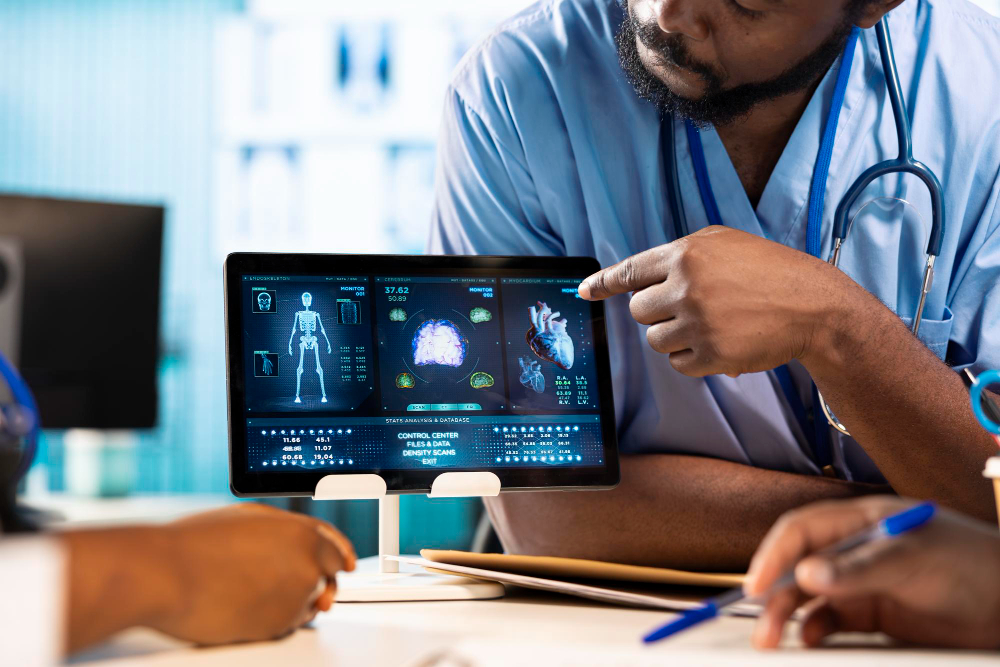
The project plans to integrate Artificial Intelligence into 1,000 primary healthcare clinics for drone deliveries, telemedicine, diagnosis and virtual consultation in Kenya, Rwanda, Nigeria and South Africa by 2028.
The Gates Foundation and OpenAI have committed $50 million (about Ksh6.4 billion) to support the integration of Artificial Intelligence (AI) in health systems in Rwanda, Kenya, Nigeria and South Africa. The initiative, dubbed Horizon1000, began as a pilot in Rwanda before rolling out to the other three countries. The goal is to reach 1,000 primary healthcare clinics and their surrounding communities by 2028.
The driving force behind the investment is straightforward: Sub-Saharan Africa faces a shortage of more than 5.6 million healthcare workers, and conventional hiring and training cannot close that gap in any reasonable timeframe.
The numbers tell a stark story. In Kenya, the Economic Survey of 2025 found that the country averages 30 doctors, nurses and clinical officers per 10,000 people; well below the World Health Organisation (WHO) recommendation of 45 per 10,000. In concrete terms, Kenya has 14,000 doctors and dentists, 75,000 registered nurses and 31,000 clinical officers serving a population of over 52 million. This means one doctor serves 5,263 people, compared with the WHO recommendations of one doctor per 1,000 people in 2015 and one doctor per 600 people in 2020.
A February 2026 publication by the Institute of Public Finance (IPF) offers some context: Kenya’s healthcare workforce doubled to over 162,233 in 2020, up from 77,417 in 2010. Even so, this number addresses only 76.4 per cent of the estimated need. Without further action, coverage could fall to 60 per cent by 2035.
Rwanda’s situation is equally pressing. The country has one healthcare worker per 1,000 people, against the WHO recommendation of four workers per 1,000. At the current pace, it would take 180 years to close that gap. Rwanda is, however, implementing a 4-by-4 initiative to achieve 4 doctors per 1,000 people.
In Kenya, around 800 nurses leave the country annually in search of career opportunities in the UK
Beyond numbers, poor working conditions, low pay and limited career opportunities are fuelling the exodus of skilled workers from the continent. In Kenya alone, around 800 nurses leave the country every year in search of better salaries and career opportunities in the UK, the US and Canada. Kenya contributes 6.5 per cent of nurses seeking VisaScreen certification, a key credential for foreign-trained health workers seeking to practice in the US.
The partnership between the Gates Foundation and OpenAI will provide funding, technology and technical support to African leaders pioneering AI in health. In his announcement, Bill Gates was clear about what the tools are intended to do: “These AI tools will support health workers, not replace them.” He drew a direct comparison with how AI is already being used in wealthier countries, where doctors can now focus entirely on patients while AI handles note-taking and administrative tasks, thus eliminating divided attention.
Gates acknowledged significant progress in global health, including a 50 per cent reduction in child mortality over the past 25 years. Yet he was candid about what remains unresolved. Sub-Saharan Africa records the world’s highest child mortality and faces a shortfall of nearly six million healthcare workers. “It’s a gap so large that even the most aggressive hiring and training efforts can’t close it in the foreseeable future. These shortages put healthcare workers in an impossible situation,” he said.
That impossible situation forces healthcare workers to manage large numbers of patients with little administrative support, limited technology, and outdated clinical guidance. The WHO has acknowledged that poor quality care causes between six and eight million deaths worldwide.
The countries selected for Horizon1000 share several common characteristics: critical shortages of healthcare workers, infrastructure gaps, dependence on foreign aid, a priority focus on improving healthcare access for pregnant mothers and HIV patients, and – crucially – a demonstrated commitment to integrating innovation in their health systems.
Kenya has over 100,000 Community Health Promoters in 47 counties ideal for AI-assisted diagnostics
Rwanda stands out as the most advanced of the four. The country established the National Health Intelligence Centre (NHIC) AI Laboratory in Kigali in 2025, making it a regional leader in AI integration. It has leveraged partnerships with firms such as Zipline for drone blood deliveries and Babylon Health (Babyl) for AI-powered telemedicine.
The Babyl app offers symptom checking and virtual doctor consultations and has over two million users. The platform processes Kinyarwanda and is accessible offline. Rwanda has also trained over 60,000 community health workers to use AI tools for real-time diagnostic support, managing 50 per cent of malaria cases through these workers.
This points directly to an opportunity for Kenya. With over 107,000 Community Health Promoters already deployed across all 47 counties, Kenya has the human infrastructure to replicate and potentially scale what Rwanda has achieved in community-level AI-assisted diagnostics.
Kenya is set to benefit from Horizon1000 after Rwanda, and it is not starting from scratch. In 2025, Kenyan researchers from the Ministry of Health, the University of Southern California’s Keck School of Medicine, Microsoft AI for Good Lab and Amref Health Africa jointly developed an AI model capable of predicting acute child malnutrition up to six months in advance, with over 89 per cent accuracy.
At the county level, Uasin Gishu and Kisumu have partnered with Elsmed Healthcare Solutions, Zipline and Kenya Flying Labs, respectively, to deliver vaccines, blood, specimens and emergency medicines to over 400 facilities. Through the Digital Health Act signed into law on 19 October 2023, Kenya established the Digital Health Agency, a government body tasked with transforming healthcare delivery through modern digital technologies.
AI is the third major discovery to transform medicine, after vaccines, antibiotics
Dr Patrick Amoth, Director General at the Ministry of Health, has urged researchers and clinicians to embrace AI to help make sense of complex health data. “Science and research are pillars of strong health systems and sustainable development. Too much evidence remains underutilised, not informing policy or guiding programmes and thus not improving lives,” he said at the inaugural STAR National Science Research Translation Congress in Nairobi.
Rwanda’s Minister of Health, Dr Sabin Nsanzimana, captured the stakes plainly at the announcement of the Gates-OpenAI deal: “AI is the third major discovery to transform medicine, after vaccines and antibiotics.” He noted that the National Health Intelligence Centre would help the available healthcare workers achieve better results at a time of scarce resources.
Gates framed the broader vision in terms that go beyond technology: “I believe this partnership with OpenAI, governments, innovators and healthcare workers in Sub-Saharan Africa is a step towards the AI we need more of: systems that help people solve generational challenges they didn’t know to address before.”
The message is that AI is not arriving in Africa as a luxury add-on. For health systems stretched far beyond their limits, it may be the most practical tool available.