As global funding shrinks and testing gaps persist, WHO’s latest guidelines are pushing Kenya towards faster, more accessible tuberculosis testing
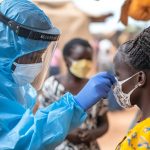
Kenya has been urged to accelerate its adoption of cutting-edge tuberculosis diagnostic tools, even as the World Health Organization (WHO) issued new guidelines calling for portable near-point-of-care tests, tongue-swab sampling, and pooled testing strategies to close stubborn detection gaps that continue to fuel the spread of one of the world’s deadliest diseases.
On World TB Day in March 2026, the WHO unveiled guidelines designed to deliver faster, more affordable, and accessible TB diagnostics, with WHO Director-General Dr Tedros Ghebreyesus declaring that the new tools “could be truly transformative for tuberculosis by bringing fast, accurate diagnosis closer to people, saving lives, curbing transmission and reducing costs.”
For Kenya, which is still ranked among the top 20 high-burden countries globally, the recommendations are not abstract. They arrive at a critical moment when domestic funding is under pressure; donor support is declining, and an estimated 30 per cent of TB cases in the country still go undetected.
Globally, TB claims more than 3,300 lives every day, with over 29,000 new infections reported daily. Despite decades of intervention that have saved more than 83 million lives since 2,000, WHO warns that funding shortfalls and diagnostic gaps now threaten to reverse that progress.
In Kenya, the numbers tell a sobering story. During World TB Day celebrations hosted by the University of Nairobi, Health Cabinet Secretary Aden Duale reported that approximately 90,900 people were diagnosed and started on treatment in 2025, representing just 81 per cent of the estimated national burden.
“This gap represents lives missed, families affected, and ongoing transmission within our communities,” Duale said.
The new guidelines highlight molecular tests, tongue-swab sampling, and pooled-sample strategies
Kenya has made measurable strides. Between 2015 and 2024, the country recorded a 48 per cent decline in TB incidence and a 58 per cent reduction in TB-related deaths; progress driven in part by expanded diagnostic infrastructure and community-level screening. But with nearly one in three cases still going undetected, health officials say the work is far from done.
At the centre of WHO’s 2026 guidance is a push to decentralise diagnosis, moving testing away from central laboratories and closer to communities, particularly those in remote or under-resourced areas.
The new guidelines highlight molecular tests, tongue-swab sampling as an alternative to sputum collection, and pooled-sample strategies that reduce costs and waiting times. These tools are especially significant for patients who cannot produce sputum, which is a common barrier in current testing, and for populations living far from health facilities.
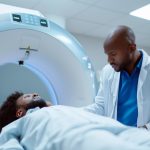
Kenya has already been moving in this direction. Duale told the gathering that, working with county governments and partners, the Ministry of Health has “scaled up TB services across all our 47 counties” and “strengthened diagnostic capacity by deploying the molecular test and the ultra-portable, AI-enabled digital X-ray machines.”
The country is among the first in Africa to deploy AI-powered portable digital X-ray machines for TB screening, taking the technology into some of the country’s most marginalised communities. The approach directly mirrors what WHO is now recommending: an integrated diagnostic network combining advanced technology with community-level access.
Men still account for 63 per cent of reported TB cases in Kenya, higher than women
While the tools are changing, the human dimensions of Kenya’s TB crisis remain complex. Men account for 63 per cent of reported TB cases in Kenya, a disparity that health officials attribute to entrenched attitudes around health-seeking behaviour.
“Men are more affected,” said Dr Nyikal Wambura James, a medical doctor and Member of Parliament for Seme Constituency. “I know men are stoic. They’ll cough for even longer than two weeks, and they are told to go to the hospital. And then they get sick.”
Duale called for “gender-responsive approaches” to reach men where they are through workplace TB programs, football events, entertainment venues, and community gatherings. “We aim to deliver services to men through sporting and social events, providing routine screening, health education, and care linkage,” he said.
Young people represent an equally urgent priority. In 2022, individuals aged 25 to 44 accounted for 63 per cent of all newly diagnosed TB cases in Kenya. Health Principal Secretary Mary Muthoni described this cohort as “the faces of TB in Kenya, but also the faces of courage, survival, and hope.”
To reach this demographic, Duale pointed to the hosting of the World TB Day event at the University of Nairobi as a deliberate strategy. “Over 300 young people have already undergone screening,” he said, adding that entertainment venues and football events should anchor future outreach efforts.
Dr Nyikal reinforced the urgency: “TB in this population is not only a public health concern but also a socioeconomic challenge.” Community Health Promoters, youth champions, and local leaders, he added, are proving that communities drive change; they do not simply receive it.
WHO has long emphasised the deadly overlap between TB and HIV, urging countries to deploy point-of-care urine tests and low-complexity diagnostics for people living with HIV as a key strategy for finding missing cases.
Donor funds are rapidly shrinking, leaving critical TB programs at risk
Kenya’s integration record is strong. PS Muthoni reported that HIV testing among TB patients reached 99 per cent, and of those found positive, 96 per cent were started on antiretroviral therapy. She described this as “compassionate, integrated, people-centred care”, an approach that links community-level screening with seamless TB-HIV services.
Muthoni also issued a direct public health appeal: “If you have a cough that is not going away, fever, night sweats, or weight loss, please go for testing early, because TB is preventable and curable.”
Perhaps the most pressing concern hanging over Kenya’s TB response is money. Dr Nyikal was candid about the risk, noting that Kenya’s TB program has historically relied heavily on external donor funding, support that is now shrinking.
“We must progressively increase domestic financing and ensure the Social Health Insurance Fund fully integrates TB services into the national financing framework,” he said. “As donor funds decline, we must use our available funds, whether from insurance or other sources, to support these programs.”
Duale echoed the alarm, disclosing that he had written to the National Treasury to protect funding for vaccinations, TB, and malaria from supplementary budget cuts, and confirming that the finance minister had approved the request.
The funding pressure is not unique to Kenya. WHO has warned that reductions in global health financing threaten to undermine hard-won TB progress in high-burden countries worldwide, particularly where advanced diagnostics remain expensive or limited to central facilities.
Despite the challenges, Kenya’s World TB Day messaging struck a tone of determined optimism. Duale was emphatic that the remaining detection gap is closable, and that doing so requires mobilising every sector of society.
“TB is curable, and services are available across the country,” he said. “No one should delay seeking care due to fears of discrimination.” He named faith leaders, civil society organisations, community health promoters, and TB survivors as essential to “finding missing cases, reducing stigma, and supporting treatment adherence.”
PS Muthoni called on Kenyans to “reject stigma, choose compassion, act with urgency, and stand together as one nation,” while Dr Neema Kimambo, the WHO Representative to Kenya, underscored that “empowered communities are important to ensure that no one is left behind.”
For Duale, the mission is clear: “Ending TB is a government-led, coordinated, result-driven mission that requires every sector, every level of government, and every community to play its role. No one will be left behind in the fight against TB, because ending TB requires all of us.”