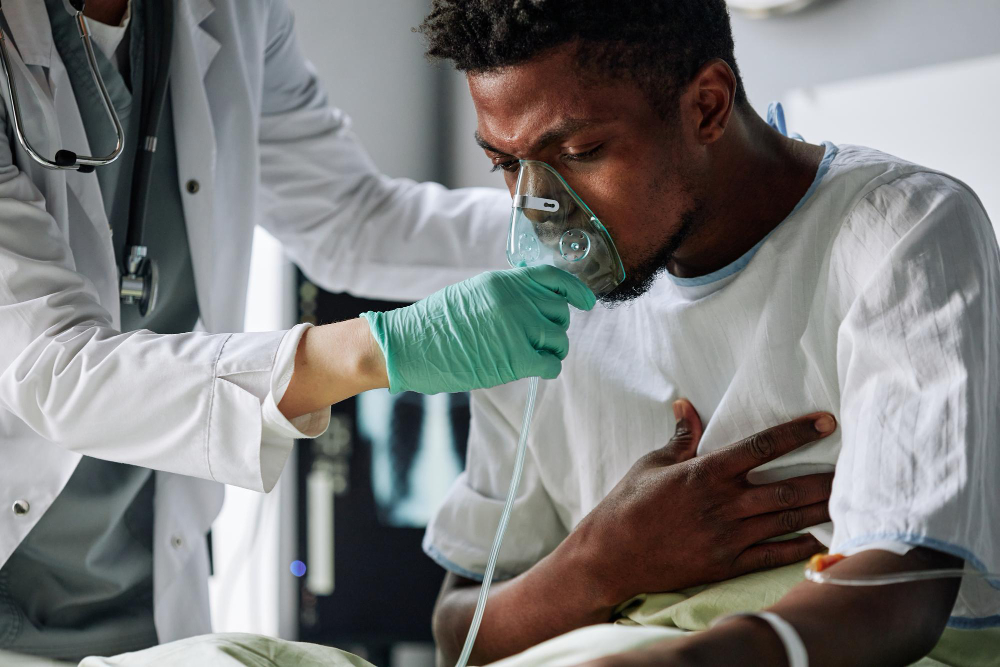
Men are more biologically susceptible to TB, more likely to delay seeking care, less likely to complete treatment, and more likely to be missed by a health system that was not designed with them in mind. Smoking, alcohol use and HIV only worsen the situation.
Kenya has a tuberculosis problem, with men carrying the heaviest burden in the country and for myriad reasons: Men are the least likely to seek care early, but the most likely to be missed by a health system that was never quite built for them. Researchers, clinicians and health policy makers have known this for years. What they are only beginning to grapple with seriously is why, and more importantly, what to do about it.
A convergence of biology, cultural norms, occupational hazards, and structural neglect has left men both more exposed to TB and less likely to survive it. The good news, emerging from clinics, communities and research, is that targeted, practical interventions are working where they have been tried. The harder question is whether those lessons can be scaled before more men are lost to a treatable disease.
That question was at the heart of a study released on March 16 ahead of this year’s World TB Day, by researchers under the LIGHT Consortium, Ministry of Health and National TB Programme, Respiratory Society of Kenya (ReSOK).
The study, A National Community Rights and Gender Assessment, under the Leaving no-one behind: Transforming Gendered Pathways to Health for TB (LIGHT) research programme, explored how social, legal and gender-related factors influence access to TB services. Its findings were stark: men are not only more biologically susceptible to TB, but they are also more likely to delay seeking care, less likely to complete treatment, and more likely to be missed by a health system that was not designed with them in mind.
“We have known, for a long time, that men have a higher burden of TB than women, but we are not completely sure why,” the researchers stated.
Mining, informal jobs, crowded political and sporting events increase men’s exposure to TB
The study, supported by UKAID and the Liverpool School of Tropical Medicine, acknowledged that biology plays a role. “Low levels of oestrogen and androgens make men more susceptible to TB infections and progression. Oestrogen and androgens modulate immunity,” it stated. Conditions that compound TB risk, among them smoking, alcohol use and comorbidities such as HIV, intensify the infection further in men.
But biology alone does not explain the scale of the gap. Occupational and socio-economic factors carry significant weight. Mining, informal jobs in construction and industry, and crowded settings such as political and sporting events increase men’s exposure to TB in ways that few workplace or public health policies have adequately addressed.
The more complex and persistent barrier is behavioural. “Lower health-seeking behaviours among men, often characterised by delayed care, avoidance of preventive services, and reliance on self-medication, deter diagnosis and treatment,” the study found. These behaviours are not random. They emerge from a complex interplay of cultural norms, masculinity, and structural barriers that shape how men understand illness and what they are willing to do about it.
Tony, a young man who sought anonymity during the study, was diagnosed with TB and faced stigma when taking his medication. “When I’m feeling unwell, I always start seeking medication from the chemist. It’s not easy for us to come to the hospital unless the sickness has persisted,” he said.
His experience resonates widely. Veteran writer and editor Ted Malanda cited cultural beliefs and masculine tendencies as barriers, asking: “How do you tell a man who owns a homestead to remove trousers?” Daniel W’Obukosia observed that “a man will even service his car in a garage while seriously ill.” Kipkorir Ruto argued that “men don’t go to hospitals because diagnosis kills faster than the disease.” Mutugi Njue pointed to intrusive and uncomfortable medical procedures as deterrents, asking: “Try getting checked for prostate cancer, you’ll know why?” Gloria Makokha observed that men are afraid of drugs and injections.
Men typically engage in self-treatment first, then local pharmacy and hospital last, when all else fails
The consequences of delay are not abstract. Edwin Biketi confessed that he regretted postponing a hospital visit. “The habit nearly cost me my life; now I know better that we all need medical care,” he said. Sylvia Mandila recounted losing a male friend to self-medication. “They treat what they don’t know. I had a friend who, for a long time, used Panadol for a persistent headache. We lost him due to a blood clot in the brain,” she said.
The study described these patterns through the concept of atomic sequences, the specific, step-by-step actions individuals take when navigating illness. For men, these sequences typically involve self-treatment first, then consulting a local pharmacy, with formal healthcare sought only when all else has failed, if at all. Fear of losing control or status compounds the delay.
Women face their own barriers: household responsibilities, lack of autonomy on health-seeking decisions, childcare burden and limited mobility. But the study found that the barriers facing men are structurally different and have received far less targeted attention from the health system.
Findings from across St Mary’s Lang’ata, Mbagathi Hospital, Rhodes Chest Clinic, Mama Lucy Hospital, Baraka Main and Riruta Health Centre identified work-related barriers as among the most significant for men. The hours of formal clinic operations conflict directly with the schedules of men in informal employment, many of whom must report to construction sites or markets before hospitals open.
Eunice Mikamu, a clinical nurse at Baraka Healthnet Clinic in Mathare, a Comprehensive Care Clinic for HIV/AIDS and TB, described how her facility responded. “Most male clients didn’t come for follow-up clinics even after diagnosis and start of treatment. They had to report to work early when hospitals were not yet open,” she explained.
Since most men prefer pharmacies for quick service, health information was given to pharmacists
The facility adjusted its TB clinic opening hours to between 6 am and 7 am, accommodating men in the jua kali and construction sectors. Community Health Promoters (CHPs) were also deployed to take drugs to the households of those on treatment. Patients now need to physically visit the hospital only once every two weeks to have vitals such as weight checked.
The facility also leveraged the tendency of men to seek care from pharmacies. “Since most men prefer to go to pharmacies for quick service, we’ve given health information to the pharmacists, who, after noticing TB symptoms, refer the suspicious cases for free X-ray scans in Mathare North and Lions Clinic. This has helped achieve timely diagnosis,” Mikamu stated.
Before these interventions, she noted, the facility was missing diagnoses and patients were wasting time treating pneumonia, delaying TB treatment. After the interventions, loss to follow-up cases fell from between 20 and 35 per cent to five per cent. Clients, feeling valued, began referring colleagues with symptoms such as prolonged coughs and weight loss to the clinic.
Dr Immaculate Kathure, Head of Tuberculosis, Leprosy and Lung Health at the Ministry of Health, turned the question back on the system. “Why are men not showing up in the hospital? Is it about stigma? Do we shout at men when they come to the hospital? Men also don’t like long queues in health facilities. The personality issue where a man as the head of the home can’t tell their wives they are sick is problematic,” she said.
Dr Kathure argued that women’s influence on men’s health-seeking behaviour was an underexplored lever. She drew a parallel with the early resistance to family planning, where male opposition constrained women’s uptake of contraceptives. “Some women were ready to use contraceptives but confessed their husbands’ threats of marrying other women who’ll continue giving birth limited their autonomy. We had to explain to the men the importance of spacing their children, and this helped turn around the situation,” she recalled. “The answer could be in looking for the women behind the men not going to the hospital, changing their attitude and making them supportive.”
Ministry of Health is now screening men in workplaces, homes, bars, and social spaces
Dr Evaline Kibuchi, Chief National Coordinator of Stop TB Partnership Kenya, warned that gender-blind programming was actively undermining progress. “Failure to address male transmission risks continued infection of women and children. Gender-responsive strategies can reduce TB incidence and mortality,” she said.
Prof Jeremiah Chakaya, CEO of ReSOK and an expert in TB control, argued that understanding individual and group behaviours of men in prisons, malls and markets would crack the riddle of why most men were affected and still got missed in care.
Stakeholders agreed on a simple truth captured by Dr Kathure: many patients are willing to seek treatment, but cannot afford basic costs like transport. These everyday barriers are often invisible in policy discussions, showing the need to ask better, more practical questions.
Kenya’s Ministry of Health is now taking services closer to men, offering screening in workplaces, homes, bars, and social spaces. Early results from Baraka Clinic show that when care meets men where they are, more of them get diagnosed and treated. The challenge now is whether these approaches can be expanded fast enough to prevent more deaths from diseases that are already treatable.