Cancer cases in Kenya are set to hit 95,000 by 2040. Radiotherapy can save lives, but myths, high costs and too few specialists mean thousands may never access it.
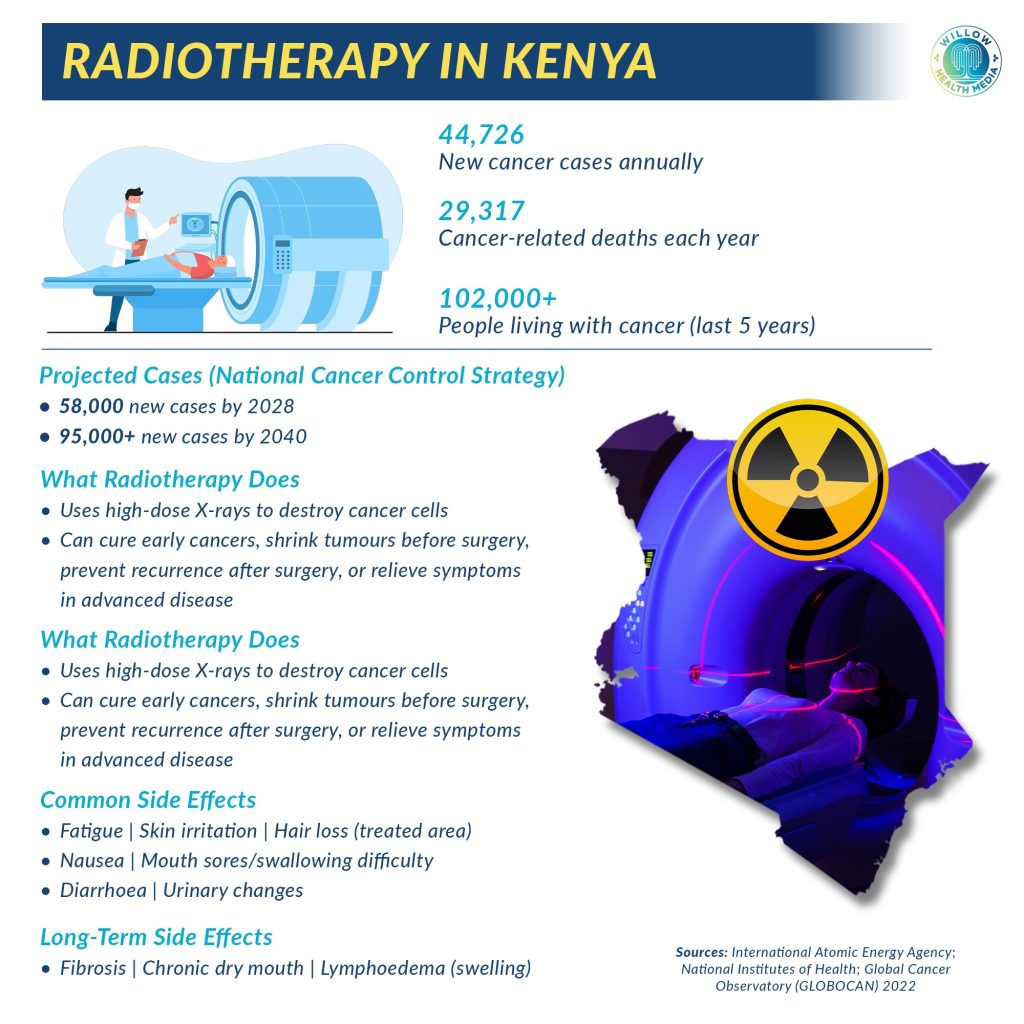
Kenya is facing a growing cancer burden that is placing increasing pressure on the health system and families. According to the Global Cancer Observatory (GLOBOCAN) 2022 estimates, the country records about 44,726 new cancer cases each year and around 29,317 cancer-related deaths annually. More than 102,000 people are currently living with cancer based on diagnoses made over the past five years.
These figures are expected to rise sharply in the coming decades. Driven by population growth, urbanisation, longer life expectancy and lifestyle-related risk factors, Kenya’s National Cancer Control Strategy (2023–2027) projects that the country will register about 58,000 new cancer cases by 2028, with the number climbing to over 95,000 by 2040.
As cancer cases grow, so does the need for effective treatment options. Modern cancer care is personalised, with doctors selecting therapy based on the type of cancer, its stage and its location in the body. Patients may receive surgery, chemotherapy, immunotherapy, targeted therapy or hormone therapy, often in combination. One of the most important treatment approaches in this mix is radiotherapy.
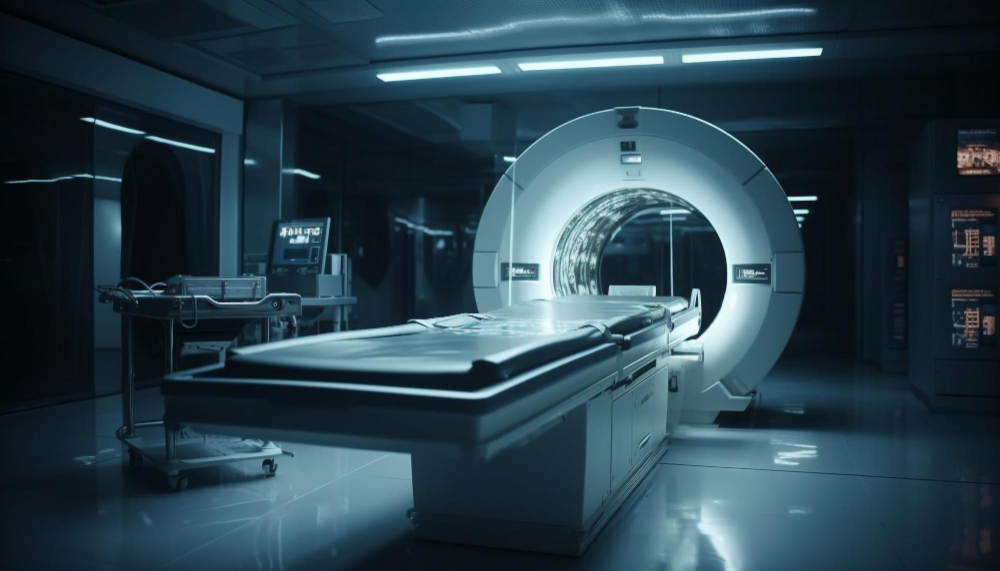
Radiotherapy uses high-energy radiation, most commonly X-rays, to destroy cancer cells by damaging their DNA and stopping them from multiplying. It is a localised treatment, meaning it targets a specific tumour rather than the whole body.
“Radiation is when we use high-dose X-ray treatment to destroy the DNA of cancer cells,” explains Dr Angela Waweru, a consultant radiation oncologist at Aga Khan University Hospital, Nairobi. “It is a local treatment, so it targets the tumour, delivers what we call ionising radiation and causes destruction of the cancer cells.”
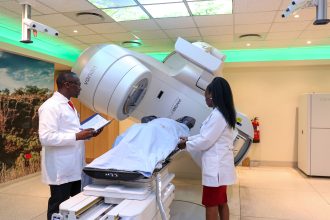
Radiotherapy for both children and adults is applied to most cancers diagnosed in Kenya
Radiotherapy can be used at different stages of cancer care. In early disease, it may be given with curative intent. It can also be used before surgery to shrink tumours and improve surgical outcomes, or after surgery to eliminate remaining cancer cells and reduce the risk of recurrence. For patients with advanced or stage four cancer, radiotherapy can help relieve symptoms such as pain, bleeding or obstruction that interferes with breathing or swallowing. “It is utilised across all stages of cancer,” Dr Waweru says.
Radiotherapy is used for both children and adults and is applied to many of the cancers most commonly diagnosed in Kenya.
“For women, we treat a lot of breast cancers, cervical cancers and endometrial cancers,” Dr Waweru notes. “For men, prostate cancer is our number one. Across genders, we see rectal cancer and oesophageal cancer. But in reality, we can treat all types of cancers, all stages and all ages.”
Despite its wide use, radiotherapy is still surrounded by fear and misconceptions. Many patients worry that it is painful or that they will become radioactive after treatment. In reality, the procedure itself is painless. During treatment, a patient lies on a hard table while the machine moves around them, delivering radiation precisely to the tumour. The process of positioning, quality checks and treatment delivery takes about 20 minutes on average.
“Many patients tell you their only awareness is the movement of the machine around them, knowing that it is delivering treatment,” Dr Waweru explains.
Small doses over time destroy the cancer cells while protecting healthy tissue
There is no standard number of radiotherapy sessions for all patients. The number depends on the type of cancer, its stage and the treatment goal, whether cure, control or symptom relief.

“We don’t have a standard number of sessions,” says Dr Waweru. “Radiotherapy is usually given over multiple days because small doses delivered over time gradually destroy the cancer cells while protecting healthy tissue.”
With advances in technology, treatment schedules are becoming shorter for some cancers. In certain palliative cases, such as relieving severe pain or bleeding, doctors may deliver a single high-dose treatment. For curative treatment or long-term disease control, however, smaller daily doses over several weeks remain common.
Like most cancer treatments, radiotherapy can cause side effects. Some appear during treatment and improve within weeks, while others may last longer. Common short-term side effects include fatigue, skin irritation, hair loss in the treated area, nausea, mouth sores, swallowing difficulties, diarrhoea and urinary changes. Long-term side effects can include fibrosis, chronic dry mouth and lymphoedema, which causes swelling of the arms or legs.
“The vast majority of side effects are temporary,” Dr Waweru says. “And they depend on the location we are treating. Side effects for lung cancer will be very different from those of prostate cancer.”
Once treatment is complete, patients do not pose any risk to family members
Modern radiotherapy technology has greatly improved safety by increasing precision and reducing damage to healthy tissues. According to Dr Waweru, 50 years ago, patients treated for left-sided breast cancer often suffered lung damage. Today, advanced machines can shield the heart and surrounding organs, making such complications far less common.
External beam radiotherapy is also not radioactive. Once treatment is complete, patients do not pose any risk to family members. The only exception is radioiodine therapy for thyroid cancer, which is radioactive and requires special inpatient isolation.
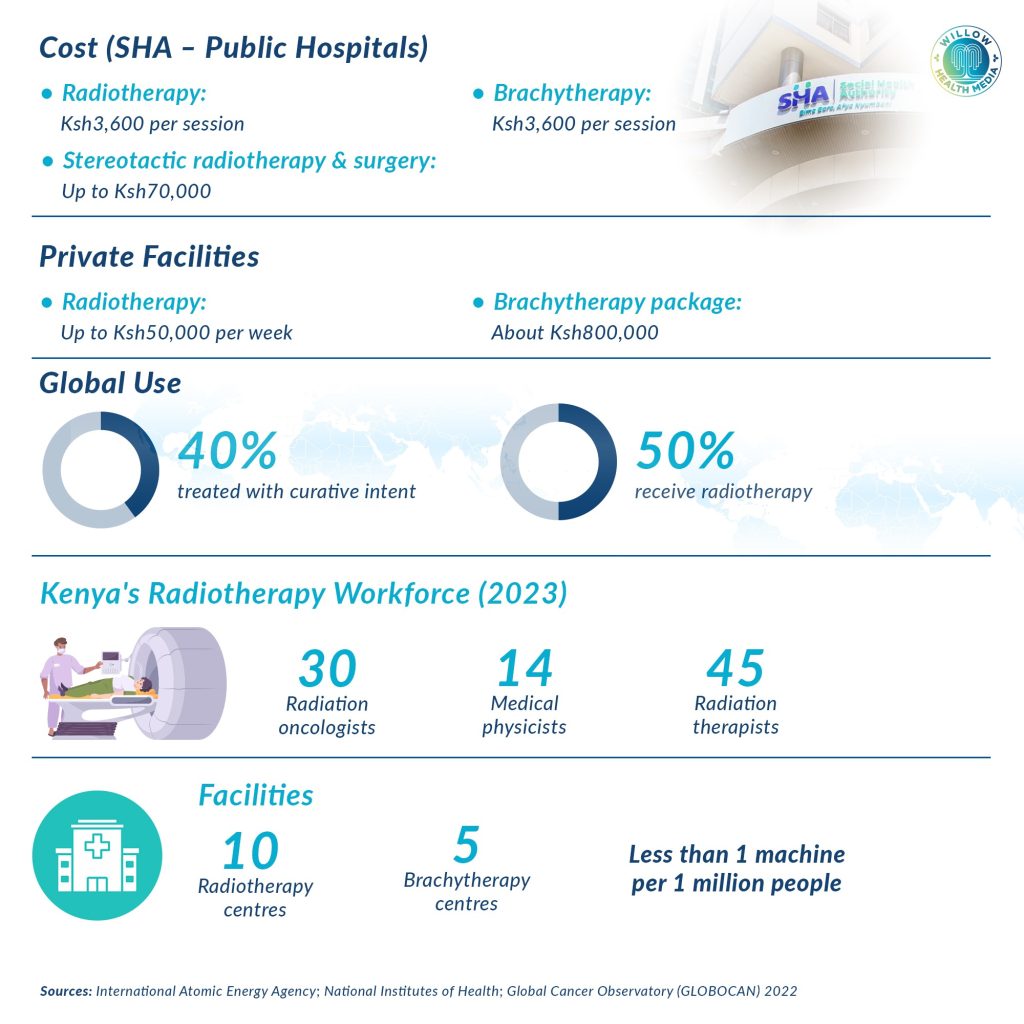
The cost of radiotherapy varies widely between public and private hospitals. Under Kenya’s Social Health Authority (SHA) oncology package, radiotherapy in public facilities is capped at Ksh3,600 per session, brachytherapy at Ksh40,000, and stereotactic radiotherapy and surgery are covered up to Ksh70,000. In private facilities, however, costs can be much higher. Radiotherapy may cost up to Ksh50,000 per week, while a full brachytherapy package can reach Ksh800,000.
Dr Waweru acknowledges that treatment in private hospitals is expensive but says the pricing reflects heavy investment in modern equipment such as high-specification radiotherapy machines.
Access to radiotherapy in Kenya has improved significantly over the past decade. Public and private hospitals have expanded services, and counties are increasingly installing radiotherapy machines, reducing the need for patients to travel to Nairobi.
“I’m glad the landscape of oncology in Kenya has grown in leaps and bounds,” Dr Waweru says. “Both the public and private sectors are investing heavily in radiotherapy, which gives increasing access.”
Kenya had 30 radiation oncologists, 14 medical physicists and 45 radiation therapists by 2023
Globally, radiotherapy is a cornerstone of cancer care. According to the National Institutes of Health, about 50 per cent of cancer patients receive radiotherapy as part of their treatment, with 40 per cent treated with curative intent. However, Kenya still faces serious shortages of skilled personnel. As of 2023, the country had only 30 radiation oncologists, 14 medical physicists and 45 radiation therapists. Data from the International Atomic Energy Agency show that Kenya has 10 radiotherapy centres and five brachytherapy centres, less than one machine per million people, far below international recommendations.
Many patients still present late due to fear, stigma or misinformation about cancer treatment. Dr Waweru encourages patients to seek information directly from specialists rather than rely on myths.
“We want them to come and hear from us, for your type and stage of cancer, this is the radiotherapy you will get, and these are the side effects you may experience,” she says. “Coming with an open mind usually allays a lot of fears and dispels old wives’ tales.”
As Kenya confronts a future with more cancer cases, expanding radiotherapy services, training more specialists and strengthening public education will be essential. Radiotherapy is not only a life-saving treatment for many patients, but it is also a critical pillar in building a comprehensive, equitable cancer care system for the country.