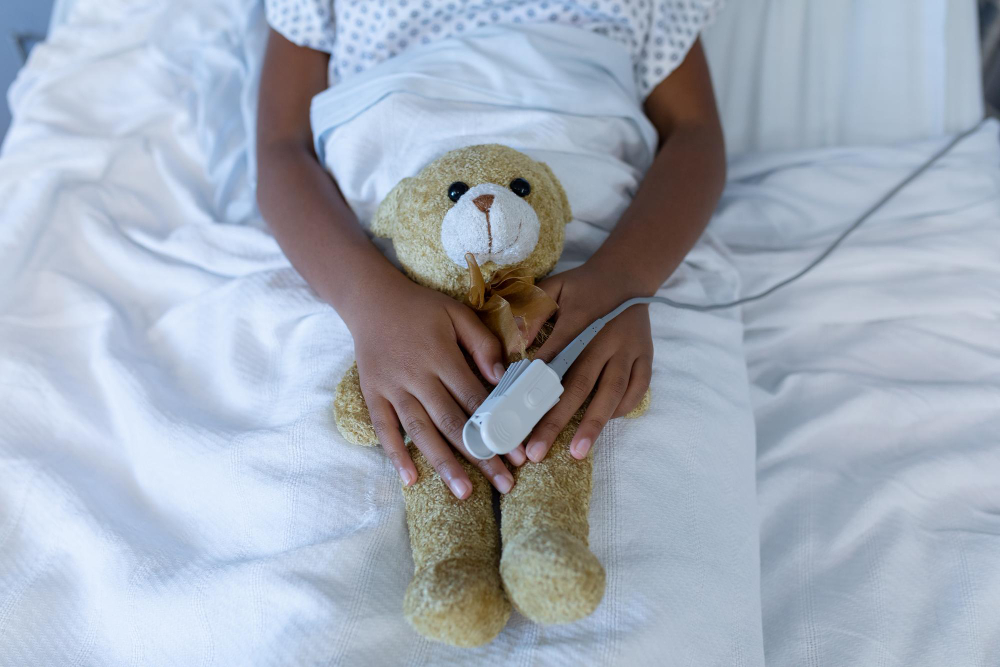
Newborns are the most vulnerable, with preterm birth, delivery complications, and infections driving the toll – exposing persistent gaps in maternal and newborn care across low- and middle-income countries.
Nearly five million children under five died in 2024, and decades of progress in child survival are at risk of being reversed, a United Nations report has warned. While child deaths have fallen by more than half since 2000, progress has stalled since 2015 at a rate of over 60 per cent.
The Levels & Trends in Child Mortality 2026 Report recorded 4.9 million under-five deaths, including 2.3 million newborns. For the first time, it includes comprehensive data on the underlying causes of death worldwide.
“Most of these deaths are preventable with low-cost, proven interventions and access to quality health care,” said UNICEF Executive Director Catherine Russell. “No child should die from diseases that we know how to prevent. But we see worrying signs that progress in child survival is slowing, and at a time when we’re seeing further global budget cuts.”
Dr Russell noted that history proves what commitment can achieve, and that continued investment and political will can build on past progress for future generations.
For Kenya, the global trends mirror familiar local challenges. While progress has been made, significant gaps remain in neonatal care, immunisation, and nutrition programmes. Malaria continues to threaten children under five, particularly in Western and Coastal counties, and access to quality maternal care remains uneven, especially in rural and conflict-affected areas.
Persistent challenges in Kenya are in data collection, newborn services, and treatment for severe acute malnutrition
The WHO notes that Kenya has implemented community-based health interventions, including training community health volunteers, expanding maternal and child health clinics, and distributing insecticide-treated nets. Persistent challenges, however, remain in data collection, essential newborn services, and treatment for severe acute malnutrition.
Among the most striking findings in the global data is the scale of death driven by malnutrition. Severe acute malnutrition directly claimed more than 100,000 children aged 1–59 months in 2024, five per cent of all deaths in this age group. When indirect effects such as heightened vulnerability to infections are factored in, the toll rises considerably higher.
Pakistan, Somalia, and Sudan are among the countries recording the largest numbers of direct deaths from SAM. Experts caution that the actual burden may be underestimated, as many deaths linked to malnutrition are misclassified in official data.
Newborns account for nearly half of all under-five deaths, making them the most vulnerable group. Complications from preterm birth account for 36 per cent of these deaths, while labour and delivery complications account for 21 per cent. Neonatal infections, including sepsis, and congenital anomalies also contribute heavily to the death toll. The data exposes persistent gaps in antenatal care, skilled delivery services, and newborn care across many low- and middle-income countries.
Beyond the first month of life, infectious diseases continue to claim young lives at an alarming rate. Malaria alone accounted for 17 per cent of deaths in this age group, with the vast majority of fatalities concentrated in sub-Saharan Africa. Countries such as Chad, the Democratic Republic of Congo, Niger, and Nigeria bear the heaviest burden, where conflict, climate shocks, drug-resistant parasites, and limited access to prevention and treatment continue to worsen an already dire situation.
Infectious disease-related deaths account for 9% of under-5 mortality in Europe and North America
Sub-Saharan Africa remains the epicentre of child mortality, accounting for 58 per cent of all under-five deaths globally in 2024. Infectious diseases alone cause more than half of these deaths, underscoring the urgent need for expanded access to vaccines, insecticide-treated nets, and primary health care.
The contrast with wealthier regions is stark. Infectious disease-related deaths account for just nine per cent of under-five mortality in Europe and North America, and only six per cent in Australia and New Zealand, a stark reflection of the deep inequities in health systems and resources that continue to divide the world.
Southern Asia, which accounts for 25 per cent of under-five deaths globally, faces a different pattern. The majority of deaths are linked to conditions around birth – preterm delivery, birth asphyxia, congenital anomalies, and neonatal infections – most of which are largely preventable with quality antenatal and perinatal care.
Fragile and conflict-affected settings remain especially dangerous. Children born in such environments are nearly three times more likely to die before their fifth birthday than their peers in more stable countries.
Dr Tedros Adhanom Ghebreyesus, WHO Director-General, issued a stark warning about the compounding effect of conflict on child survival. “Children living amid conflict and crisis are nearly three times more likely to die before their fifth birthday,” he said. “We must protect essential health and nutrition services and reach the most vulnerable families so every child has the chance not only to survive, but to thrive.”
Self-harm leading cause of death among girls aged 15 to 19, while road traffic injuries predominate among boys
The report extends its analysis beyond under-fives, estimating that 2.1 million individuals aged five to 24 died in 2024. Infectious diseases and injuries are leading causes of death among younger adolescents, while older age groups face markedly different risks. Self-harm is the leading cause of death among girls aged 15 to 19, while road traffic injuries predominate among boys of the same age. These patterns point to the urgent need for targeted interventions addressing mental health, injury prevention, and adolescent-friendly health services.
Under-Secretary-General for Economic and Social Affairs Li Junhua said the report serves as a stark reminder that progress on child survival is slowing and that too many countries are off track to meet the Sustainable Development Goals. He called for renewed political commitment, sustained investment in primary health care, and stronger data systems to ensure no child is left behind.
Li Liu, PhD, associate professor at the Johns Hopkins Bloomberg School of Public Health, reinforced the economic and moral case for acting now.
Reversing the slowdown in child survival requires urgent, coordinated action
“These estimates demonstrate that many deaths among children under five, from causes such as preterm birth, lower respiratory infections, and injuries, are avoidable with proven, cost-effective interventions,” she said. “The science is clear: targeted investments in primary health care, maternal and newborn health services, routine immunisation, nutrition programmes, and quality and timely data systems can save millions of lives.”
Monique Vledder, World Bank Group Director of Health, called for faster action at scale. “These findings are a collective call to speed up implementation of the proven, scalable solutions we know are within reach. Our target is to reach 1.5 billion people with quality primary health services,” she said.
The UN report is clear: reversing the slowdown in child survival requires urgent, coordinated action. Governments and donors must prioritise child survival, focus on the most vulnerable, and invest in primary health care – including community health workers, skilled birth attendants, and quality newborn care. Cuts to maternal and child health programmes risk undoing a generation of progress.