Professor Qureshi did not begin her medical journey expecting to lead one of the most impactful maternal health innovations of the decade; yet today, her research and advocacy are saving thousands of mothers’ lives in Kenya
Every six minutes, somewhere in the world, a mother dies from postpartum haemorrhage (PPH). In Kenya alone, between 4,000 and 5,000 women lose their lives each year to this preventable complication. These are mothers who never return home from the delivery room, leaving families shattered and children suddenly motherless.
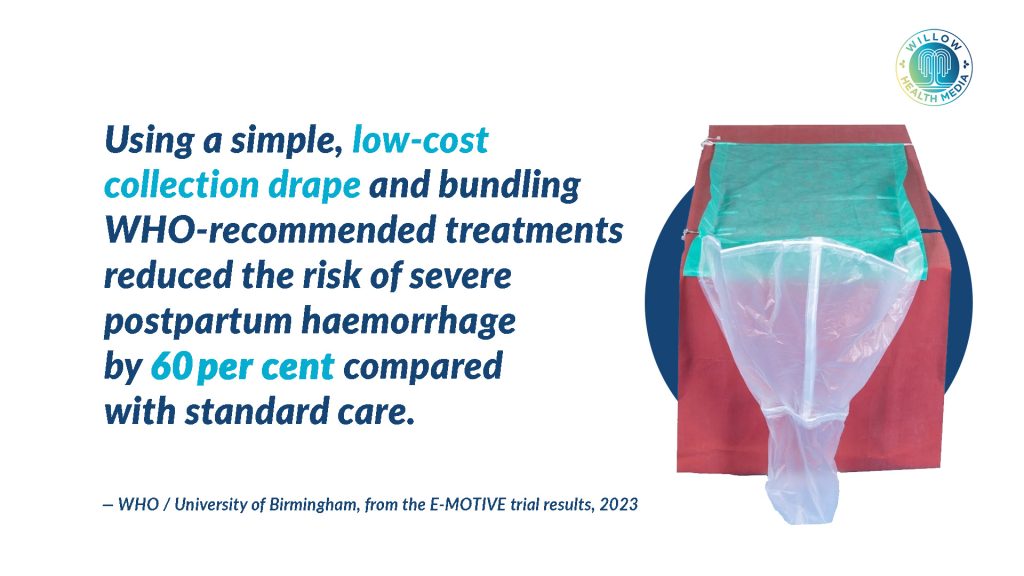
But across Kenya’s maternity wards, a quiet revolution has begun, driven not by high-tech equipment or expensive pharmaceuticals, but by a calibrated plastic drape which has reduced severe bleeding by 60 per cent in clinical trials and cut maternal deaths by a third.
At the centre of this transformation is a soft-spoken but formidable obstetrician-gynaecologist who has spent her life asking one painful question: “Why are so many mothers still dying from something we know how to prevent?”
For Professor Zahida Qureshi, Head of the Department of Obstetrics and Gynaecology at the University of Nairobi, the story of the PPH drape is intertwined with her own lifelong pursuit of safer childbirth for women in Kenya and beyond.
Professor Qureshi did not begin her medical journey expecting to lead one of the most impactful maternal health innovations of the decade. “I somehow had this inclination that I wanted to do medicine,” she recalls. Over time, she found herself drawn deeper into women’s health; first through clinical practice, then through teaching, and eventually, research.
When she joined the University of Nairobi as a faculty member, her work quickly intersected with global maternal health priorities. Collaborating with the World Health Organization (WHO), she contributed to international studies targeting the biggest killer of mothers worldwide: postpartum haemorrhage.
The breakthrough came when Professor Qureshi confronted the deceptively basic issue of estimation
Despite years of research and advocacy, the statistics refused to shift. Kenya’s maternal mortality ratio of 362 deaths per 100,000 live births remained stubbornly high.
PPH, defined as losing more than 500 millilitres of blood within 24 hours of birth, accounted for around 40 per cent of those deaths. Globally, it affected 14 million women every year and killed roughly 70,000 mostly in low- and middle-income countries.

Senior officials at the Ministry of Health pressed her to find out why, despite all the studies, nothing was changing.
It was a question that provoked Professor Qureshi to look not at what women were suffering from, but at how health workers were recognising and responding to postpartum haemorrhage. The problem, she realised, was hiding in plain sight.
The breakthrough came when Professor Qureshi confronted a deceptively basic issue: estimation.
“Visual estimation is incredibly inaccurate,” she explains. “One midwife might guess 200 millilitres (of blood), another might guess 400. In reality, it could be 700 or more.”
In packed maternity wards, where one midwife may oversee several labouring women at once, staff typically glanced at the blood on sheets or floors and made a quick judgment. The margin for error was enormous. Underestimation meant delayed response; delayed response meant women bled longer, deteriorated faster, and often died before lifesaving interventions began.

Another challenge was cultural. Reporting PPH was sometimes perceived as an admission of inadequate care. “Healthcare providers don’t want to say their patient has had postpartum haemorrhage,” she says. “So, you would always give a figure less than 500.”
The result was a dangerous cycle of silence and misjudgment. Recognition came too late, and treatment began too slowly. To break that cycle, something radically simple was needed: a way to measure blood loss objectively.

When blood reaches 300ml, staff are alerted; at 500ml, intervention is mandatory
Researchers had used calibrated drapes in previous studies, but it was the E-MOTIVE trial, conducted in Kenya, Nigeria, Tanzania, and South Africa, that wove two essential innovations together: early detection and rapid, bundled treatment.
At the moment of delivery, the drape is placed beneath the mother. Shaped like a V, the plastic funnels blood into a transparent pouch marked clearly at 300ml and 500ml. When the blood reaches 300ml, staff are alerted; at 500ml, intervention is mandatory.
“When blood reaches 300 millilitres, it triggers an alert,” Professor Qureshi says. “At 500, treatment must begin immediately.”

The second innovation, dubbed the treatment bundle, required healthcare teams to perform all critical interventions within 15 minutes: uterine massage, uterotonic drugs, tranexamic acid, IV fluids, and 15-minute vital assessments. It eliminated the old pattern of doing one thing, waiting, then trying another.
“Previously, we’d try one thing then wait five to ten minutes,” she says. “With the bundled approach, you do everything within 15 minutes.”
When the trial results arrived, even the researchers were stunned. They had hoped for a 25 per cent reduction in severe PPH. Instead, they achieved 60 per cent.
“We all jumped up and down,” Professor Qureshi laughs, still delighted by the memory. “We didn’t think it would be such a high figure.”
In Kenya, 19 facilities participated. Half used the new intervention; half continued with standard care. The results were certain: objective measurement plus rapid action saves lives.
Despite its simplicity, the drape initially faced resistance. Midwives feared it would slow down patient flow, as a bed occupied for too long delayed the next delivery. But Professor Qureshi persisted. She and her team of trained staff demonstrated the drape’s ease of use, and ensured each hospital had a dedicated research midwife for support.
If PPH is recognised and treatment begins within the first hour, survival is near 100 per cent
“Once they started using it, they liked it,” she says. Cleanliness and workflow improved; even cleaners appreciated the difference. By the end of the trial, midwives did not want to return the devices.
“They asked, ‘Where can we get more?’” she recalls. “They didn’t want to part with them.”
At the core of her advocacy is what she calls “the golden hour.” If PPH is recognised and treatment begins within the first hour, survival is near 100 per cent. But if detection and treatment are delayed beyond that, survival plummets to as low as 10-20 per cent.
“The drape ensures we recognise postpartum haemorrhage early and act immediately,” she says. “That is the game-changer.”
One surprise came from a Kenyan entrepreneur who overheard a conversation about the drape and saw an opportunity. After researching the device, he established a local factory to manufacture it in Kenya, a decision Professor Qureshi calls transformative.

During the trial, drapes had to be imported from India, incurring high shipping and duty costs. Local production drastically reduced prices and ensured reliable supply. The entrepreneur now produces three versions: a standard drape, a biodegradable option, and a hybrid with a reusable upper portion to reduce plastic waste.
Professor Qureshi chuckles, “He’ll become a millionaire; a billionaire, from these drapes.”

Nigeria has since followed suit with local manufacturing as Ethiopia, Tanzania, and South Africa are developing their own scale-up plans.
Research often takes years to translate into policy, but E-MOTIVE was different. Within months of the 2022 trial’s conclusion, the WHO convened a global PPH summit after which Kenya quickly developed a costed implementation plan.
National guidelines were updated, the drape and treatment bundle were integrated into emergency obstetric training; counties were directed to adopt them, and heat-stable carbetocin (a key drug requiring no refrigeration) was added to Kenya’s essential medicines list. Some counties like Makueni have already reported two years of zero preventable PPH deaths.
“The governor there has been a champion,” Professor Qureshi says proudly. “They bought drapes for the entire county.”
Her presentations at county forums and national conferences have sparked widespread support. The message from local leaders is now clear: every delivery in Kenya should use a calibrated drape.
Today, the WHO and the Gates Foundation have developed an international training package inspired by the E-MOTIVE model. Donors have funded free drapes for trial sites across four countries. Nations around Africa are preparing national rollouts.
For Professor Qureshi, the drape’s success is not just academic validation; it is a human victory born from listening to midwives, understanding the realities of overcrowded maternity wards, and refusing to accept preventable deaths as inevitable.
“Really interesting things happened because the results were so phenomenal,” she reflects. “But most importantly, this innovation came from understanding our context, and showing that simple, practical solutions can save the most lives.”
Graphics by Brian Wekesa.