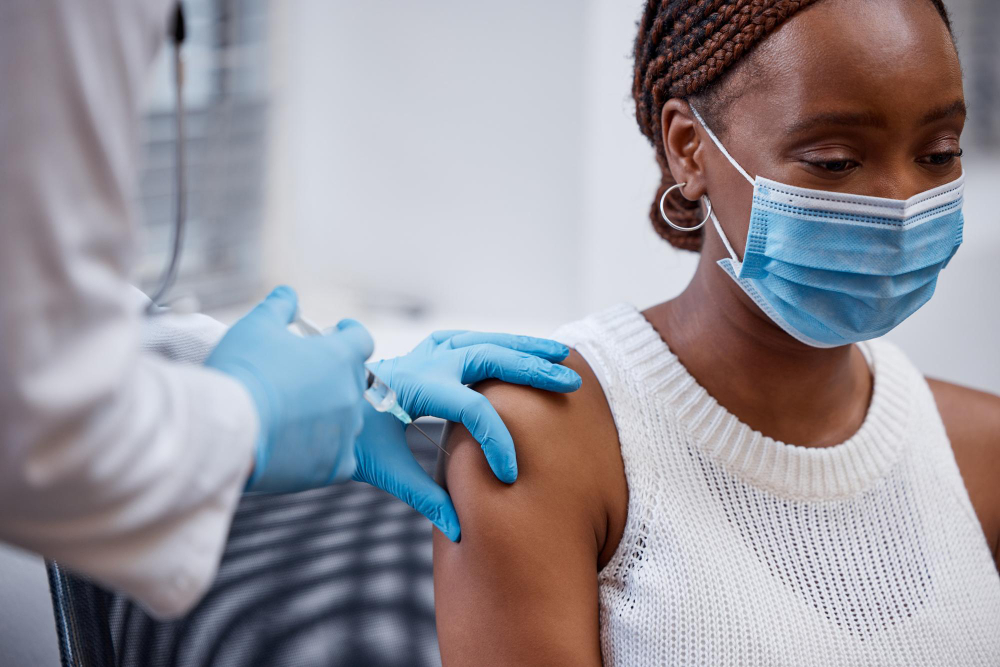
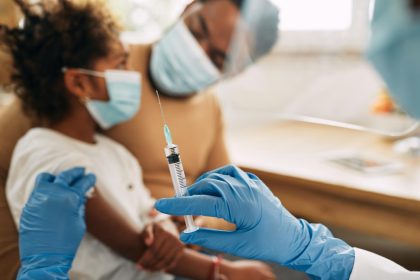
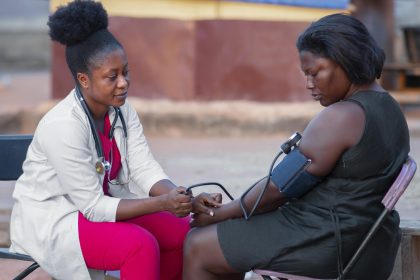Building vaccine factories on the continent is only half the challenge. The other half is convincing governments and populations to trust what comes out of them.
When COVID-19 vaccines rolled out as the pandemic ravaged the world six years ago, African nations found themselves last in line, watching from a distance as decisions made in faraway capitals determined who lived and who died.
That bitter lesson has now ignited a new resolve across the continent: to break free from the waiting game, produce vaccines at home, and take ownership of its own survival when the next global health crisis strikes.
This urgency drove a high-level discussion at the World Health Summit Regional Meeting 2026 in Nairobi, where policymakers, scientists, financiers and manufacturers converged to chart a path from political promises to functioning vaccine markets. Africa currently produces only about one per cent of the vaccines it uses, far below the African Union’s target of 60 per cent by 2040. Bridging that gap will require concrete action on financing, regulation and market creation and, as speakers made clear, far less talk and far more delivery.
Kenya is positioning itself at the forefront of this transformation. Principal Secretary for Medical Services Dr Ouma Oluga outlined a vision that extends beyond national borders. Kenya’s strategy is not simply to manufacture vaccines for its own population, but to anchor a regional system supplying a wider African market.
“The market is beyond Kenya to the region,” Dr Oluga said, noting that ongoing discussions with the Centre for Disease Control and Prevention (Africa CDC) are aimed at unlocking access to up to 21 countries through regional blocs such as COMESA and frameworks like the African Continental Free Trade Area.
Kenya is investing in regulatory systems, has set a target of producing its first vaccines by June 2027
Kenya has already committed to advance purchase agreements that guarantee demand for locally produced vaccines, a move seen as critical to attracting investment. “Commitment alone is not enough. Action speaks louder than words,” Dr Oluga stressed.
The country is simultaneously working on workforce development and infrastructure, working with partners such as the World Bank and the World Health Organization (WHO) to de-risk early investments. Kenya has set a target of producing its first vaccines by June 2027, acknowledging that timelines may shift while remaining resolute about the broader goal.
Execution, not ambition, is the central challenge. “The challenge is not ambition because it is there, but execution,” said Dr Frederik Kristensen of the Regionalised Vaccine Manufacturing Collaborative. Investors and manufacturers, he noted, consistently ask for three things: demand certainty, financing mechanisms that absorb early risk, and regulatory systems that enable products to move across borders. Without all three, political will remains exactly that.
At the centre of Kenya’s manufacturing ambitions is the Kenya BioVax Institute. Prof Richard Oduor described a phased approach beginning with fill and finish processes while building long-term research and development capacity. “We need to manufacture, we need to commercialise and translate research into healthcare products,” he said. He cautioned, however, that building factories alone will not guarantee success. Skilled personnel, regulatory systems and public trust are equally critical.
One of the most underappreciated challenges, Prof Oduor noted, is whether African populations will accept locally produced vaccines. “We are dealing with a population in Africa that is very cautious, particularly about products that are developed locally, hence the need for strong community engagement and trust-building efforts,” he said.
Vaccine manufacturing is capital-intensive, complex and slow to generate returns
The technical work of manufacturing, in other words, cannot outpace the social work of building confidence in what comes off the production line.
Financing remains a significant hurdle. Vaccine manufacturing is capital-intensive, complex and slow to generate returns, making it a difficult proposition for private investors.
Dr Peter Okwero of the World Bank Group highlighted the unique nature of vaccines as public goods, which complicates efforts to attract private capital. “The initial investment costs are very high, and it takes a long time to get your returns back,” he said. The World Bank is supporting countries like Kenya with concessional financing, infrastructure funding and risk guarantees designed to draw in larger investors. “The idea is really to de-risk major investments so that we can attract big capital,” Dr Okwero explained.
Beyond financing lies the equally critical question of market creation.
Dr Tala Jallow of the Africa CDC argued that Africa must actively shape its vaccine market rather than passively rely on global supply chains. “We have to make a choice, are we going to buy African-made products?” she said, urging governments to prioritise local manufacturers even if costs are initially higher. For Jallow, health security and supply security are inseparable. “We cannot talk about health security without supply security. Early investment is essential to achieving long-term affordability,” she said, drawing on lessons from the Covid-19 pandemic and pointing to the dramatic fall in antiretroviral drug prices as production scaled up over time as proof that the model works.
Regulatory progress has been made. Initiatives such as the African Medicines Regulatory Harmonisation programme and the African Medicines Agency have strengthened collaboration among countries. Gaps remain, however. A recent continental pilot showed that only one out of ten African manufacturers assessed met the required standards for approval. That figure points to a structural problem: manufacturing capacity and regulatory capacity must be built together, not sequentially.
A continent capable of producing own vaccines would respond more effectively to health emergencies
Farah Losper of the Africa Vaccine Manufacturing Initiative noted that promoting local manufacturing must go hand in hand with maintaining global quality standards. She pointed to ongoing discussions between African manufacturers and UNICEF for vaccine tenders as a meaningful milestone, reflecting how far the continent has come in a relatively short time.
The warning she attached to that progress, however, was unambiguous. “If you don’t get volumes at scale, you can never compete,” she said. Securing large and consistent markets for African manufacturers is not optional. It is the condition on which everything else depends.
The implications of getting this right are considerable. A continent capable of producing its own vaccines would respond more effectively to health emergencies, reduce preventable deaths, strengthen economies and foster innovation in science and technology. It would represent a shift from dependency to self-reliance, from vulnerability to resilience. Failure to act decisively could leave Africa trapped in the same cycle of dependence that defined its Covid-19 response. The stakes, as the Nairobi discussions made clear, are not merely technical or economic. They are existential.
The tools for transformation already exist. Financing instruments are available. Regional frameworks are in place. Scientific capacity is growing. What remains is the collective will to invest, to collaborate and to trust in African-made solutions, so that when the next crisis arrives, Africa is not once again left waiting at the back of the queue.