Wafula took his son to the hospital to escape the dangers of a traditional cut. Instead, the dangers followed him there…yet medical horrors from traditional circumcision starring unsterilised knives, excessive bleeding, sepsis and death, are fading away….
Wafula, a teacher and small-scale farmer in Bungoma, Western Kenya, took his son and nephew to be circumcised. This rite of passage has been observed by his Bukusu people every other year in August, followed by seclusion ceremonies in December to shape boys into men.
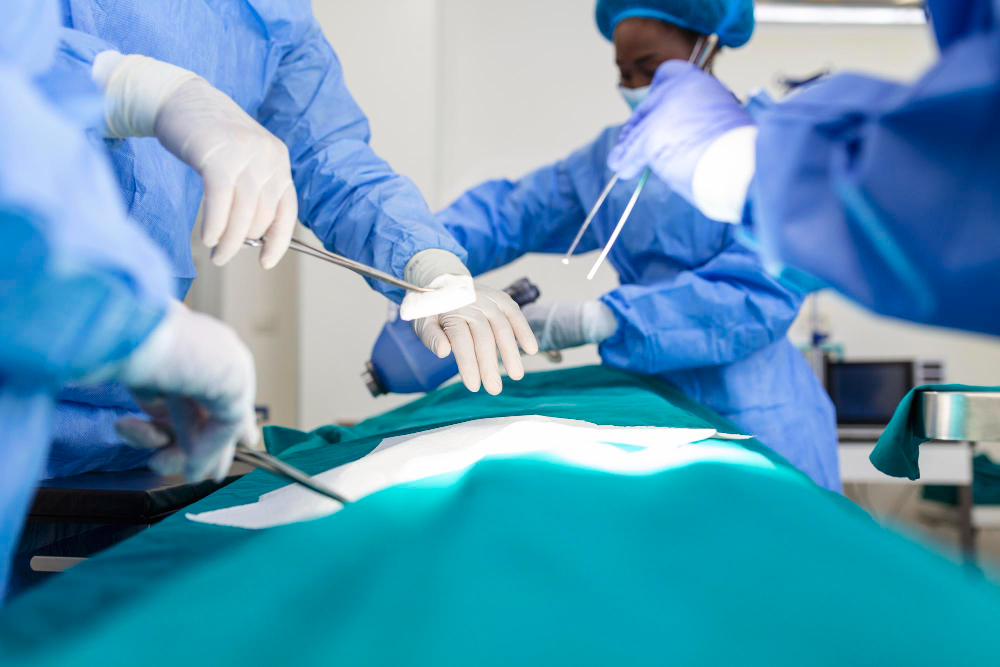
But instead of having his son initiated in the forest under a communal circumciser’s knife, Wafula opted for a safer, hospital alternative costing Ksh1,000 per boy in a public facility. In private hospitals, the cost ranges from Ksh10,000 to Ksh90,000.
Surgeons circumcised the boys who returned home to a Likombe, a special house for initiates, under the care of their grandfather and an uncle, a former nurse.
The nightmare began in the second week when the nephew healed, but not Wafula’s son, as “He walked with difficulty, he was in pain.” There was a darkened cut at the tip of my son’s organ.”
The son was rushed to the Bungoma West Hospital, where doctors noticed that “The circumcised area was dry and almost falling off,” Wafula recalls. “I was scared. I was angry. They told me the only option was corrective surgery, which was performed at the Kakamega Referral Hospital.
The medics suggested skin graft performed abroad as the only long-term solution
The medics discovered that tissue beneath the skin had dried and become gangrenous, rotting away. With corrective surgery and a month under medication, the son did not heal. No new skin grew naturally.
The medics suggested a skin graft performed abroad as the only long-term solution. “I ran up and down looking for money,” recalled Wafula, who considered taking his son to the USA, where his brother lives, or India.
Wafula was lucky, though. Some friends connected him to two Indian doctors on an exchange programme at the Kenyatta National Hospital (KNH) in Nairobi, where “The surgeon harvested skin from his thigh and grafted it onto the affected area, giving the organ a new layer of skin.”
Skin graft surgery at KNH costs Ksh1.2 million. Admission at Bungoma West Hospital for two months at Ksh3,000 daily cost Ksh180,000. Other medical expenses, including getting a passport, travel, food and accommodation, came to about Ksh1.6 million.
His son healed after a month but is still “traumatised psychologically as his friends had already gone through the forest seclusion and became men.”
The circumcision ordeal at a modern hospital contrasts with the dangers of the past
Wafula was stressed to get everything right and have the right of passage completed in 2022, an even year when “I feared I might not have a genealogy from this young man, but now I am confident I will one day have grandchildren.”
Wafula’s son told Willow Health Media that “From January to May 2023, I didn’t attend school. I stayed at home. Raising money for the surgery was difficult, but we managed despite the trauma I was subjected to.”
His mother, Bridget, terms it “The most difficult time of my life…we had no money, no time, and I was trying to care for the rest of my children while praying my son would survive the ordeal.”
The circumcision ordeal at a modern hospital stands in sharp contrast to the dangers of the past. Traditionally, untrained circumcisers using unsterilised knives caused excessive bleeding, amputation, penile damage, uneven cuts, urinary complications, sepsis and gangrene. Boys died in silence. Their deaths were blamed on fate, not preventable medical errors.
The shared blade was the greatest danger. A single knife moved from boy to boy, sometimes circumcising an entire village without sterilisation. When HIV/AIDS swept East Africa in the 1980s and 1990s, this practice became a transmission route.

Multiple boys were circumcised with shared, unsterilised blades
A 2016 study in PLOS Medicine found that traditional circumcision practices increased HIV transmission when hygiene was poor, especially when multiple boys were circumcised with shared, unsterilised blades.
Dr Nicholas Kitungulu, County Executive Committee Member for Health Services in Vihiga County, is clear about the health risks posed by traditional circumcision. “In the forest, there is very little we can control,” he says. “It is heavily protected by tradition, and even those taking care of the boys may be HIV positive, yet they are not screened.”

He notes that while some Luhya communities, including the Terik in Hamisi and Tiriki, still practise traditional circumcision, public awareness campaigns have reduced the numbers significantly.
“Recent reports show that HIV infections among the youth are highest in Hamisi, where traditional circumcision continues,” Kitungulu says. “Sometimes the knives may not be properly sterilised, and blood exposure can lead to infections. The hands of those performing the cut are often the hidden risk.”
The World Health Organisation (WHO) estimates that complications from unsafe traditional male circumcision affect 10-20 per cent of procedures performed without medical oversight, with serious adverse events including haemorrhage, sepsis, and permanent disfigurement occurring in two to three per cent of cases.
Traditional circumcisers have embraced training, hygiene, and medical knowledge
Over the past two decades, Western Kenya has seen a quiet revolution. Traditional circumcisers have embraced training, hygiene, and medical knowledge- transforming their ancient practice while preserving their cultural soul.

Philip Wanyonyi Wekesa, the Minister of the Bamaasaba Cultural Institution in Kenya and Uganda, says nowadays transmission of diseases like HIV has reduced as “We ensure that those performing circumcision are trained in hygiene and medical knowledge.”
Joseph Sinino Omukolongolo, the chairman of traditional circumcisers in Bungoma County, explains that previously, cold river waters at dawn helped to reduce pain, while smearing the initiates with soil was for preventing infections. The circumcision knife, the lukembe, on the other hand, is passed through fire to kill germs after cutting the foreskin in seconds.
“Healing is quick, usually within one or two weeks,” he said. It costs between Ksh300 and Ksh500 to circumcise a Bukusu boy.
Omukolongolo adds that “If an accident happens, we immediately make a hospital referral, but rarely do accidents occur.”
A traditional circumciser cannot have sex, drink alcohol, or leave his homestead
Wekesa acknowledges that maintaining standards requires discipline.
“A traditional circumciser cannot have sexual intercourse with women, drink alcohol, or leave his homestead during the month-long circumcision period. These rules were designed to protect him from making mistakes.”
He adds, “In the past, no payments were made; sometimes a chicken or local brew was enough. Today, people rush the process for money, and some cultural practices are ignored. Circumcision must continue, but it should be respected and performed safely, blending tradition with modern knowledge.”
This training revolution has yielded measurable results.
A 2018 study by the Kenya Medical Research Institute (KEMRI) found that trained traditional circumcisers who adopted sterile techniques and single-use instruments reported complication rates comparable to medical circumcision when performed under proper conditions, with adverse events dropping from historical rates of 15-20 per cent to below five per cent.

Modern hospital circumcision protects boys from HIV, hepatitis
Dr Kitungulu advocates strongly for hospital-based circumcision while acknowledging the cultural significance of traditional rites. “Modern hospital circumcision protects young people from transmissible infections like HIV, hepatitis, and other viral and bacterial diseases,” he explains. “Clinicians and surgeons are trained, procedures are standardised, and any complications are immediately managed. In the forest, a boy who bleeds excessively may never reach a hospital in time.”
However, Kitungulu acknowledges the cultural importance of traditional rites. “We are not calling for the end of culture,” he says. “Take your boys to the hospital for the operation, but continue with the traditional celebrations in the forest. Anyone responsible for their care should be tested for HIV and hepatitis to ensure the boys’ safety.”
He emphasises a balance between modern medicine and cultural practice. “It is difficult to control beliefs, but with education and advocacy, people are beginning to embrace hospital circumcision while preserving their heritage.”
The tension between these perspectives reveals a deeper truth: neither system is without risk. Today, tradition moves to a different rhythm. It shares the road with hospital corridors, surgical gloves and signed consent forms. Parents stand between ancestral obligation and medical counsel. Elders defend rituals that forged communities, while doctors tally injuries, infections and even deaths that never find their way into a song.