Imagine your first days of motherhood clouded by haunting visions and whispers that aren’t there- this is the sudden and severe reality of postpartum psychosis, a rare but serious mental illness that strikes without warning within the first two weeks after childbirth.
After all the morning sickness, back pain, and other pregnancy-related complications, every mother hopes for a successful childbirth. Most assume life after birth will be neatly lined up for the coming physical and psychological changes.
For some, things go their way, but for others, the opposite is true as they struggle to care for their babies, refuse breastfeeding and avoid changing soiled nappies. Others shun bonding with their babies. This isn’t distant, but what befalls some mums like Moureen*, who was forced into motherhood through rape.
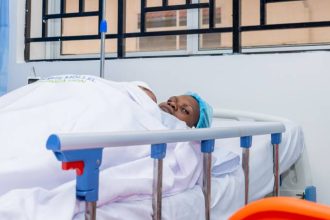
At only 16, Moureen gave birth to a baby boy, but her discharge was delayed due to strange behaviours which were mistaken for normal postpartum stress. She became noticeably cold, moved the bed by the window, leaving the baby alone on the other bed. She was fidgety, her eyes fixed on what was happening outside, as she made faces and frowned.
Moureen’s nonchalance was pronounced when her baby began crying. Instead of showing concern, she hastily swung out of the maternity ward towards the gate, where her maternity uniform betrayed her.
“Where to, young woman?” asked one of the security guards. Moureen returned a blank stare, then shouted angrily, “I hear voices in my mind calling me home…”
Postpartum psychosis is characterised by hallucinations, delusions and paranoia
The guards escorted her back to the ward. Medics later diagnosed Moureen with postpartum psychosis, hearing voices, and needing immediate mental health care.
Postpartum psychosis is a sudden mental illness after childbirth that affects a person’s ability to tell the difference between what is real and what is not.
It is characterised by hallucinations (seeing, hearing, or feeling things that aren’t real), as in Moureen’s case, delusions (beliefs that feel real but are actually false), and paranoia (extreme fear that others are against you).
It usually starts within the first hours to a fortnight after childbirth, as seen in Moureen’s case, whose symptoms started showing on day two. For some, onset may occur after six weeks post-delivery.
Without treatment, postpartum psychosis can spiral out of control, putting both mother and baby at serious risk.
Maternal blues and Postpartum depression differ from Postpartum psychosis
Maternal blues (baby blues): Are common, mild mood swings after childbirth that usually go away on their own within two weeks.
Postpartum depression is more severe, lasts longer and requires medical attention.
Postpartum psychosis is rare yet serious, involving hallucinations, delusions, and risk of harm to the mother or baby. It often coexists with postpartum depression, which can lead to mood swings.
Given the condition’s rarity, Kenya falls short of clear national data and research, a gap driven by a shortage of trained professionals, inadequate surveillance systems, limited mental health research funding, and persistent stigma that discourages reporting.
Early signs may be subtle and go unnoticed. They include mild confusion, withdrawal, insomnia, mood swings and restlessness.
Without treatment, symptoms can escalate into hallucinations and delusions that may threaten the safety of both mother and child. A mother who appears withdrawn thus needs constant care.
First-time mothers acclimatising to a newborn more vulnerable to postpartum psychosis
Some factors that could increase the risk of postpartum psychosis include:
First-time mothers: Given that everything is new, from recovery after birth to caring for a newborn, acclimatisation can be difficult, rendering them vulnerable to postpartum psychosis.
Mothers with a family history of mental health conditions: An interplay between genetics and learned coping mechanisms can increase stress sensitivity, putting them at higher risk.
Sleep-deprived mothers: A lack of rest can affect mood, focus, and emotional balance. Once sleeplessness becomes the norm, even small challenges can take a big toll, increasing their risk.
Prior postpartum psychosis: If you’ve had it before, your risk of another episode in a future pregnancy is much higher.
History of bipolar disorder: Having bipolar disorder increases the risk of postpartum psychosis. The risk is higher if mood-stabilising or antipsychotic medication is stopped during pregnancy. Therefore, treatment should be continued unless otherwise advised by your doctor.
Hormonal changes after birth: Sudden drops in pregnancy hormones and a quick rise in milk-producing hormones can upset the brain. This rapid shift sometimes triggers mood changes but rarely causes postpartum psychosis.
Pre-eclampsia and eclampsia: Severe high blood pressure and, in eclampsia, seizures can trigger postpartum psychosis. Headaches and fluid overload put extra stress on the brain, paving the way for postpartum psychosis.
Caesarean delivery: The pain, discomfort, limited mobility, and concerns about healing can add to the mental load, potentially triggering postpartum psychosis.
Postpartum infection/haemorrhage: Serious infections after childbirth or heavy bleeding can put the body under extreme stress. These strains, at times, trigger postpartum psychosis.
Admission to the newborn unit: The constant stress, broken sleep, and pressure of caring for a sick baby can strain a mother’s mind, making serious mood and mental health problems more likely.
Experiencing rape and lack of social support: The combination of past trauma and isolation can be overwhelming, increasing the risk of postpartum psychosis.
Thyroid disorders: The thyroid acts like the body’s internal balance system. If it goes out of balance after birth, it can put extra stress on the mind and, at times, cause postpartum psychosis, though this is rare.
Treatment for postpartum psychosis includes antipsychotics, mood stabilisers, or anticonvulsants. If you’ve had postpartum psychosis or other mental health issues, talk to your doctor before pregnancy. Counselling at antenatal clinics can also greatly improve outcomes.
Remember: you are not alone. Let loved ones know so they can watch for changes. Partners should stay informed and support each other. Early help and shared care protect the mother and baby. Kenya must also train more mental health professionals for early detection and follow-up cases of postpartum psychosis, which is worsened by the following:
Neglected maternal health policies and national health plans
Limited access to care leads to delayed help.
• Many women are unaware of the risk of postpartum psychosis.
• Weak screening programs miss warning signs.
Cultural stigma and beliefs
• Some communities label postpartum psychosis as witchcraft, discouraging mothers from seeking medical care.
• Fear of shame and blame forces women to suffer in silence, worsening the condition.
Inadequate number of trained psychiatrists
• As of September 2025, there were only 150 psychiatrists in Kenya.
• Many healthcare workers lack training to detect problems early. Continuous Medical Education may help.
Few psychiatric nurses
• Other nurses can screen for mental health issues, but heavy workloads delay detection of postpartum psychosis.
• Delayed detection leads to delayed care.
Limited supply of medications
Antipsychotics, mood stabilisers and anticonvulsants are often unavailable at county and sub-county hospitals.
• Drug stock-outs force patients to pay out of pocket.
• Irregular medication use increases the risk of relapse.
Family and social support gaps
• Stigma makes many mothers reluctant to seek help.
• Lack of family support leaves mothers isolated and unsure where to turn.
Geographic distance from hospitals
• Long distances make it difficult to access check-ups or mental health services.
• In emergencies, reaching a hospital is nearly impossible, allowing the condition to worsen.
Low economic status
• Poverty limits the ability to afford transport, consultations or medication, delaying or preventing care.
• Financial stress adds emotional strain, further worsening the condition.
Moureen’s experience was not a curse or nightmare-it is a real medical condition exposing major gaps in Kenya’s health system. Mothers remain untreated due to trained staff shortages, weak screening, drug stockouts, stigma and poor support. We need universal healthcare for women, more mental health workers, stronger family support, and public campaigns to fight stigma. Fixing this will improve maternal and child health—and benefit all of Kenya.
Dr Rachel Kerubo is the Resident Medical Officer – Department of Internal Medicine, Nyamira County Referral Hospital.