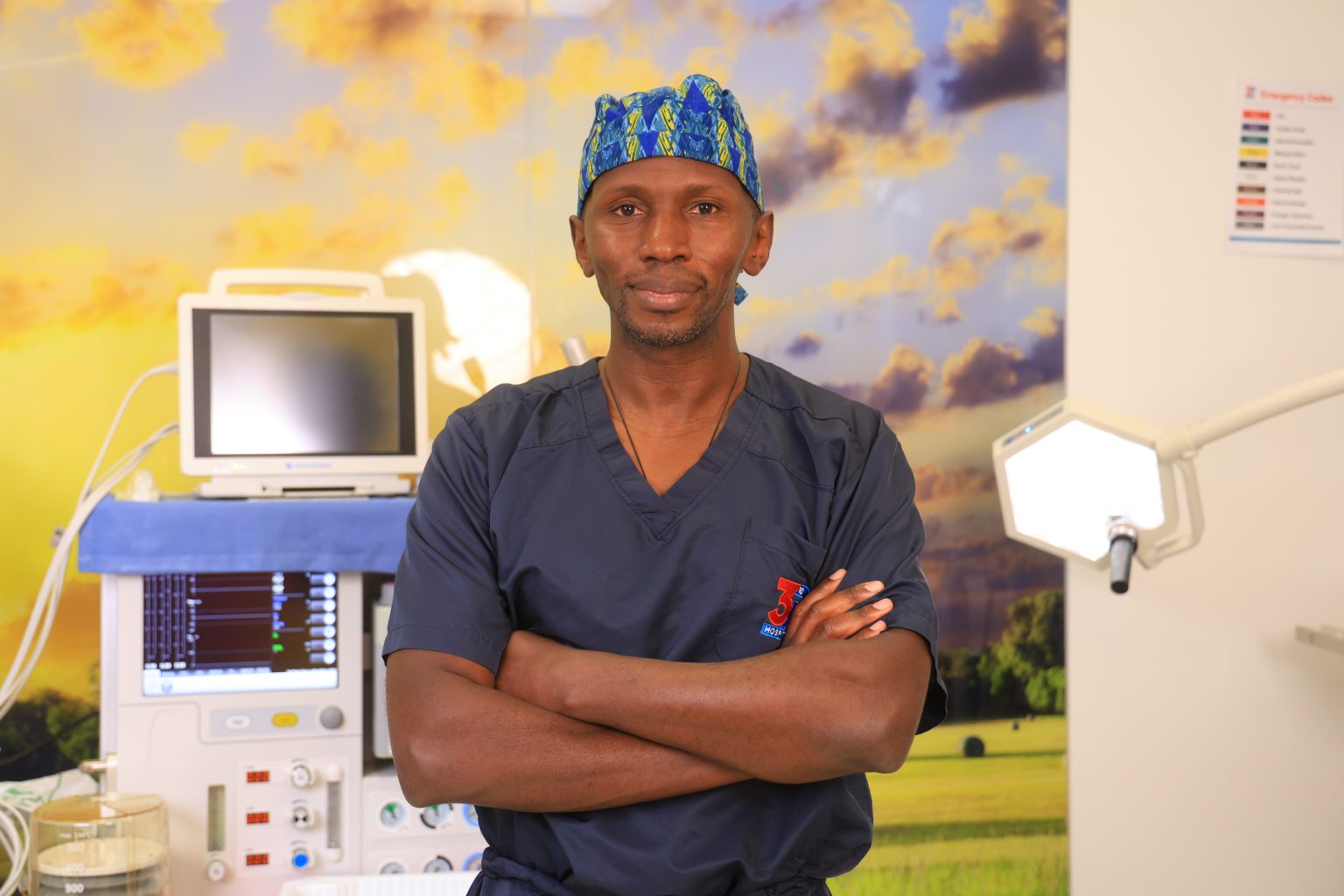
Three continents, two specialities, one decision. How a rugby injury, a surgeon father and years of quiet deliberation brought Dr Mordicai Atinga back to Kenya.
When Dr Mordicai Atinga speaks about surgery, his tone is measured, almost understated. There is no theatricality, no grand declarations, just the quiet confidence of someone who has spent years refining a precise craft across continents. But behind that calm delivery lies a decision that many highly trained professionals struggle with: whether to stay abroad or return home.
For Dr Atinga, a specialist in Sports Medicine, Shoulders and Knees, the answer was neither immediate nor simple. “It was a timing thing,” he says.
After years of training in the United Kingdom, Australia and New Zealand, he reached what he described as a transition point, a moment where the trajectory of his career could diverge permanently.
“You get to a stage where you’ve completed your fellowship training, and that qualification becomes a kind of passport,” Dr Atinga says. “It gives you options. You know you can work in different systems.”
For many, that passport leads to permanence abroad. For Dr Atinga, it opened the door to a question he could no longer ignore: why not return to Kenya?
At the centre of conversations to relocate to Kenya was his father, himself an orthopaedic surgeon
The decision to come home was not driven by a single moment of clarity. Instead, it unfolded over several years of reflection, planning and consultation. “It took maybe three or four years,” he says. “You don’t just uproot everything overnight. There were a lot of conversations with my family members and with mentors, and a lot of thinking about whether it would work for me or not.”
At the centre of those conversations was his father, himself an orthopaedic surgeon, whose influence on his son’s career is both acknowledged and, at times, gently contested. “If you had asked me 10 years ago, I would have said it was entirely my own choice,” Dr Atinga says. “But the more I think about it, there must have been some influence.”
That influence was not just professional but personal. Growing up around medicine meant early exposure to the realities of the field. But it was his own experiences as a young athlete that would shape his eventual path. “I broke my wrists three times playing rugby,” he recalls. “I had knee problems, muscle injuries. I would go through my dad’s books trying to understand what was wrong.”
Those early encounters with injury sparked a curiosity that would later define his career. Orthopaedics, he says, appealed because it was tangible. Problems could be identified, understood, and often fixed.
Dr Atinga’s journey through medical training was not without difficulty. An early setback came during his initial studies, where he found himself struggling to keep pace with his peers. “I joined late, about six weeks behind everyone else,” he says. “And in medicine, that’s significant. It felt like I was always catching up.”
From early on, he had decided on orthopaedics and every step was aligned with that goal
The experience, he says, was humbling. Surrounded by high-performing students, he began to question whether he truly belonged. “It felt like sprinting against elite sprinters,” he says. “You’re running as fast as you can, but everyone else is already ahead.”
That period, however, proved formative. By the time he moved into the UK training system, he had developed the resilience and discipline required to thrive. “The training there is very structured,” he explains. “You know what’s expected of you from the start. You just have to manage it.”
He remained focused throughout. From early on, he had decided on orthopaedics, and every step of his training was aligned with that goal. “If I had a project, it would be orthopaedic. If I had a rotation, I tried to make it relevant,” he says. “Everything pointed in that direction.”
Despite the breadth of Sports Medicine, Dr Atinga’s work is highly specialised. “Shoulders and knees,” he says. “That’s my focus.”
It is a choice shaped partly by timing. When he began his training, shoulder arthroscopy was still developing. The procedure uses a tiny camera and specialised instruments to diagnose and treat problems inside the shoulder joint with minimal invasion. “It was in its infancy,” he says. “That made it exciting. We were all learning, all figuring things out.”
Young athletes present with dislocations, older patients require treatment for degenerative conditions
The shoulder, Dr Atinga explains, remains one of the most complex joints in the body. Unlike the knee, where many procedures are well established, shoulder surgery continues to evolve. “We still don’t have all the answers,” he says. “There’s always new data, new approaches.”
The range of patients adds to the challenge. Young athletes present with instability and dislocations, while older patients often require treatment for degenerative conditions such as arthritis. “You’re dealing with completely different problems at different ends of the age spectrum,” he says.
In Australia, Dr Atinga worked in a system deeply embedded in sports culture. The cases were frequent and often complex, reflecting a population heavily engaged in physical activity. “It was high volume,” he says. “A lot of shoulder and knee injuries, particularly from contact sports.” The experience exposed him to an intensity that sharpened both his technical skills and his decision-making.
In New Zealand, the focus shifted slightly, with greater emphasis on joint replacement and long-term outcomes. “The two experiences complemented each other,” he says. “One was more acute, more sports-focused. The other looked more at longevity and function.”
Together, they provided a comprehensive foundation, one he hoped to bring back to Kenya.
Returning home, Dr Atinga expected to encounter significant limitations in equipment and resources. Instead, he found a system that, in many ways, matched what he had seen abroad. “We have the same implants, the same tools,” he says. “That was a pleasant surprise.”
Many patients seeking specialised treatment still believe care abroad is superior
The challenge, however, lies in cost and sustainability. “Everything is imported; by the time it gets here, it becomes expensive.” That cost has real consequences. Patients who might otherwise be treated locally often choose to travel abroad, sometimes finding it cheaper even after factoring in flights and accommodation. “It’s difficult to explain,” he says. “But it happens.”
Beyond cost, another factor driving medical tourism is trust. Many patients seeking specialised treatment still believe care abroad is superior. “There’s a perception that care abroad is better,” Dr Atinga says. “But that’s not always the case.”
He believes Kenya has a growing number of highly trained specialists capable of delivering world-class care. The problem, he says, is that their work is not always visible. “We tend to speak to ourselves,” he says. “We publish in journals, we present at conferences, but the public doesn’t always see that.”
Bridging that gap, he argues, is essential. “There needs to be a way of translating what we do into something the average person can understand.”
For a country known globally for its athletes, Kenya’s sports medicine infrastructure remains uneven. “It’s not about individuals,” Dr Atinga says. “We have good people, surgeons, physiotherapists, nutritionists. What we lack is structure.” In more developed systems, athletes are supported by integrated teams that manage everything from injury prevention to rehabilitation. “In Kenya, it’s often fragmented,” he says. “Some teams have good setups, but it’s not consistent.”
That inconsistency can have serious consequences, particularly for athletes whose careers depend on timely intervention. “A small injury, if not managed properly, can become career-limiting,” he says.
Orthopaedics is being reshaped by advances in technology, including robotic surgery
One of the most significant influences on Dr Atinga’s practice comes from his time in the UK, where healthcare systems operate under both financial constraints and legal scrutiny. “Resources are limited, so you have to be careful how you use them,” he says. At the same time, a culture of accountability means that communication and documentation are critical.
“Doctors have to be very clear with patients,” he says. “What you say, what you do, how you document it all matters. These habits are not just about avoiding legal issues. They are essential for building trust. Ultimately, patients are allowing you to operate on them. That is a huge responsibility.”
Like many areas of medicine, orthopaedics is being reshaped by advances in technology, including robotic surgery. “It’s coming,” Dr Atinga says. “Whether we like it or not.” While robotics can improve precision, particularly in procedures such as knee replacements, he remains cautious. “We still need to show that it improves outcomes, not just images.”
For now, he sees it as a tool, not a replacement. “You still need a surgeon,” he says. “The human element is still critical.”
For young doctors entering the profession, Dr Atinga’s advice is simple: be patient. “There’s a tendency to want to move quickly, to establish yourself, to make a name,” he says. “But medicine rewards those who take their time. Nothing is wasted.”
In surgery, that trust is profound. Patients place their lives in the hands of someone they may have only just met. “You have to live up to that,” he says.