The hardest part of making a vaccine is not the science. It is the last dirt road, the missing fare, the mother who never heard her baby’s death had a name.
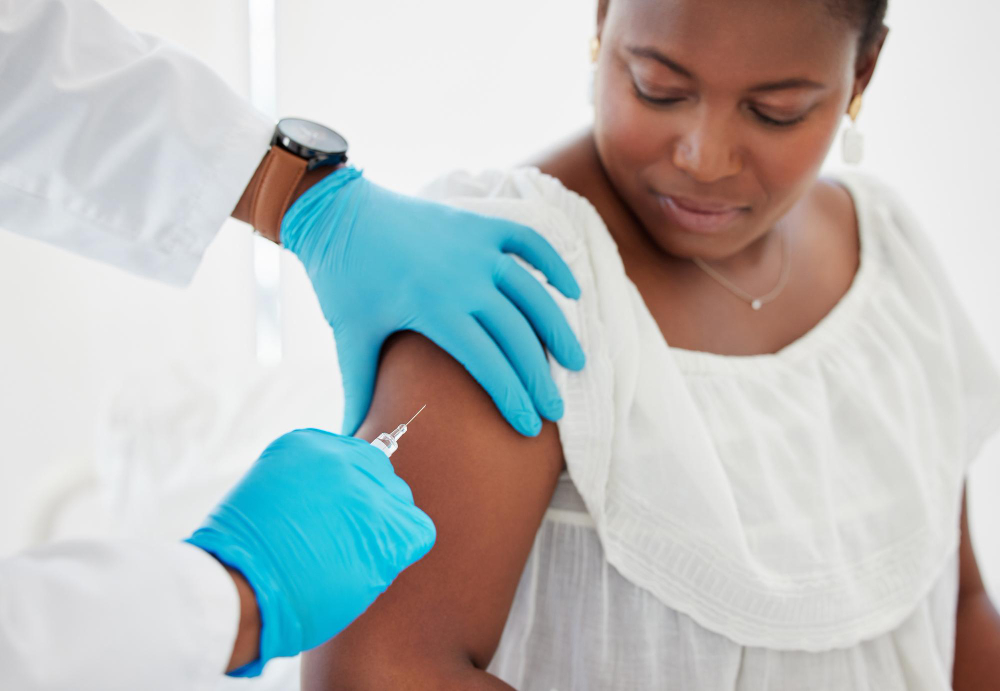
For many pregnant women in Kenya, distance, cost and weak diagnostics stand between them and lifesaving care. Now, a new challenge is taking shape: when a maternal vaccine for Group B Streptococcus (GBS) becomes available, will it reach the women who need it most – or repeat the familiar pattern of new technologies benefiting the few while bypassing the many?
That question dominated discussions last week at the 4th International Symposium on Streptococcus agalactiae Disease (ISSAD) conference in Nairobi, Kenya, where clinicians, policymakers and researchers confronted the gap between the promise of prevention and the realities of health systems that still struggle to reach women at the last mile.
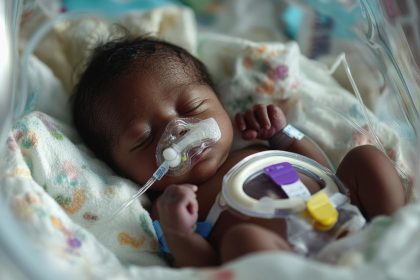
The stakes are significant. While GBS is best known as a cause of newborn sepsis and meningitis, growing evidence links it to maternal sepsis, stillbirth and preterm labour. A global fact sheet estimates that GBS contributes to more than half a million preterm births each year, alongside tens of thousands of deaths and cases of lifelong disability.
Scientists at the conference projected that a maternal GBS vaccine could potentially avert 127,000 early-onset infections, 87,300 late-onset infections, 31,100 deaths, nearly 18,000 cases of neurodevelopmental impairment, 23,000 stillbirths and 185,000 preterm births annually. For Kenya, where an estimated 134,000 babies are born prematurely each year, the promise of prevention is powerful.
Kenya’s maternal health focus has traditionally centred on haemorrhage, obstructed labour and hypertensive disease. GBS has barely featured. Dr Simon Kigondu, a gynaecologist and President of the Kenya Medical Association (KMA), told delegates that this may mean the country is misreading its own data.
We see preterm delivery, growth restriction and neonatal infections, but not routinely test for GBS
“Some of the perinatal morbidity and mortality we see may actually be attributed to Group B Streptococcus,” he said. “We see preterm delivery, growth restriction and neonatal infections, yet we do not routinely test for GBS. If there is a vaccine that is affordable, effective and safe, then primary prevention would be a very good way forward.”
But introducing a maternal GBS vaccine would require national policy shifts and new financing pathways. Dr Kigondu warned that even existing antenatal tests stretch public facilities. “Testing for GBS is not routine, and financing is already an issue,” he said. “If we introduce screening or vaccination, it has to be supported by policy and by a funding mechanism, possibly through social health insurance, so that women delivering in public hospitals can access it.”
Kenya’s Social Health Authority (SHA) reforms aim to expand coverage for essential services, but whether a future maternal vaccine would be included in benefit packages remains uncertain. Without reimbursement, uptake could be confined to urban private facilities and thus deepen inequality.
Vaccine acceptance depends on confidence, and for maternal immunisation, safety concerns are magnified because two lives are involved. Dr Martha Mandale, Principal Regulatory Officer at the Pharmacy and Poisons Board (PPB), said Kenya has pharmacovigilance systems but must strengthen them for pregnancy-specific use.
“We must be able to track vaccine exposure in pregnancy and link it to outcomes for both mother and baby,” she said. “At the moment, we rely heavily on passive reporting, which leads to under-reporting. Active surveillance will be critical for maternal vaccines.”
Before we talk about acceptance, we have to know whether a woman knows the vaccine exists
Kenya is already working with regional partners and the WHO to strengthen safety monitoring for other maternal vaccines such as RSV (Abrysvo). These efforts could be adapted for a future GBS vaccine, helping regulators detect rare adverse events and maintain public trust.
Even with policy and safety systems in place, experts said Kenya’s biggest challenge lies at the community level. Prof Violet Naanyu, a social scientist at Moi University, argued that access begins with awareness, and that awareness alone is not enough.
“Before we talk about acceptance, we have to talk about whether a woman even knows the vaccine exists,” she said. “Then willingness, then reach. Distance is not just kilometres, it is fare, permission from a husband, complicated registration systems and how she is received at the facility.”
Drawing on lessons from HIV prevention programmes, she described how decentralised services and simple explanations in local languages transformed uptake. “There was not a single woman who refused when she understood what the intervention was and why it mattered,” she said.
Her concern is that maternal GBS vaccination could fail if rolled out without addressing clinic hours, staff shortages, hidden fees and digital systems that exclude low-literacy users. “Equity is not equality,” she said. “Some women need more support than others to reach the same outcome. That is the last mile.”
Addressing GBS means integrating it into antenatal care, infection prevention, maternity care
Mary Muriuki, Principal Secretary at the Ministry of Health (MoH), said prevention remains central to Kenya’s vision for universal health coverage. “Addressing Group B Strep means integrating it into antenatal care, infection prevention, nutrition services and respectful maternity care,” she said. “Quality should not be reserved for a few facilities. It must be the standard everywhere a woman gives birth.”
She highlighted the role of Kenya’s community health promoters, who visit households to monitor pregnancies and encourage clinic attendance – workers who could be key to building awareness and demand for maternal vaccination. “Public health is most powerful when it reaches everybody, urban or rural, affluent or vulnerable,” she said.
Several GBS vaccine candidates are in late-stage development. Unlike childhood vaccines, maternal immunisation relies on antibodies crossing the placenta to protect newborns in their first months of life, making timing and dosing critical. Cold-chain capacity, supply security and affordability will shape how quickly Kenya can adopt any approved product. Past experience with COVID-19 and RSV vaccines shows that delayed access for low-income countries can widen global inequities.
We must go upstream and address structural, economic and cultural barriers
Kenya shows partial readiness: strong political commitment to maternal and newborn health, existing antenatal vaccine platforms, expanding safety surveillance systems and community health networks that can support awareness. But gaps remain. There is no national GBS burden data, financing is uncertain, the linkage between maternal and newborn records is weak, and last-mile barriers driven by poverty and overstretched services persist.
Dr Kigondu summed up the dilemma plainly. “We do not yet know how much GBS contributes to our poor outcomes. But that should not stop us from preparing.”
Prof Naanyu offered a final warning that framed the challenge in its broadest terms. “We must go upstream and address structural, economic and cultural barriers,” she said. “Otherwise, the women most at risk will benefit last.”
The promise of a GBS vaccine is not just fewer infections, but fewer premature births, fewer stillbirths and fewer maternal deaths. Whether that promise is realised will depend less on the vial itself and more on Kenya’s ability to deliver it safely, affordably and all the way to the last mile.