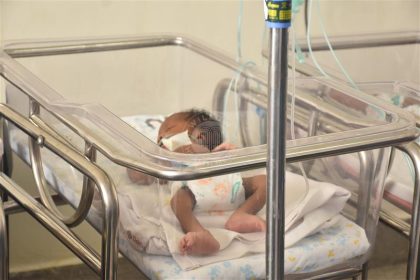
Each year, 134,000 babies are born prematurely in Kenya, which has no national data on Group B Streptococcus (GBS), how many pregnant women carry it, how many newborns it kills, or how many preterm births it may be causing.
A common bacterium that lives harmlessly in the bodies of healthy women is quietly driving thousands of preterm births, stillbirths and maternal infections across Kenya – and in most cases, it is never detected.
Group B Streptococcus (GBS), long recognised as a cause of newborn sepsis and meningitis, is now understood to play a far larger role in maternal and perinatal health than current data reflect. Scientists presenting at the International Symposium on Streptococcus agalactiae Disease (ISSAD) in Nairobi say the true burden of GBS in low- and middle-income countries is certainly being undercounted, and Kenya is a stark example.

“We often underestimate infection as a cause of maternal death,” said Prof Anna Seale, Principal Officer for maternal immunisation, product development and surveillance at the Gates Foundation. “Globally, over a quarter of a million women die each year from maternal causes. Around 11 per cent are due to infection, and GBS is part of that picture, but it is largely invisible in routine data.”
GBS commonly colonises the vagina and rectum of healthy women without causing any symptoms. During pregnancy and childbirth, however, it can ascend into the uterus or be passed to the baby, triggering maternal sepsis, endometritis, chorioamnionitis, urinary tract infections, stillbirth, preterm birth, and newborn sepsis and meningitis.
Globally, a GBS fact sheet estimates that 518,100 preterm births annually are linked to GBS infection. In Africa, the burden of neonatal disease is estimated at 1.12 cases per 1,000 live births. Scientists also estimate that a future maternal GBS vaccine could potentially avert 127,000 early-onset GBS cases, 87,300 late-onset cases, 31,100 deaths, and 185,000 preterm births and “These figures hint at both the scale of disease and the opportunity for prevention,” Prof Seale noted.
A significant number die from complications of prematurity, others face lifelong disability
About 134,000 babies are born prematurely in Kenya every year, according to the Ministry of Health’s 2024 World Prematurity Day fact sheet. A significant number die from complications of prematurity, while others face lifelong disability.
Yet despite this burden, Kenya lacks up-to-date national data on GBS colonisation in pregnant women, reliable figures on GBS-related neonatal disease, estimates of GBS-associated stillbirths, and evidence on how many preterm births are driven by GBS.
Dr Simon Kigondu, a gynaecologist and President of the Kenya Medical Association (KMA), said the conference had highlighted how overlooked the bacterium is in routine care, especially its importance in both maternal and perinatal health.
Kenya, he said, has long focused on the ‘big killers’ like bleeding, infection and ruptured uterus for mothers and asphyxia and preterm delivery for babies, yet “Some of the maternal and perinatal morbidity and mortality may actually be attributed to it (Group B Streptococcus).”
Many unexplained poor outcomes, Dr Kigondu added, could be linked to GBS like “Intrauterine growth restriction, preterm delivery and neonatal infections, and many times we have not thought of Group B Streptococcus. But now awareness has increased, especially because of this conference.”
Unlike Western countries, where routine screening are standard, most African women are never tested for GBS
A scoping review commissioned by Kenyan health bodies including Kenya Obstetrics and Gynaecology Society, the Kenya Paediatric Association and Lignum Vitae Health, found GBS evidence to be highly uneven.
Maternal colonisation ranged from 1.8 per cent to 64 per cent, with transmission to babies reaching 63.3 per cent. Infants of colonised mothers faced up to 20 times higher infection risk. Higher colonisation rates were linked to younger mothers, preterm pregnancies, and HIV- though co-trimoxazole offered protection for HIV-positive women.
Unlike in high-income countries, where routine screening at 35 to 37 weeks and antibiotics during labour are standard, most African women are never tested for GBS.
“GBS is not very well tested in Kenya,” Dr Kigondu said. “We don’t routinely test for it. Usually, a woman presents with a condition and then we do tests. I have not seen much routine GBS testing in my practice.”
Global attention has focused on infants, but ISSAD delegates stressed that maternal disease has been equally overlooked. Autopsy studies comparing clinical diagnoses with laboratory findings reveal major gaps.
“There is a huge discrepancy between what clinicians think causes maternal death and what laboratory evidence shows,” Prof Seale said. “We are not ascertaining maternal GBS disease.”
When GBS ascends from the vagina into the uterus, it causes inflammation, triggering early labour
Systematic reviews suggest there are at least 40,000 cases of invasive maternal GBS disease globally each year, a figure considered a severe underestimate, particularly in countries without blood culture facilities.
The danger extends to the foetus too. In Ethiopia, a study found that when mothers had GBS bacteria in their blood, every case ended in stillbirth and “These are tragic losses that never make it into national statistics,” Prof Seale said.
Scientists increasingly believe that when GBS ascends from the vagina into the uterus, it causes inflammation of the foetal membranes, triggering early labour. Animal studies show that even without live bacteria, GBS membrane vesicles can weaken the tissues separating mother and foetus. In one major placental analysis, GBS was the only organism found in placental tissue that could not be explained by laboratory contamination, suggesting true infection.
Human studies show women colonised with GBS have about 1.2 to 1.4 times higher odds of preterm birth – likely an underestimate.
“Gestational age dating is imprecise, and GBS testing is not always done at the right time,” Seale said. “That creates noise and hides the true association.”
Social health insurance could make screening for Group B Streptococcus more accessible
Dr Kigondu said routine testing would require major policy shifts, especially in testing for GBS “But financing is an issue,” he said. “The test for Group B Streptococcus may be out of reach for many people, especially in the public sector, where even routine tests are already a challenge.”
He suggested that social health insurance could make screening more accessible.
“This test could be included in insurance reimbursement, which would make it more accessible,” he said. “Laboratories would also need to increase their capacity so we can collect local data, because right now we do not have widespread data on the prevalence and effects of GBS on our mothers and newborns.”

One of the most anticipated developments is a maternal GBS vaccine now in late-stage trials. Keith Klugman, Director of the Pneumonia Programme at the Gates Foundation, said the vaccine could transform understanding of the disease.
“We hope to introduce the vaccine in Africa within three years,” he said. “For the first time, the vaccine itself will act as a probe, showing us what fraction of stillbirths, prematurity and neonatal sepsis are really due to GBS.”
Marty Perhach, Chief Executive of Group B Strep International, highlighted the human cost, considering “Many surviving children will have lifelong neurodevelopmental challenges. That is a lifetime of heartache for families.”
Most women in Kenya give birth without ever being tested for Group B Streptococcus
Portugal offers a glimpse as it has since introducing routine screening and antibiotics during labour, with the country recording a 40 per cent reduction in disease incidence and lower fatality rates.
Elizabeth Martins of Lisbon’s Faculty of Medicine explained that Portugal moved from voluntary guidelines to national policy in 2011 as “An official norm issued by the public health authorities which established, similarly as to what was being done in the United States, the screening of pregnant women at 35 to 37 weeks gestation and the recommendation of intrapartum antimicrobial prophylaxis for pregnant women care.”
The contrast with Africa is stark: most women in Kenya and neighbouring countries still give birth without ever being tested for GBS.
Experts at ISSAD argued that Kenya must rethink how it measures maternal and newborn infections. Proposals include integrating GBS surveillance into electronic medical records, expanding blood culture testing, linking maternal and newborn outcomes, creating sentinel genomic sites, and strengthening laboratories.
Imagine preventing not just newborn sepsis, but also preterm births and maternal deaths
“We need to design this as a national system, not just research projects,” Prof Seale said. “Pregnancy does not end with delivery. The postpartum period is a high-risk time for infection.”
GBS is neither rare nor benign. It contributes to maternal sepsis, stillbirth, and prematurity – three of the most devastating outcomes of pregnancy. Yet because most cases go undiagnosed, the infection remains largely invisible in national statistics.
As Kenya grapples with high rates of preterm birth and maternal mortality, ISSAD’s message was clear: GBS can no longer be ignored.
“Imagine preventing not just newborn sepsis,” Prof Seale said, “but also preterm births and maternal deaths. That would be a profound change for families and health systems alike.”