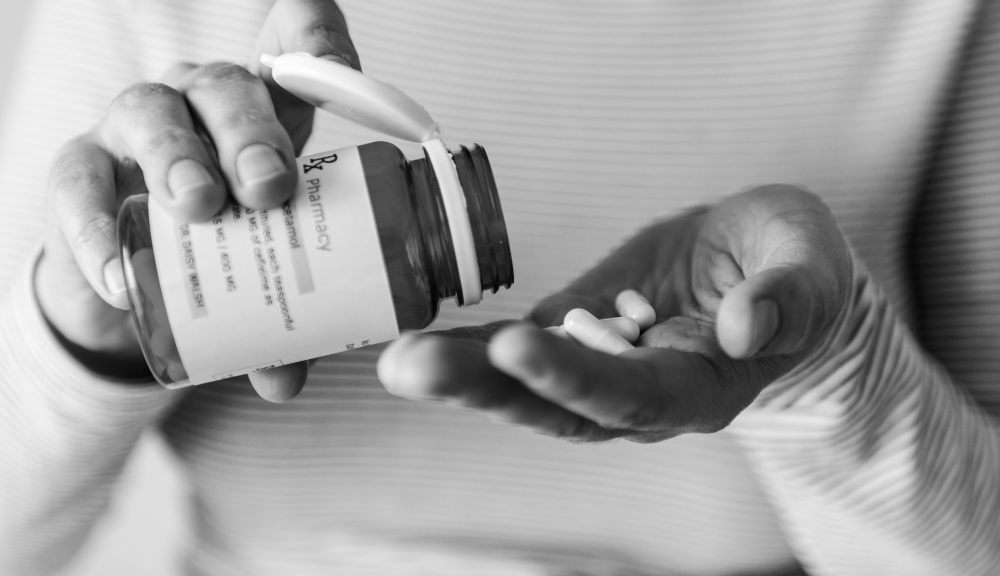
We could stock HIV medicines, draft policies, mobilise donor funding, but adherence rested on trust, and the quiet burdens people carry: secrecy, difficult disclosure, fear of discrimination.
I have debated policy in Nairobi boardrooms, audited county health budgets against performance, and drafted operational guidelines rooted in constitutional law. But the image that has stayed with me throughout my career is the first orphaned child who asked a question I could not answer in 2001.
I was then a student at Maseno University, studying communication and media technology as the country wrestled with HIV, poverty, inequality and hope.
I began volunteering with Compassion International, tutoring children to help them believe in a future beyond their circumstances. Instead, they transformed my understanding of health.
Many had lost one or both parents to HIV. Some lived with needy, ageing grandparents. Some rotated between relatives. Some had already internalised stigma and avoided certain conversations. Others were openly angry at God, at the world, at systems they couldn’t name.
They were children, but they carried adult grief.
The more I spent time with them, the more we talked about school, life, their fears. I introduced age-appropriate sexual and reproductive health conversations because misinformation was everywhere. I mentored them academically and emotionally. I watched bright minds dim under the weight of trauma and neglect. I saw how mental health was never spoken of, yet always present.
‘If my mother had gone to hospital earlier, would she still be alive?’
One afternoon, after a session, a boy lingered behind and then asked quietly: “If my mother had gone to the hospital earlier, would she still be alive?” The question froze me.
I did not then understand viral loads, CD4 counts, differentiated service delivery, or structural barriers. I did not know I would one day help design HIV interventions across counties. I did not know Kenya would adopt a constitution declaring health a right. I did not yet grasp that community systems stand between prevention and tragedy.
All I knew was that beneath the child’s question lay something deeper: Why did no one reach us in time?
That question has followed me for 25 years-into villages, informal settlements, peace dialogues in conflict zones, HIV technical groups, pandemic emergency centres, and health financing meetings.
It shaped my conviction that Universal Health Coverage (UHC) is not primarily about insurance cards or policy milestones, but whether prevention reaches households before loss does.
Human rights in constitutional text must travel to a remote homestead
And that journey between prevention and loss begins on a dusty village path, with a community health promoter reaching every household in time, linking them to care.
In 2010, Kenya enacted a new Constitution, a transformative moment. Article 43 declared health, including reproductive care, a right for all.
For those of us who had worked with orphaned children, survivors of violence, and young people living with HIV, this was more than legal reform. It was a moral affirmation.
It told the boy who asked about his mother: your loss was preventable. It told women in abusive relationships: your dignity matters. It told adolescents with silent questions: you deserve information and care.
Health was no longer charity. It was justice.
But rights written in constitutional text must travel a long distance before they become reality in a remote homestead.
Health workers waited months for pay, supplies ran out
Devolution followed, transferring primary healthcare to 47 counties. The idea was powerful: services closer to people, decisions made nearer to communities. In some counties, it worked beautifully. Community health units grew stronger. Data improved. Payments came more regularly. In others, budget shortfalls and political priorities slowed progress. Health workers waited months for pay. Supervision was unclear. Supplies ran out.
Over the years, as I moved from grassroots work to national programme leadership, supporting sexual and reproductive health and HIV systems, shaping behavioural interventions, and embedding community engagement into public health, I saw this unevenness clearly.
We had built legal architecture. But the human foundation remained fragile.
When I began working at a national scale in HIV prevention and systems strengthening, Kenya was confronting the epidemic with renewed intensity. We were talking about epidemic control, combination prevention, strategic information and viral suppression targets.
But in communities, the reality was more intimate.
I remember sitting in a support group for adolescents living with HIV at Live With Hope Centre in Nyagacho, Kericho. One young girl, barely sixteen, said, “The hardest part is not taking medicine. The hardest part is hiding it.”
Sister Placida, the Centre manager, looked at me in a despondent glare. That statement contained the essence of stigma.
They identify signs of depression, are first responders in cases of violence
We could procure antiretroviral drugs. We could design guidelines. We could secure donor funding. But adherence required trust, understanding the lived reality of secrecy, disclosure, fear of discrimination.
That someone was often a peer educator or mentor mother.
This experience, plus others, birthed an initiative we dubbed “Mwangalizi” (Carer), which paired an adult on HIV treatment with a child or adolescent struggling with medication for support. The “Mwangalizi” was essentially a volunteer community carer alongside other community cadres with different titles: peer educators, lay counsellors, mother mentors, and community health volunteers.
Regardless of name, their function is consistent. They are bridges. They visit homes. They follow up on missed appointments. They explain laboratory results in an accessible language. They mediate between healthcare providers and hesitant patients. They identify signs of depression. They are first responders in cases of violence.
I remember how a mentor mother in Kipsolu village in Belgut, Kericho, prevented a young pregnant woman from defaulting on treatment simply by visiting her daily for a week after disclosure triggered family rejection.
As a team leader within the HIV Free Generation Initiative, we empowered peer educators working with young men in informal settlements to create safe spaces for conversations about masculinity and risk, reducing vulnerability in ways no clinical guideline could achieve alone.
Female genital mutilation framed as cultural obligation rather than bodily harm
Yet these same cadres often operated without formal recognition. Some were supported through short-term donor grants. Some received stipends irregularly. Some had no structured supervision.
It was clear to me: epidemic control was being carried on the shoulders of people the system barely acknowledged.
Early in my career, through faith and community networks, I encountered the quiet epidemic of gender-based violence (GBV). In conflict-prone pastoralist regions, I facilitated dialogues where women described abuse as routine, girls resigned themselves to early marriage, and female genital mutilation was framed as a cultural obligation rather than bodily harm.
Violence was normalised. Silence was survival. From a public health perspective, GBV intersects nearly every indicator we measure: HIV transmission, maternal mortality, mental health burden, and child wellbeing.
I will never forget a young woman who repeatedly visited a clinic with vague headaches, fatigue, and abdominal pain. It took a community health worker’s gentle questioning about her home life to finally uncover severe domestic violence.
Providing post-violence care, psychosocial support, discreet follow-ups
The health system might have treated her symptoms indefinitely, but the community health worker addressed the cause. By providing post-violence care, psychosocial support, and discreet follow-up with local leaders, they moved from clinical treatment to operationalising dignity.
The Constitution guarantees equality and freedom from discrimination. But enforcement often begins not in courts but in conversations at the household level.
In cross-border peacebuilding near Uganda and Sudan, I learned that health access is about more than proximity. For years, the ToT Health Centre was avoided-a “monument of death”-after bandits killed women and children during an immunisation clinic. Though fully functional, it remained empty because it sat in conflict-prone territory, haunted by the memory of that attack.
Over the years, we also witnessed rumours about vaccination campaigns fuelled by communal or political mistrust, undermining immunisation coverage.
During outbreaks such as COVID-19, MPOX, and other emerging threats, these dynamics intensified. National guidance was disseminated quickly. Technical updates were clear. But compliance depended on trust.
Without them, misinformation would have spread faster than viruses
Community health workers became interpreters of intent. They reassured communities that vaccination was protective, not punitive. They explained quarantine measures without escalating fear. They carried feedback to policymakers, ensuring two-way communication.
Without them, misinformation would have spread faster than viruses.
Pandemics revealed a truth we often overlook: community health systems are a resilience infrastructure.
For decades, Kenya relied on community cadres without fully institutionalising them. Meagre budgets led to burnout, and talented peer educators bolted to more stable livelihoods.
But the passing of the Community Health Services Act 2022 marked a turning point. Community Health Promoters were formally recognised. Training and supervision were structured. Remuneration was mandated.
But recognition must be accompanied by predictable financing, continuous training, supportive supervision systems, and clear integration into primary healthcare financing frameworks. Without these, the promise remains aspirational.
A pregnant woman missing antenatal visits, presenting in obstructed labour
UHC, supported by evolving financing reforms, seeks to reduce catastrophic health expenditure and ensure access to essential services. UHC will fail financially if prevention is underfunded. I have seen the cost of delayed intervention:
A child with uncomplicated malaria progressing to severe disease requiring hospitalisation and transfusion.
A pregnant woman missing antenatal visits, presenting in obstructed labour, requiring emergency surgery.
An adolescent living with HIV is defaulting on treatment, developing opportunistic infections that overwhelm referral hospitals.
The dusty village path is where HIV stigma is challenged, GBV detected
In each case, the turning point was at the household level, where a trained and supported community health worker could have intervened sooner. Prevention is not only compassionate. It is fiscally prudent.
When community health workers are adequately financed through primary healthcare allocations, secondary and tertiary costs decrease.
Indeed, UHC is not measured solely by enrolment numbers or facility upgrades, but by whether any child has to ask why help came too late. The dusty village path is not metaphorical nostalgia. It is the frontline of constitutional fulfilment. It is where: HIV stigma is challenged. Gender-based violence is detected. Orphans are mentored. Adolescents receive truthful education. Conflict is mediated. Vaccines are accepted. Outbreaks are contained.
It is where Article 43 becomes lived experience. And until every household feels that promise, the work is not finished.
Obwiri Kenyatta is a global health expert in community-led health equity, climate justice, SRHR and HIV programmes.