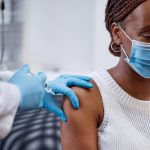
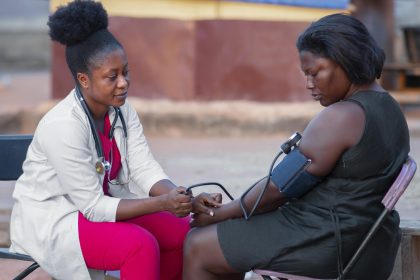From file-opening fees to mystery charges, the confusion around what SHA covers is costing Kenyans money they were never supposed to spend.
The government has defended the Social Health Authority’s (SHA) healthcare financing model, saying it was designed to protect poor Kenyans, not burden them. However, two persistent problems remain: hospitals illegally charging patients for services that should be free, and Kenyans who can afford to contribute but choose not to.
SHA Chair Dr Abdi Mohamed and University of Nairobi economics professor and Presidential Advisor on Health Financing, Dr Daniel Mwai, made the defence during the Willow Health Media Lifeline Dialogues, where they dismissed critics of the system and urged all Kenyans to participate.
The dialogue came after a story published by African Uncensored investigated whether the proxy means-testing model used by SHA was overestimating the incomes of poor Kenyans and forcing them to overpay. Dr Mwai dismissed the claims, arguing that critics were focusing on an early version of the model rather than the improved final system.
He said the government deliberately designed the model to underestimate incomes rather than overestimate them, specifically to avoid placing heavy financial pressure on vulnerable households. “From the information that we have shared, the actual data vis-à-vis what was alluded to, you have seen close to 90 per cent plus are paying way below the Ksh600 mark,” he said.
The model was developed using data from between 16,000 and 30,000 households. It was later improved through a process known as ground-truthing, where researchers physically visited more than 2,000 households across eight counties, including Nairobi, to compare estimated incomes against actual living conditions. “There were steps that were taken to correct that issue. First, by doing two-step modelling. Secondly, by going back to the ground-truthing for eight counties. Nairobi, being one of them,” Dr Mwai said.
The old NHIF flat rate low-income earners paid more thus punishing poorer people
He reiterated that fixed contributions, such as the old National Health Insurance Fund (NHIF) flat rate, unfairly punished low-income earners because poorer people ended up paying a higher proportion of their income than wealthier Kenyans. “Anytime you fix a value, you disadvantage the poor people,” he said.
Under the current system, informal workers can contribute flexibly through the lipa pole pole (instalment) arrangement, which allows payments on a daily, weekly or monthly basis. “At Ksh600, that’s Ksh20 daily,” Dr Mwai said.

Both officials also pushed back against concerns that only five million contributors are carrying the financial burden, with Dr Abdi clarifying that many Kenyans misunderstand the difference between registration and contribution and treat them as the same thing, yet “They are mutually exclusive things completely.”
He explained that more than 30 million registered Kenyans are already entitled to free primary healthcare funded through taxation, whether or not they contribute to the Social Health Insurance Fund (SHIF) for services including outpatient treatment, laboratory tests, consultations, radiology services and emergency healthcare.
Dr Abdi also noted that many registered members have not yet updated their dependents, including spouses and children, on the system. SHA allows unlimited children and multiple spouses under one principal contributor.
Some public hospitals have been illegally charging patients small amounts to open files
One of the more direct admissions from the session was Dr Abdi’s acknowledgement that some public hospitals have been illegally charging patients small amounts to open files or access primary healthcare services that should be free under SHA.
He was unequivocal in response. “There’s nothing called opening files,” he said. He described such facilities as rogue providers and called on the public to report them to SHA county offices, saying the authority would act swiftly against them.
He said the biggest challenge SHA faces is not poor Kenyans who cannot pay, but public misunderstanding about what services are free and which facilities are permitted to charge. “We are actually suffering because of being open and transparent, something most people are not used to,” he said.
Both officials said SHA’s digital infrastructure was central to improving accountability and reducing fraud. Through the Afya Yangu app and USSD platforms, members can check their registration status, confirm whether employers have remitted their contributions, track dependents under their cover and monitor services billed under their names.
Dr Mwai argued that these digital systems were already helping SHA detect fraudulent hospital billing that had previously gone unnoticed under NHIF. He said some facilities had submitted suspicious claims, including duplicate billing and treatment records that did not match patient information. “Now we have an AI-driven system. When you identify this claim, it rejects,” he said. He added that claims rejection rates at some hospitals had already dropped significantly after providers realised the system was flagging suspicious activity.
SHA compliance maybe linked to business licence renewals, motor vehicle insurance verification
Dr Mwai said the most pressing enforcement challenge was not poor Kenyans who genuinely cannot afford to contribute, but those with stable incomes who choose to avoid payments. For salaried workers, contributions are automatic because employers deduct them directly from payroll. Informal workers with steady incomes, however, often escape the system entirely.
He suggested the government may eventually link SHA compliance to services such as business licence renewals or motor vehicle insurance verification, once ongoing court cases on mandatory enforcement are resolved. “If I’m coming to renew my business licence, can they also check that I’m paying SHA?” he asked.
Dr Mwai also defended the inclusion of elderly parents and retirees under SHA, arguing that older people are among the highest-risk groups for expensive conditions such as cancer, diabetes, kidney disease and heart conditions. He noted that many families willingly support elderly parents with food, housing and transport, but resist paying health premiums that could shield them from hospital bills running into hundreds of thousands of shillings.
He argued that SHA still offers broader access for elderly Kenyans than private insurers, many of whom exclude older clients because of age or pre-existing illnesses. “One minute you are this, the second minute you are in ICU requiring life support,” he said.
Both officials acknowledged that SHA still faces serious operational challenges but maintained that the reforms represent a meaningful shift toward universal healthcare coverage in Kenya. They called on the public to engage through public participation and media education, and framed the success of the system as a collective responsibility. “The only way it can work is if we work as a team,” Dr Abdi said.