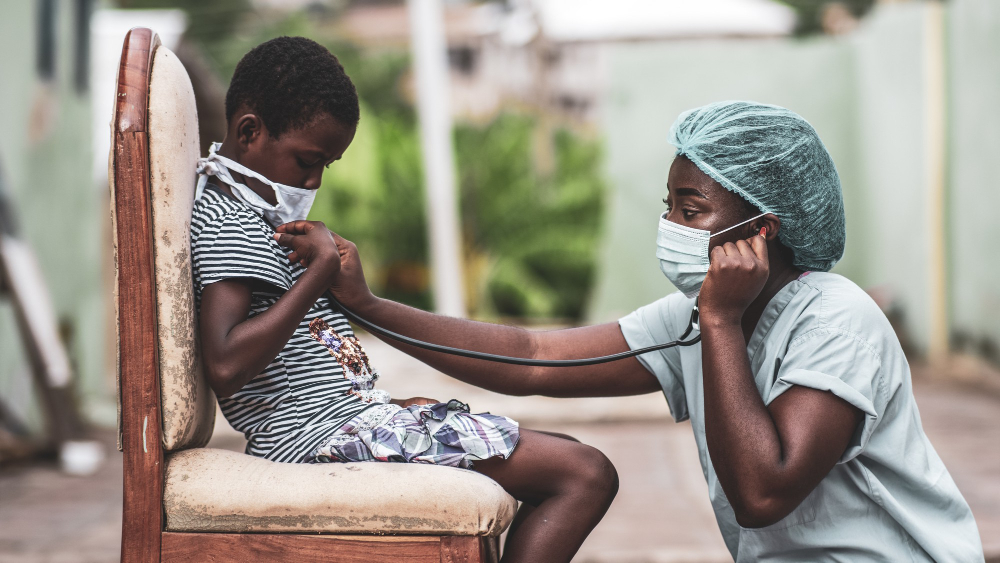
Tuberculosis is treatable, but in many Kenyan communities, diagnosis is linked with HIV, which has become an invisible barrier – which no pill can break, or lab test can find.
In Kenya’s fight against tuberculosis, the greatest challenge is not always the bacteria itself, but the belief systems that surround it. Nearly every Kenyan has heard of TB, yet deeply entrenched misconceptions, particularly the widespread belief that TB and HIV are the same condition, continue to block diagnosis, treatment and survival. The problem is worst in specific counties, sharpest among older women, and most stubbornly resistant in communities where education and health infrastructure remain thin.
According to the 2022 Kenya Demographic and Health Survey (KDHS), 96.8 per cent of women and 98.3 per cent of men aged 15 to 49 have heard of TB. But among those who have, 4.7 per cent of women and 4.4 per cent of men believe that everyone with TB also has HIV.
Kenya’s recorded TB cases account for only 68 per cent of all detected TB cases, meaning a large share of actual cases go undiagnosed. During the World TB Day 2026 commemorations, Health Cabinet Secretary Aden Duale revealed that Kenya diagnosed and treated 90,900 people in 2025. While this represents 81 per cent of the estimated TB burden, it leaves a dangerous 19 per cent missing. Kenya’s 2023 National TB Annual Report notes that only 38 per cent of the set target for TB Preventive Therapy contacts was reached.
Despite these technological and clinical strides, the shadow of stigma remains the most formidable barrier to a TB-free Kenya. In many Kenyan clinics, TB screening is linked to HIV testing, especially in maternal health settings. Without clear communication, women may leave believing the two conditions are inseparable, even though TB is an airborne bacterial infection and not a marker of HIV status.
TB stigma, myths and misconceptions highest in Nyamira, Narok and Meru counties
At the county level, Nyamira and Narok stand out as stigma hotspots, with misconception rates far above the national average. Nyamira records a male misconception rate approaching 19 per cent, while Narok shows the highest female misconception rate, both far outside the national distribution and flagged as statistical outliers. In Nyamira, nearly one in five men believes all people with TB have HIV.
Nyamira County is among the counties in Kenya with the highest HIV burden, with an estimated HIV prevalence of 3.5 per cent and a high TB-HIV coinfection rate of 25 per cent, which continues to point to missed opportunities to provide HIV and TB testing, treatment and care. The misconception rate in Nyamira is not evidence of ignorance in a vacuum. It is evidence of a community experiencing genuine TB-HIV co-infection at high rates, absorbing that reality as a general rule, and having insufficient health literacy infrastructure to parse the distinction between correlation and causation.
People living with HIV and TB also face challenges such as stigma and limited access to health education, leading to limited health-seeking behaviour, late diagnosis and poor treatment adherence.
As a predominantly pastoralist county with historically limited fixed health infrastructure, Narok faces low partner and male testing, difficulties in disclosure, stigma and discrimination, and few ART sites. The high misconception rate here is less about clinical messaging gone wrong and more about a population that has been structurally excluded from health education in any consistent form. The health system’s physical footprint in Narok is thin; misconceptions fill the vacuum. In pastoralist and rural communities where health infrastructure is thin, misinformation often fills the vacuum left by limited access to education and services.
Meru’s appearance in the top ten counties with the highest HIV misconceptions is perhaps the most policy-relevant outlier. Unlike Narok or Nyamira, Meru is not a marginalised pastoral county with structural access problems. It is a mid-sized agricultural county with a relatively developed health infrastructure. Its presence in this list, with female misconception rates around 13 per cent, warrants a focused qualitative inquiry that the DHS data alone cannot provide.
Keeping girls in school longer is one of the most effective ways to reduce TB stigma
The data also shows a sharp drop in misconceptions once people move from primary to secondary school, with the biggest decline seen after secondary education. That makes schooling a public health intervention. Keeping girls in school longer may be one of the most effective ways to reduce TB stigma in the next generation.
A population that has moved through secondary education and holds fewer misconceptions about TB-HIV links is more likely to present for screening, more likely to adhere to treatment, and less likely to stigmatise household members with TB.
The findings also point to older women as a neglected group. Women aged 40 to 49 have the widest awareness gap compared with men, yet they are often the primary caregivers in their homes. If caregivers are misinformed, the consequences reach beyond their own health, affecting how families respond to symptoms, isolate sick relatives and complete treatment.
Children remain heavily affected by TB, with an estimated 337,000 children aged 0 to 14 developing TB in the WHO African Region in 2024, reflecting ongoing gaps in prevention, early diagnosis and child-friendly treatment. Those children are largely in the care of mothers and grandmothers. If the women over 40 responsible for managing sick households are working from incomplete or distorted information about TB, the downstream effects on care-seeking, isolation practices and treatment adherence are direct and measurable.
What the data demands
Kenya’s TB communication strategy is currently built around general population awareness, mass media, World TB Day events and school drama performances. What the DHS demands is something more precise: women-centred messaging that explicitly separates TB from HIV, particularly in ANC settings; secondary school retention as a de facto health intervention; county-specific campaigns calibrated to local misconception profiles, with Nyamira, Narok, Mandera, Meru and Embu as the first tier of urgency; and dedicated outreach for women over 40 who are outside the health system’s current social media and maternity-channel reach.
Kenya’s Ministry of Health has already signalled the need for innovations in ensuring early detection and campaigns to help tackle misconceptions at the grassroots level.
“These innovations are enabling early and accurate detection, even in remote areas, as we take services closer to the people in line with Universal Health Coverage,” Health CS Aden Duale said.