From a world-first facial reconstruction to snakebite antivenom, Dr Mercy Korir argues that what gets reported shapes what gets fixed.
In Kenya, a wrong health decision can begin with something as simple as bad information, a misleading social media post, a delayed diagnosis, or a patient choosing a quack over a qualified doctor because they simply did not know where else to turn.
For Dr Mercy Korir, CEO and Editor-in-Chief of Willow Health Media, this is where journalism becomes more than storytelling. It becomes a matter of life and death.

“The right kind of health information is literally the difference between you going to the right place or going to some quacks,” said Dr Korir during an interview on The People’s Breakfast on Radio Generation Kenya. “If you give the wrong information, people will use that information and do the wrong thing or not seek healthcare at all.”
This belief pushed her from medicine and mainstream journalism into building one of Kenya’s digital newsrooms dedicated to health and science reporting. But beyond reporting, she sees health communication as a critical pillar of Africa’s future, one tied to innovation, research, political leadership, and health sovereignty.
“We are a digital newsroom,” she explains. “Only that our focus is on health and science journalism. We produce and publish both video and text content on our website and all our social media platforms.”
A story that changed lives: They removed that whole tumour and replaced her jaw with full implants
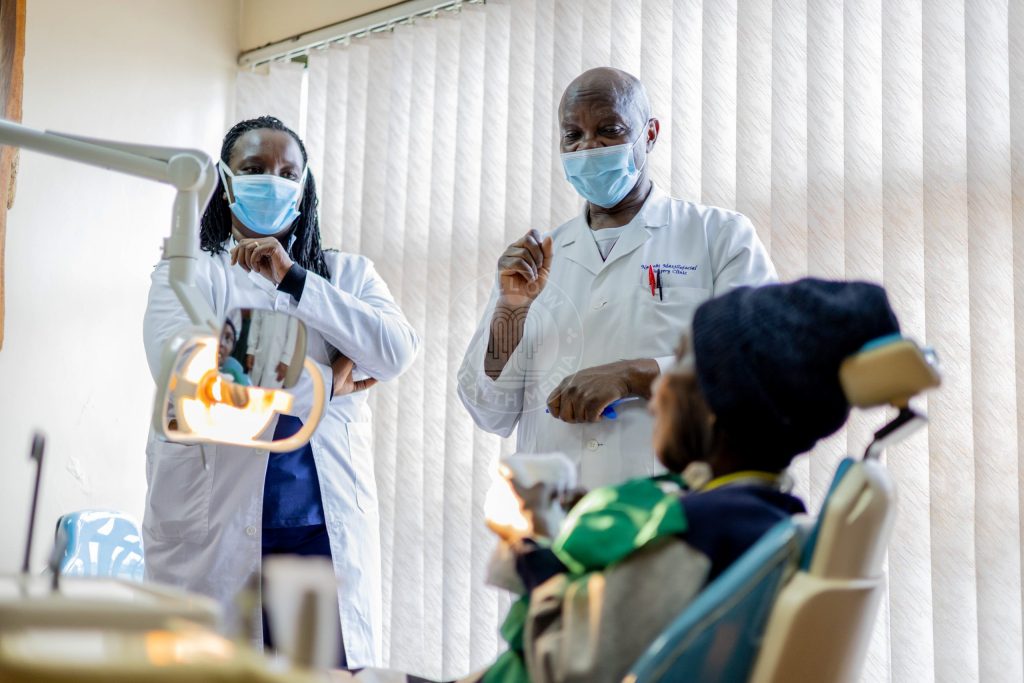
One of Willow’s most powerful recent stories followed a young woman in her mid-20s whose life had been overtaken by a massive facial tumour that severely disfigured her face and robbed her of confidence, mobility, and normal life. Doctors first told Dr Korir about the case in 2023, and when Willow Health launched fully in 2024, her team began documenting the young woman’s journey.
“She had a facial reconstruction,” Dr Korir says. “You can imagine half of her face. They removed that whole tumor and replaced her jaw with full implants in a surgery that lasted 18 hours. Now she has a new face. She has a new life.”
For Dr Korir, the story was bigger than one patient. “This is a world’s first facial reconstruction surgery done here in Kenya by Kenyan doctors, Kenyan engineers, Kenyan everything,” she says. “It gives confidence in the healthcare we have and the expertise we have.”
For decades, many Kenyans believed such procedures could only happen abroad, particularly in India, the UK, or the United States. She said it was happening here in Kenya, and that people did not need to travel, spend a lot of money, or sell all their property to access such care. After the story aired, families with similar conditions began reaching out, asking how they could contact the doctors. That, she says, is the real power of journalism.
In an age flooded with misinformation, disinformation, and misleading online content, Dr Korir believes health communication has itself become a determinant of health. “Right now, in this digital age, health communication is actually a determinant of health,” she says. “There is too much information, misinformation, disinformation, everyone can be an expert in anything.”
Donor dependence in HIV treatment, health data systems and critical healthcare financing
It is why Willow also runs a strong training component for journalists and public health communicators, from interns all the way to working journalists. Through partnerships with institutions like KEMRI Graduate School, the platform trains health reporters in ethical reporting, public health communication, child protection, consent, confidentiality, and responsible storytelling. “You have to understand that people have rights. When you are covering children, vulnerable communities, sexual and gender-based violence, there are special considerations. At the end of the day, it is not just the story,” she said.
Beyond journalism, Dr Korir is deeply concerned about Africa’s health sovereignty, the ability of countries to fund, research, and solve their own medical problems. In her view, Kenya is still far from achieving it.
“We are not there,” she says, pointing to donor dependence in HIV treatment, health data systems, and critical healthcare financing. “As long as somebody else is financing critical sections of your healthcare, then you don’t have sovereignty.” She recalls how aid freezes under the Trump administration exposed dangerous vulnerabilities, noting that HIV programmes, antiretrovirals, and health data systems should depend on nothing other than a country’s own taxes and funding.
Even something as basic as snakebite treatment reveals the problem. In counties like Baringo, West Pokot, and Ukambani, snake bites remain a major health threat, yet Kenya still relies heavily on antivenom developed in India. “The snakes in India are not the same snakes we have here,” she says. “Thankfully, they kind of work, but increasingly we need solutions that work for our own population.” The Kenya Snakebite Research and Intervention Centre is working toward developing local antivenom, but progress is slowed by poor research funding. Kenya’s investment in research was supposed to reach 2 per cent of GDP, but currently stands at around 0.7 per cent.
Dr Korir notes that Kenya carries a double burden of disease, with infectious diseases and non-communicable diseases accounting for almost equal proportions, a reality that requires the government to invest in both directions simultaneously.
AI is most effective in diagnostics, identifying TB, pneumonia, lung conditions, but doctors must apply clinical judgment
Technology offers hope. From artificial intelligence in diagnostics to telemedicine and robotic surgery, Kenya is beginning to embrace digital health solutions. But Dr Korir is quick to warn against blind trust. “AI does not replace human intervention,” she says. “Even ChatGPT can hallucinate.” She believes AI is most effective in diagnostics, particularly radiology, where it can help identify TB, pneumonia, Covid-19, and rare lung conditions. Doctors, she insists, must always apply clinical judgment.
She is also, perhaps surprisingly, an advocate for traditional medicine, though with caution. “Modern medicine is derived from plants. It is just sophisticated herbs.” She believes Kenya risks losing generational herbal knowledge if it is not documented and scientifically researched before the elders who hold it pass on. Institutions like KEMRI already have dedicated centres for traditional medicine research, she notes, but progress needs to go further.
Ultimately, Dr Korir insists that many of Kenya’s health failures are not medical problems. There are leadership problems. On maternal deaths, she is blunt. “Any mother dying from preventable causes is a political leadership problem. Health is devolved. Counties control hospitals, staffing, blood supplies, emergency care, and newborn intensive care units. If you have not made an intentional decision to have blood in your hospital, the right medicines, and the right people, if this mother dies, who do we blame? It is the governor.”
As Nairobi hosts the 2026 World Health Summit Regional Meeting for the first time in Africa, Dr Korir believes the continent stands at a defining moment. “We are the next frontier for everything,” she says. But Africa’s health future, she insists, will not be built by chance. It will be built by deliberate investment, truthful journalism, political will, and people having the right information at the right time, because sometimes, saving a life begins long before a patient reaches the hospital.