The fate of 6,500 orphaned and vulnerable children from 3,000 households in Bungoma County is now walking a financial tightrope — no safety net in sight — after Ksh30 million annual funding vanished after the closure of USAID.
It is a hot, sunny day, and the blue sky is dotted with fluffy white clouds as we saunter to the home of Patrick Osakho in East Bukusu village, Kanduyi constituency, Bungoma County.
His small, modest home is a silent witness to the unyielding struggle of a father caught between love, responsibility, and despair. Despite the bright sunshine glaring outside, a dark cloud hovers over his life. The sound of children’s laughter at Osakho’s home fades away. It is replaced by a growing silence, one that speaks of fear, of lives hanging by a thread.

Osakho is a caregiver raising two children, both living with HIV. The two boys are sons of his late brother, who died of HIV-related complications along with his wife over five years ago.
After their parents’ deaths, the children were enrolled by Community Research in Environment and Development Initiatives (CREADIS), a local non-governmental organisation running 4TheChild program that supported people living with HIV, Orphans and Vulnerable Children.
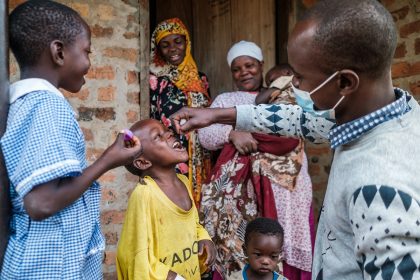
4TheChild was sponsored by the United States Agency for International Development (USAID) and supported over 6,500 children in Bungoma alone. Children enrolled in the program received school fees, meals, and Antiretroviral Therapy (ART) drugs that kept their fragile health intact.
But all that came to a sudden halt with the recent official termination of all foreign assistance under the United States Agency for International Development (USAID), sending shockwaves across the globe.
Hope should be the last thing to lose, but it’s hard to see where hope is hiding
“The antiretroviral drugs aren’t adequate when the children have no food to eat. They need proper nutrition to stay strong, but how can I give them that when there is nothing left?” Osakho tells Willow Health. “I have always believed hope should be the last thing to lose, but now, it’s hard to see where hope is hiding.”
“Please,” Osakho whispers amidst despair. “Someone, anyone, help us… I don’t know how much longer they can hold on.”
CREADIS received Ksh30 million annually from USAID’s 4TheChild Program to support 6,500 children from 3,000 households in Bungoma. Some 18 CREADIS staff members on the program have since been laid off, like Wanjala Senorina, the case manager and documentation officer at CREADIS, who focused on four key domains: health, safety, stability, and education.
“We enrolled children and their caregivers into the program to ensure they had access to essential resources for survival,” offers Senorina. Under the health docket, children received nutrition, viral suppression, medical adherence and regular follow-ups with caregivers. “We also monitored school attendance, ensuring all children were in school.”
To support and empower caregivers economically, CREADIS introduced small grants, merry-go-rounds, loans and savings at low interest rates for small businesses.
“Many beneficiaries are calling, crying for help, begging for any support not knowing I’m also jobless,” says Senorina. “There is an urgent call for other donors to step in and help. These families need support more than ever, and we can’t abandon them now.”
By exposing us, they want us to die… People were scared to go pick their ARVs
Merab Oguna, 52, has been living positively with HIV for 24 years. She is the director of TB Support Group, a community-based organisation (CBO) in Kisumu that ensures that clients on TB and HIV treatment adhere to their treatments. The CBO has 25 members, but their advocacy program benefits over 200 people.

“We have a special section for People Living with HIV in the health facilities. We have a Comprehensive HIV Care Clinic, designed to provide a wide range of services, including provision of antiretroviral drugs, counselling, CD4 testing, and other healthcare services tailored to the needs of people living with HIV,” explains Oguna, adding that after USAID funding cuts, the impact was immediate.
The abrupt dismissal of USAID staffers saw HIV clients facing stigma. No one was willing to serve them. Most were referred to public hospitals’ outpatient units.
“People were scared to go to the facilities to pick their ARVs and such panic is not good for their wellbeing,” Oguna told Willow Health, adding that HIV clients are facing depression. “We are on a lifelong treatment,” she says. “Majority of those affected give up when they ponder the idea of going to an outpatient unit to collect their medication.”
You go to a public hospital pharmacy to pick ART drugs with a neighbour picking malaria tablets
The government is integrating services to cut costs following the termination of USAID health projects, which, according to Oguna is not a good idea as those whose HIV status were private now
“Imagine someone who had kept their (HIV) status private now have to ‘go to a public hospital pharmacy to pick their ART drugs with a neighbour picking malaria drugs. By exposing us, they want us to die.”
“We risk eroding the milestones the country had made in the fight against HIV,” she predicts. “We will experience many deaths, a spike in new infections and stockouts of commodities if the matter is not addressed with the urgency it deserves.”
Kisumu County has the second highest prevalence of HIV in Kenya at 14.5 per cent against the national prevalence of 4.9 per cent. The National Syndemic Diseases Control Council (NSDCC) estimates that there are more than 116,000 people living with HIV in the county who are under treatment and management of HIV.
The fate of people living with HIV in Kenya is now uncertain. They previously had free access to antiretrovirals through the President’s Emergency Plan for AIDS Relief (PEPFAR) and the Mother-to-Child Transmission of HIV Control (MTCT) programs.
Kenya has enough antiretroviral drugs and HIV testing kits to last two years
Health Cabinet Secretary Dr Deborah Barasa, while speaking at the Mission for Essential Drugs and Supplies (MEDS) headquarters earlier this month, exuded confidence that Kenya has enough antiretroviral drugs and HIV testing kits to last two years.
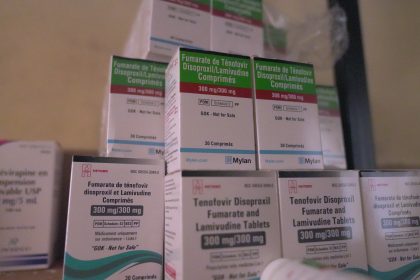
Barasa was flagging off a consignment of HIV related medical supplies from the MEDS warehouse, where she said the commodities included 2.5 million bottles of ARVS, 750,000 HIV test kits and half a million malaria drugs.
“Kenya currently has over two million packs of TLD (Tenofovir, Lamivudine, and Dolutegravir), the main antiretroviral therapy regimen for HIV treatment. This stock is estimated to cover approximately 4.7 months of demand,” Barasa said, adding that another consignment of 4.8 million packs is expected by June this year, which would extend the stock to about 11 months.
She intimated that there are over 360,000 packs of Abacavir/Lamivudine (120/60mg) for paediatric treatment,t which can last for 7.4 months and “the government is committed to introducing a fixed dose paediatric combination from August this year that will last for 18 months.”