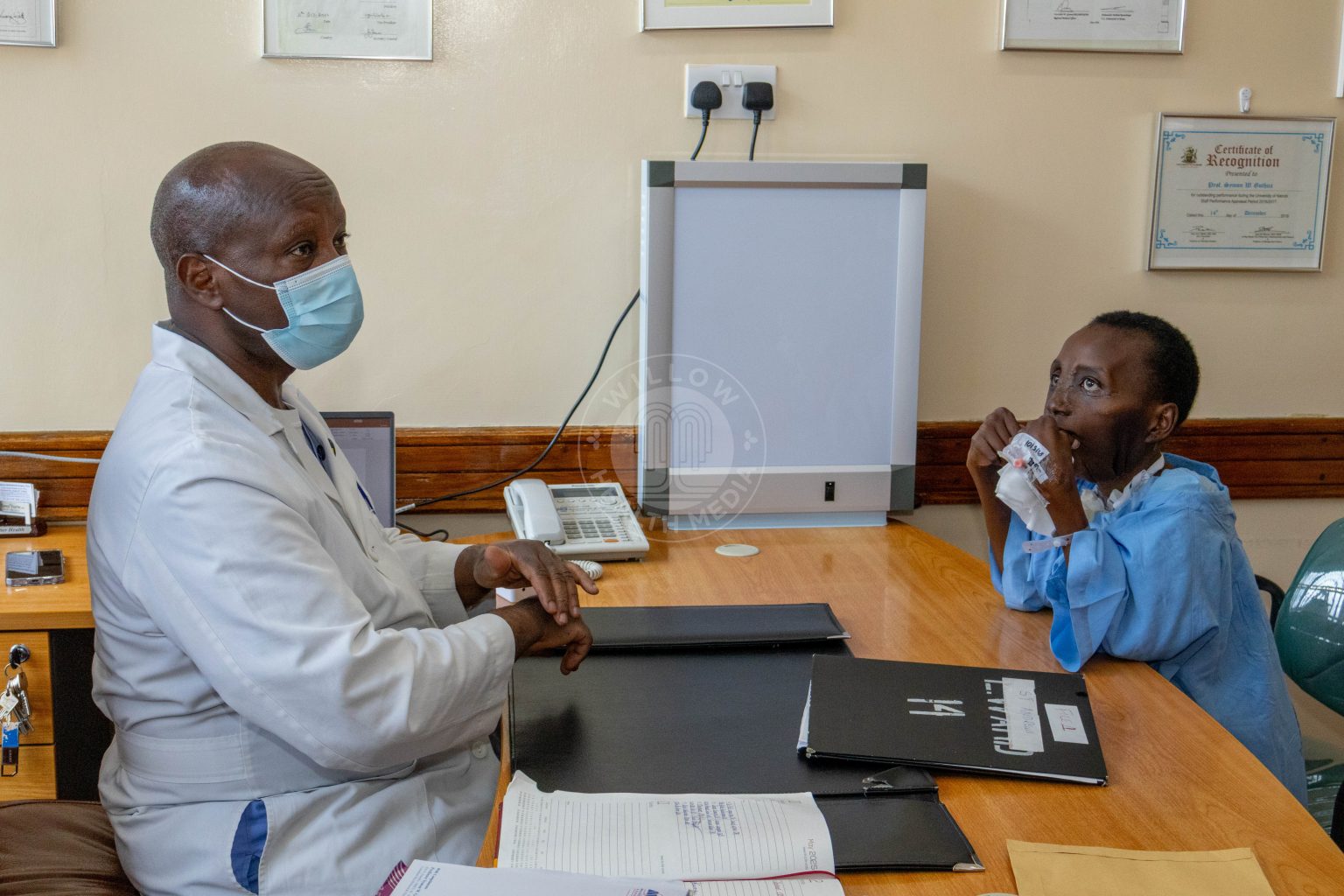
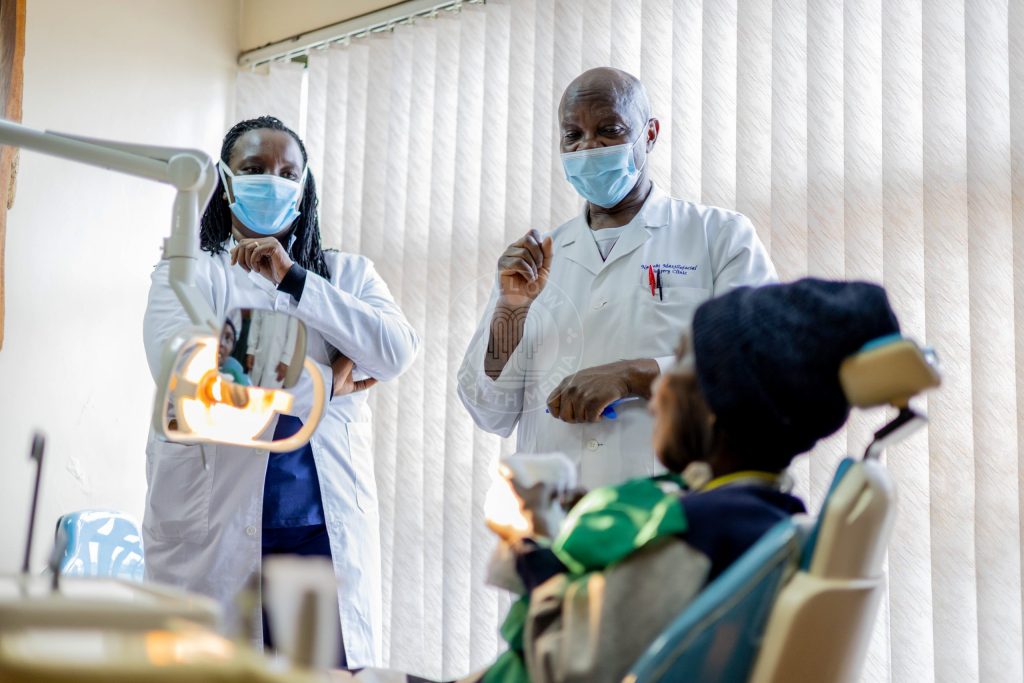
A team of doctors at Nairobi Hospital spent 18 hours that Good Friday in 2025, and ‘When surgery finally began, the danger proved even greater than anticipated,’ recalls lead surgeon Prof Symon Guthua.
On the morning of Good Friday 2025, while Kenyans marked a day of quiet reflection, a different kind of revelation was unfolding inside an operating theatre at Nairobi Hospital. For 18 and a half hours, a multidisciplinary team of doctors were performing a medical miracle on a 28-year-old woman whose face had been overtaken by a massive tumour, leaving her barely able to breathe.
Her name is Lucy Gathoni. This is the story of the doctors who faced what many would consider impossible- and chose to proceed anyway.
Prof Symon Guthua: Confronting the impossible tumour
“Usually, in the past, the tumours have been one jaw,” explains Prof Symon Guthua, the maxillofacial surgeon who led the operation. “Either the upper jaw, called the maxilla, or the lower jaw, called the mandible. But this time, it is both jaws.”
He pauses, as if still absorbing the scale of the challenge.
“And not both jaws, but both jaws with very complicated growth. The upper jaw almost went to what we call the cranial base.”
By the time Lucy arrived at Nairobi Hospital on a Wednesday in 2025, years of unchecked growth had left her disfigured and struggling to eat, speak, or breathe. Prof Guthua describes her condition as having reached “a point of desperation.”
When surgery finally began, the danger proved even greater than anticipated.
“This tumour was highly vascularized, particularly on the right side,” he recalls. “That was something that, of course, worried one.”
Highly vascularised meant a severe risk of bleeding. Removing the tumour would require precision, endurance and resolve.
Asked what drove him forward, Prof Guthua reflected on the moment and the meaning of the day.
“Since you’re helping patients, I think the motivation is that you want to change their lives. This lady has been suffering for a very long time. She has come to a point of desperation. So the fact that you can change her life at this time of Easter, Good Friday, when Jesus suffered for all of us, and now you’re asked to suffer a little bit for somebody, I think it’s very important that you do that.”

Dr Kinyua Gathukia: Guarding the airway, guarding life
Before a scalpel could touch the tumour, Lucy’s survival depended on a different kind of battle.
Dr Kinyua Gathukia, an anaesthesiologist, describes himself and his colleagues as “the unseen guys behind the surgeries.” Yet in Lucy’s case, his role would determine whether surgery was even possible.
“Her case is unique because ordinarily our biggest challenge is the airway,” he explains, seated beside the “cockpit” – a wall of monitors that would guide him for more than 18 hours. “Without oxygen, basically, you cannot survive. So, our primary goal is to make sure that the patient is able to breathe, or we are breathing for them.”
The tumour had distorted Lucy’s face so severely that normal intubation was impossible. Any misstep could mean losing the airway completely.
“We would not want to do anything drastic or anything major so that we lose the airway and be in trouble,” Dr Gathukia recalls.
The solution was careful sedation, followed by a tracheostomy performed by ENT surgeons, placing a tube directly into her trachea through the neck. Only then could surgery proceed.
Throughout the operation, Dr Gathukia managed massive blood loss and a complex balance of medications.
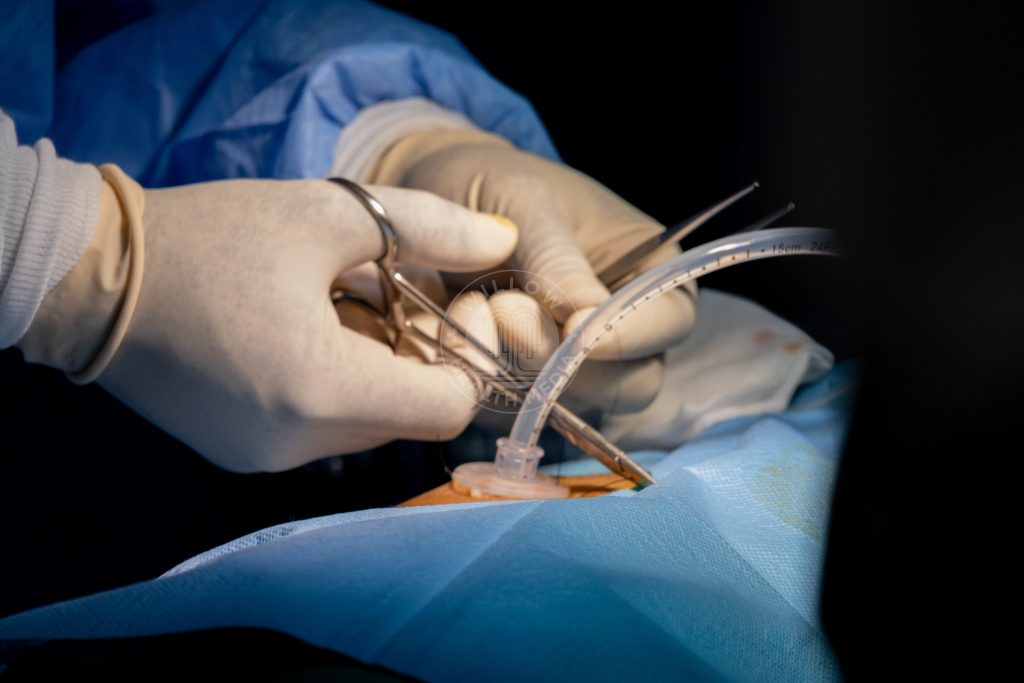
“I’ve given her quite a bit of blood,” he says. “This is to compensate for the blood loss during the surgery and to help her through the healing.”
He also addressed a common misconception about anaesthesia.
“One might assume that if you are under general anaesthesia, you don’t feel pain, but that’s not the picture. If you’re not given pain medication during general surgery, you still feel the pain.”
For 18 and a half hours, he monitored every breath, every heartbeat.
“We usually say we are the unseen guys behind the surgeries. Most of the time, it’s ‘the surgery was done.’ But nobody asks how it was done, whether there was another doctor who was there. But we are always there.”
Dr Margaret Ndung’u Mwasha: Rebuilding a face, restoring a Life
While the operating room battle unfolded, another part of Lucy’s journey had begun years earlier.
Dr Margaret Ndung’u Mwasha, a prosthodontist, had been planning Lucy’s reconstruction since 2023. Using CT scans from as far back as 2015 – before the tumour reached its devastating size – she virtually mapped every step of what would need to be rebuilt.

“Technology has allowed us to do what is called virtual resections, virtual reconstruction, and virtual rehabilitation before the procedures are done in the mouth,” she explains. “We looked at the tumour. We looked at the extent of the tumour, both the upper jaw and the lower. That really guided us in terms of what sort of design we were looking at.”
Her goal was simple in principle, daunting in practice: restore form, function and aesthetics.
“Those are the basics,” she says.
After surgery, she watched closely for signs that the reconstruction would hold.
“Just looking at the processes, looking at the jaw, looking at the fact that the mandible is able to move up and down, I think for me that is, I would almost say, a miracle. It is a miracle.”
Despite “a few challenges here and there,” the implants seated well, and recovery looked promising.
More Than a Surgery: This could have been at a very huge cost to the patient
Dr Mwasha is careful to stress that Lucy’s survival was not the work of one individual.
“We must mention that we are grateful to Nairobi Hospital for giving us this opportunity, for giving the patient the opportunity to get treatment here. This is a multidisciplinary team approach. This hospital has been very gracious in allowing us to have the patient here, having all the team members, the use of equipment. We can’t take this lightly. This would have been at a very huge cost to the patient.”
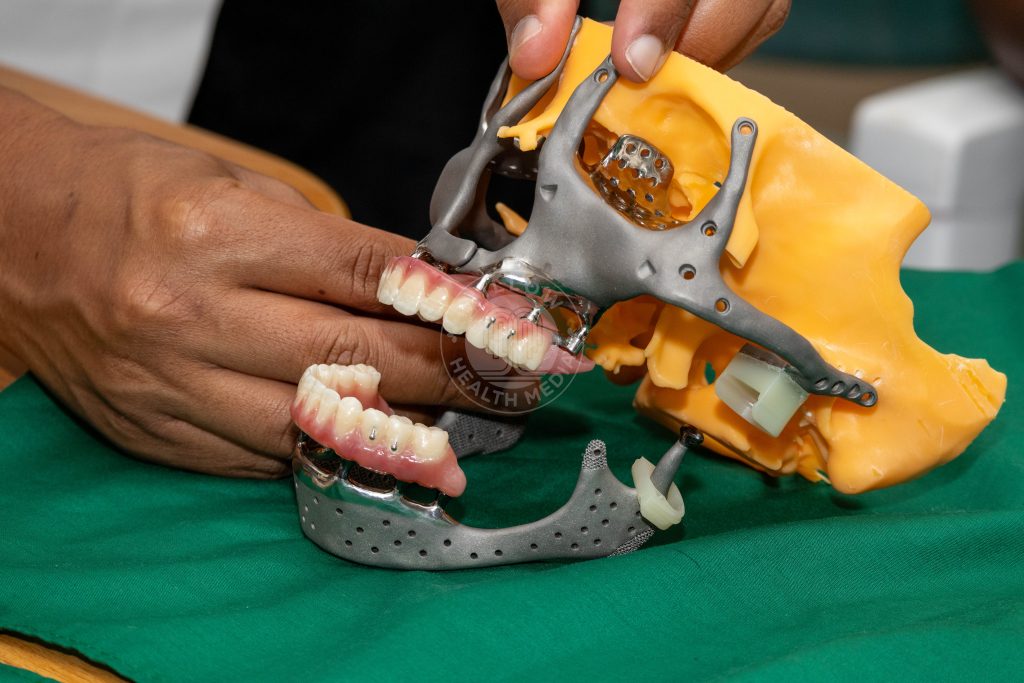
She also acknowledges the wider community- benefactors such as Bishop Muheria and Father Joseph- who supported Lucy when she had reached her lowest point.
“It’s been a really, really long journey.”
Today, Lucy is recovering at home in Othaya. She can speak. She can walk. She can breathe without struggle. The pain that once defined her life is gone. Though she continues to feed through a tube and will need regular follow-ups, her progress is unmistakable.
Eighteen and a half hours in an operating theatre gave Lucy back what years of suffering had taken away: dignity, breath, and a future. For the doctors who stood by her on Good Friday, it was a reminder that some lives are saved not by miracles alone, but by skill, sacrifice and the refusal to walk away from the impossible.