A rare bone disease had been consuming Lucy Gathoni’s face for over a decade. What surgeons did next was a complicated, but successful surgery for the record books.
Who is Lucy Gathoni, and what is her condition?
Lucy Gathoni has lived with a rare and relentless disease since she was 12 years old: severe craniofacial fibrous dysplasia. In simple terms, it is a bone disorder where normal, healthy bone is replaced by fibrous, scar-like tissue. Instead of strong bone forming in the skull and face, weak, abnormal tissue grows in its place, creating tumours that continue to expand.
The condition is extremely rare, affecting roughly one in 30,000 people worldwide. In Lucy’s case, it was even more complex. The disease did not remain confined to one part of the face. It affected both her upper jaw, known as the maxilla, and her lower jaw, the mandible, extending toward the base of her skull.
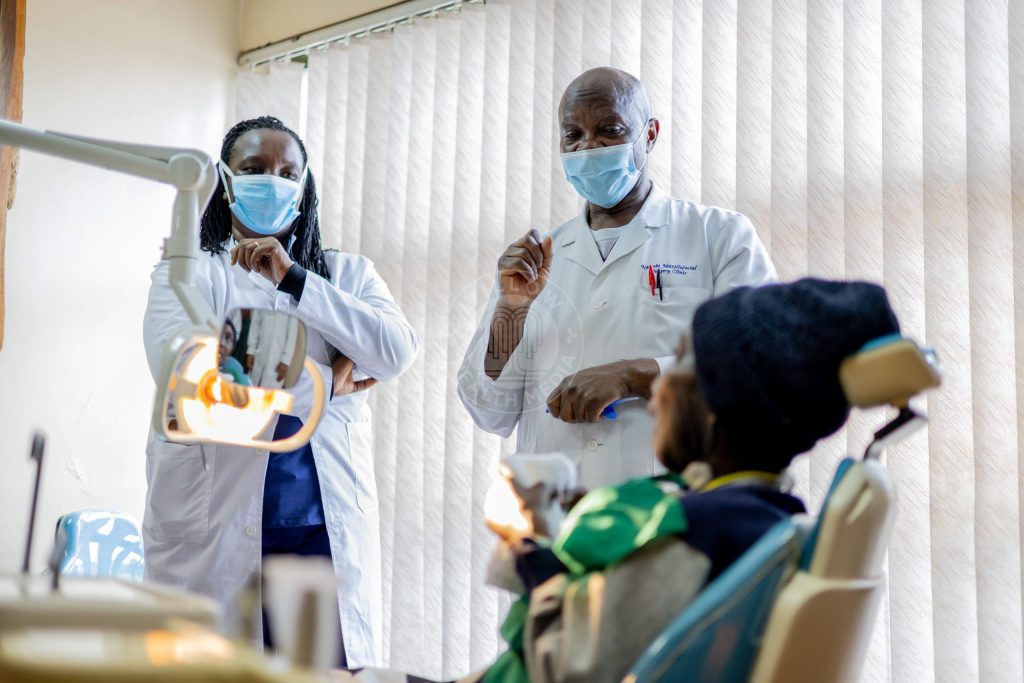
As Prof Symon Guthua, the oral and maxillofacial surgeon who led the procedure, explained: “Usually in the past, the tumours have been in one jaw, either the upper jaw, called the maxilla, or the lower jaw, called the mandible. But this time it is both jaws. And not both jaws with simple growth, the upper jaw almost went to what we call the cranial base.”
Over the years, the tumours grew relentlessly. Earlier surgeries attempted to remove them, but they kept returning, larger and more invasive each time. The abnormal bone progressively deformed Lucy’s face, blocked parts of her airway, making breathing difficult, and turned eating and speaking into daily struggles. By the time she went into surgery, she weighed just 33 kilograms.
How do you plan a surgery with no blueprint?
Planning for the operation began in 2023. But before anyone could begin surgery, the medical team had to solve a problem with no clear precedent. Lucy’s face had been so altered by the disease that the most basic question had to be answered first: what exactly were they rebuilding toward?
The answer came from technology.

Using Lucy’s CT scans from 2015, taken before the tumours had expanded dramatically, the team created a digital blueprint of what her face should look like.
Dr Margaret Mwasha, the prosthodontist on the team, explained: “Technology has allowed us to use a patient’s CT scan to do what is called virtual resections, virtual reconstruction, and virtual rehabilitation before any procedures are done. We looked at the tumour, we looked at its extent in both the upper and lower jaw, and that guided us in terms of what design we were looking at because we knew what bones needed to be replaced.”
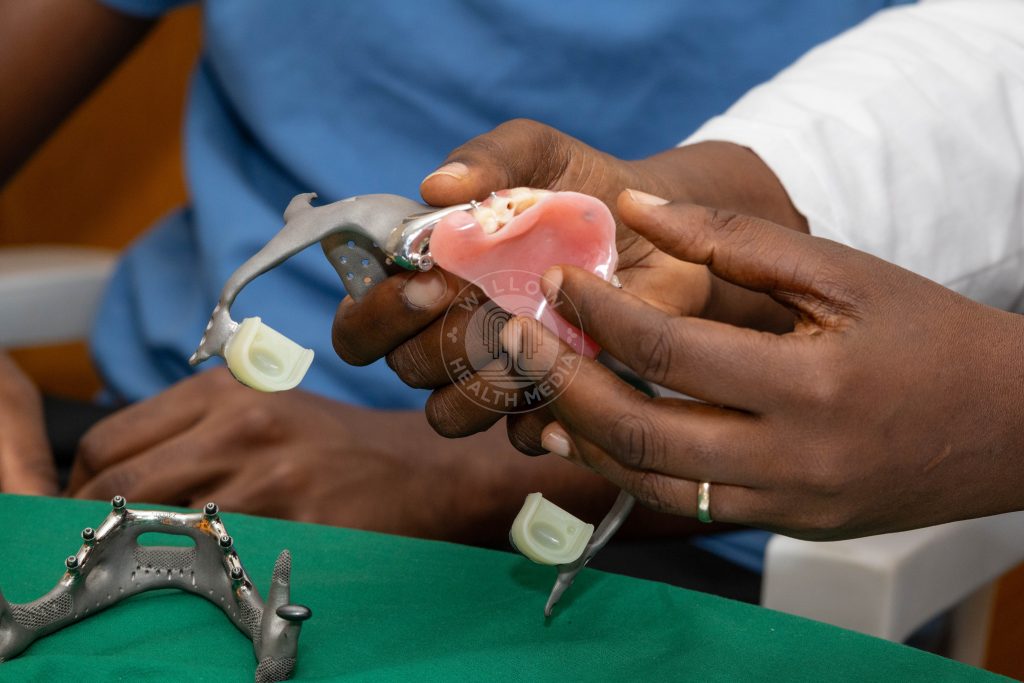
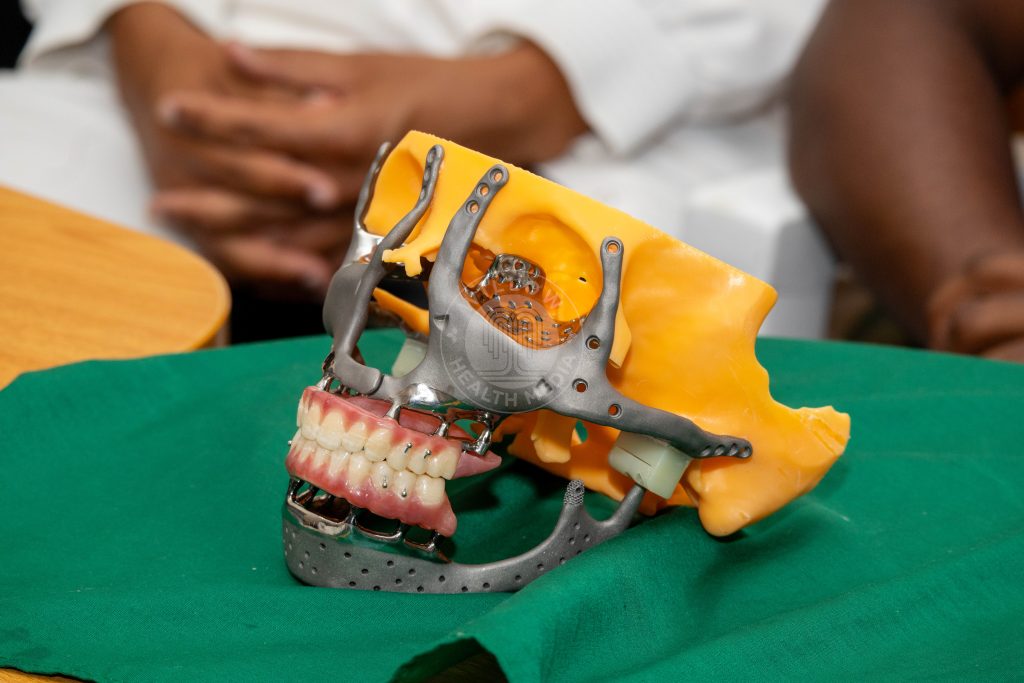
From that digital blueprint, the team designed patient-specific titanium implants, custom-made down to the millimetre, to rebuild Lucy’s entire jaw and midface.
The reconstruction plan included a titanium lower jaw, midface components to restore the upper jaw, fixed dentures for both upper and lower teeth, artificial joints to allow the jaw to move naturally, and a removable palate to restore the roof of her mouth so she could eat and speak.
Two days before surgery, the team held a full rehearsal. Every doctor reviewed Lucy’s case. Every implant, screw, and instrument was confirmed to be ready.
What happened inside the operating theatre?
On 18 April 2025, the procedure began at 6:50am at the Nairobi Hospital.
What followed was 18 and a half hours of careful, sequential surgery, like assembling a complex puzzle in which every step had to occur in the correct order. More than ten specialists and medical students were present throughout the operation.
The first phase focused on removing the tumours.
By 9:55am, the team had begun extracting the first tumour from Lucy’s upper jaw. It weighed 1.1 kilograms and, together with the second tumour, represented nearly 10 per cent of her entire body weight.
Nearly seven hours later, when the final tumour was removed, the operating theatre broke into spontaneous applause.
The reconstruction phase began at 5:15pm and continued into the early hours of the following morning, finishing at 1:20am.
The surgical team worked through eight precise stages: positioning the left midface implant to rebuild the left side of her upper face and eye socket; placing the matching implant on the right side to restore symmetry; attaching the upper denture; positioning the artificial jaw joints known as condyle boxes; aligning and fixing the titanium lower jaw; closing the joints to allow natural movement; fitting the lower dentures; and finally placing a removable palate to restore the roof of her mouth.
Prof Guthua described the most critical element of the entire reconstruction: “The main turning point for this operation is that joint as small as it looks, if that works, the midface is not an issue. This is the only joint in the body that is C-shaped, the only one which opens and closes and helps you eat. We were going to reproduce it. And we were hoping and praying that it works.”
What makes the implant itself remarkable?
Every part of Lucy’s implant was designed not only for structure but also for long-term durability.
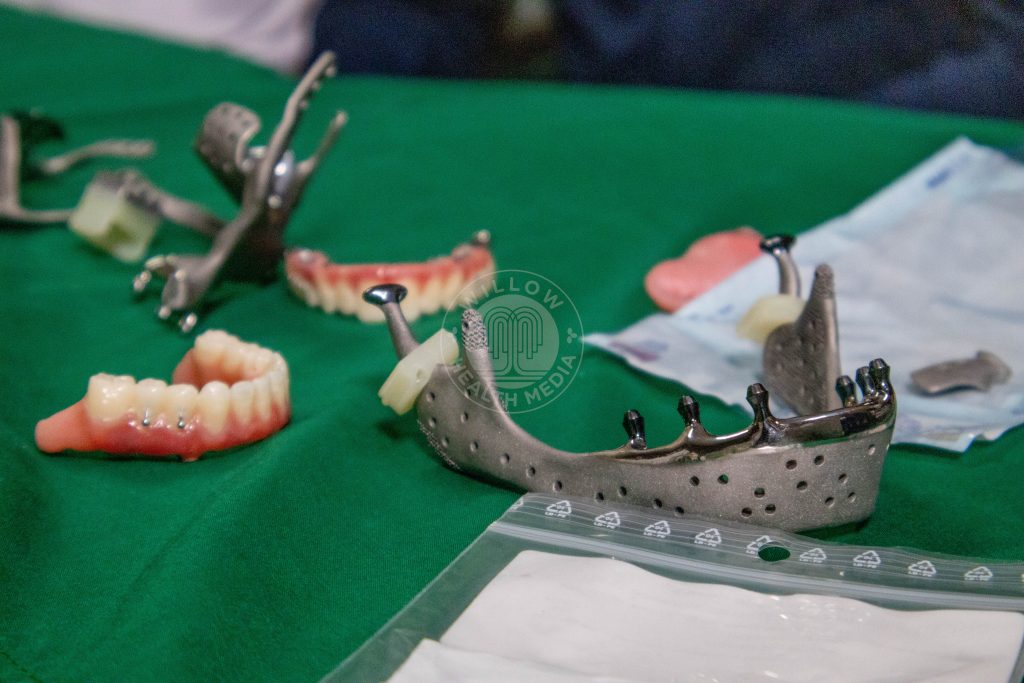
Dr Mwasha explained one detail that shows the level of planning involved: “If you look at the condyle heads, the parts that move, there is a black coating. It is called a diamond-like coating. Anytime you have two parts moving together, you get friction, and from friction, you get residue. This coating is intentionally designed to reduce friction, and even where friction occurs, the components will not irritate surrounding tissue. It increases the longevity of the whole reconstruction.”
The implant also included coronoid processes, small projections built specifically to give Lucy’s temporalis muscle, one of the main chewing muscles, a place to reattach.
Without these structures, the jaw would not be able to move.
Prof Guthua explained their importance: “These are not for beauty. They are meant to hold the muscles that we are going to reattach to facilitate movement on both sides.”
What has this surgery restored, and what comes next?
For years Lucy’s tumours had interfered with three of the most basic human functions: breathing, eating, and speaking.
Dr Mwasha described the impact of the surgery simply: “Her whole life will be transformed. She is a young woman who has struggled all her life. Breathing has been interfered with. Feeding has been interfered with. How she looks has been affected. It has quite severely interfered with her quality of life.”

After surgery, Lucy’s mouth was temporarily sealed so that tissues, muscles, and implants could heal in the correct position before normal jaw movement resumed.
She was fitted with a gastrostomy tube to receive liquid nutrition during the early stages of recovery. In the coming months, she will also undergo facial therapy, a specialised rehabilitation process that helps patients relearn how to move facial muscles, chew, swallow, and speak after major reconstructive surgery.
According to Dr Mwasha, complete replacement of the lower jaw, such as Lucy underwent, has only one other documented case anywhere in the world.
In a country where access to specialist surgical care remains deeply unequal, what happened at the Nairobi Hospital on 18 April 2025 represents more than a medical milestone.
It shows what becomes possible when advanced technology, surgical skill, and meticulous planning come together and how far Kenya’s capacity for complex reconstructive surgery has progressed.

The Facial Reconstruction Steps
(Reconstruction began at 5:15pm and concluded at 1:20am the following morning)
Step 1: The left side of her upper face and eye socket was restored first using a custom-made implant screwed into place at 5:15pm.
Step 2: The right side was rebuilt to mirror the left, restoring facial symmetry.
Step 3: Her new upper teeth were attached.
Step 4: Artificial jaw joints were positioned where the jaw connects to the skull.
Step 5: The titanium lower jaw was aligned and fixed into place, connecting to the joints.
Step 6: The joints were closed, allowing Lucy’s jaw to move naturally up, down, and side to side.
Step 7: Her new lower teeth were fitted, completing a full set of teeth.
Final Step: A removable palate was placed to restore the roof of her mouth so she could eat and speak again at 1:20am.
Key Terms Explained
Craniofacial fibrous dysplasia: A rare condition where bones in the face and skull become soft and weak, forming growing lumps that can change the shape of the face.
Intubation: Placing a tube in the throat to help a patient breathe during surgery.
Titanium implants: Strong, lightweight metal parts placed in the body to replace damaged bone.
Condyle/condyle box: The rounded joint at the top of the lower jaw that lets the mouth open and close. The condyle box is the artificial version used in surgery.
Coronoid processes: Small parts of the jawbone where chewing muscles attach, helping the jaw move.
Temporalis muscle: A muscle on the side of the head that lifts the jaw when you bite.
Gastrostomy tube: A tube placed directly into the stomach to give liquid food when someone cannot eat by mouth.
Tracheotomy: A small opening made in the front of the neck to help a patient breathe when the normal airway is blocked.
Diamond-like coating: A very hard thin layer added to implants to reduce friction and wear.