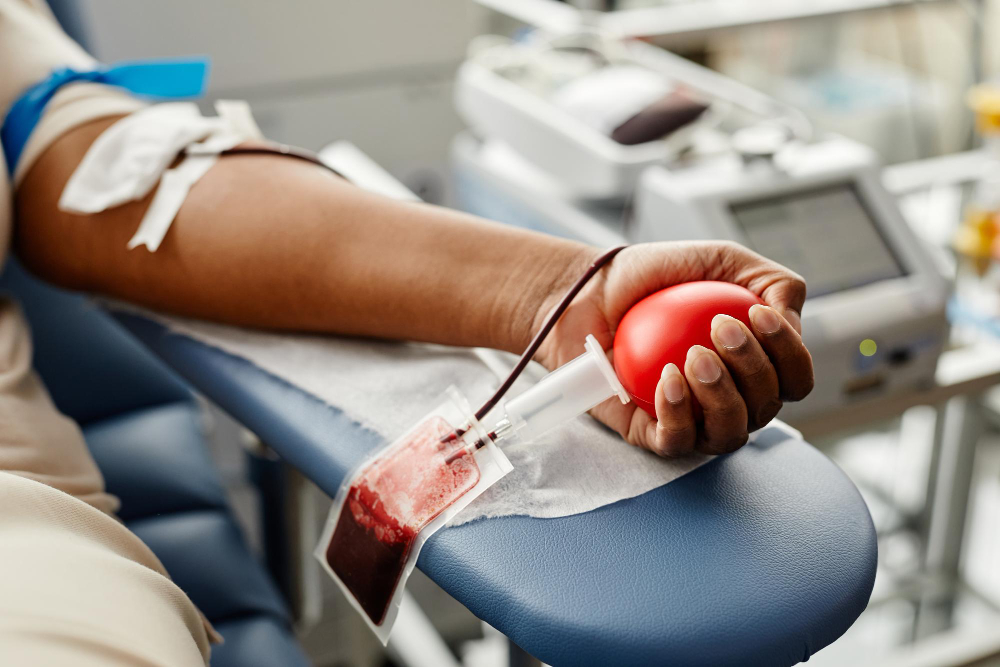
Most blood-related deaths in Africa are not caused by complex medical conditions, but by systemic failures affecting supply and demand.
Africa must stop treating blood as a hospital consumable and begin recognising it as essential national infrastructure to enhance the survival of the continent’s population, experts have said.
Speaking at a webinar held late last year (2025) titled From Dependency to Sustainability: Financing Africa’s Blood Future, organised by the Coalition of Blood for Africa (COBA), experts lamented that in Africa, conversations about blood donation tend to surface only during emergencies.
Blood, they said, is mentioned when it is urgently needed, often amid frantic searches by families and hospitals scrambling to save lives. Outside crisis moments, however, blood systems rarely receive sustained attention or investment.
The discussion shifted the focus from emergency response to a broader and more urgent reality, that blood is a critical infrastructure for the health and survival of Africa’s population. The experts said that most blood-related deaths on the continent are not caused by complex medical conditions, but by systemic failures.
Africa’s population of over 1.5 billion people requires an estimated 15 to 20 million units of blood annually to meet World Health Organisation (WHO) standards, which recommend that at least 1 per cent of the population donate blood each year. However, most African countries fall far below this threshold.
According to Joseph Wangendo, Senior Technical Officer at Africa CDC, current supply levels are well below WHO targets. “We cannot talk about sustainability when we have not addressed the issues of supply and demand,” he said.
Donor-funded blood programmes do not offer long-term solutions; when funding ended, services collapsed
In many regions, donation rates remain at just 5-7 per 1,000 people, compared to the recommended 10-30 per 1,000.
“Africa’s challenges are shared,” Wangendo noted. “Which means the solutions can be shared too.” He called for pooled procurement and harmonised policies across the African Union to reduce the continent’s heavy reliance on external donor funding.
Wangendo warned that donor-funded blood programmes do not offer long-term solutions. Under initiatives such as the President’s Emergency Plan for AIDS Relief (PEPFAR), some national blood services were almost entirely financed by external partners, with minimal government contribution. However, when funding ended, services collapsed.
“Healthy people do not want to go to hospitals,” Wangendo said, recalling the Covid-19 pandemic, when blood donations dropped sharply almost overnight.
His experience in Kenya demonstrated that access drives supply. Mobile blood buses stationed in high-traffic areas of Nairobi became the highest-performing donation centres because donation was made convenient and visible to the public.
Yet the crisis persists. Kenya needs at least 500,000 units of blood annually, but collects only 200,000 to 250,000 units, according to the Kenya Tissue and Transplant Authority (KTTA), leaving a shortfall of about 200,000 units every year.
A similar crisis exists in Nigeria. Prof Saleh Yuguda, the Director General of Nigeria’s National Blood Service Agency (NBSA), said the country faces a severe shortage. “In Nigeria specifically, we face about 75 per cent shortage of blood,” he said.
Based on WHO recommendations, Nigeria, with a population of over 200 million, requires more than two million units of blood annually to meet demand.
The consequences are deadly. Prof Yuguda said 27 per cent of maternal deaths in Nigeria are caused by postpartum haemorrhage, while 40 per cent of road traffic deaths result from excessive bleeding and the inability to access blood transfusions in time.
In response, Nigeria enacted the National Blood Service Commission Act in 2021, leading to the establishment of the National Blood Service Commission as the central authority responsible for coordinating and regulating blood transfusion services nationwide.
Prof Yuguda emphasised the need to integrate blood services into national health insurance schemes. Currently, in many African countries, blood transfusion is not covered under public health insurance, leaving patients to pay out of pocket.
“We can encourage the wider coverage of the existing health insurance system in our countries and make sure that we incorporate blood transfusion into the existing system,” he said, noting that this would significantly reduce out-of-pocket costs for patients.
He also stressed the importance of public-private partnerships, arguing that governments alone cannot fund the entire blood ecosystem, including the procurement of screening kits and other essential supplies.
Hundreds of thousands of litres of plasma are discarded every year due to the lack of extraction infrastructure
While global standards prioritise voluntary, non-remunerated blood donation, Prof Yuguda argued that in contexts where patients die while waiting for blood, safety and access must take precedence over ideology. Blood systems, he said, require strong political will and enabling legal frameworks to ensure domestic ownership and continuity.
David McIntosh, Chair of United Plasma Action, described plasma as “liquid gold”, yet noted that across Africa, hundreds of thousands of litres are discarded every year due to the lack of plasma fractionation infrastructure, the industrial setup used to turn donated human plasma into life-saving medicines.
Currently, most plasma collected in Africa is wasted. McIntosh challenged the assumption that there is no market for plasma-derived medicinal products (PDMPs) on the continent, arguing instead that demand is suppressed by high prices and the absence of local manufacturing. Processing plasma locally, he said, could turn waste into a sustainable source of revenue.
“In the US or some of the countries in Europe that are well served, you would have 75 per cent of plasma medicines made from source plasma from apheresis,” he noted. This means plasma that is collected directly from a donor using a special process called apheresis, rather than being separated from whole blood after a regular blood donation.
The plasma is often collected at plasma donation centres, and donors can give more frequently than whole blood donors. The collected plasma is then used to manufacture plasma-derived medicines such as immunoglobulins, clotting factors for haemophilia, and albumin.
Despite the challenges, pockets of sustainability are emerging. Maishibe Ntihane, CEO of South Africa’s National Bioproducts Institute (NBI), pointed to South Africa and Namibia as examples of functional blood systems.
These countries operate cost-recovery models in which hospitals pay for blood products, and the revenue is reinvested into equipment, quality systems, and compliance with Good Manufacturing Practice standards. The result is a self-sustaining supply chain.
“Blood services are the cornerstone of healthcare,” Ntihane said. “If they collapse, the system collapses.”
John Paul Omollo of Roche Africa added that while blood systems must remain publicly led and transparent, scaling them effectively will require private-sector expertise in diagnostics, cold-chain logistics, and data systems.