Kenya Eyes WHO Certification for Elimination of Sleeping Sickness whose symptoms include fever, headaches, joint pain, confusion and sleep disturbances
Guinea has officially eliminated Human African Trypanosomiasis (HAT) as a public health threat—a landmark achievement in the global fight against Neglected Tropical Diseases (NTDs). Now, Kenya is poised to follow suit, seeking the same recognition from the World Health Organization (WHO) after reporting no local cases since 2009.
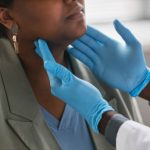
The last recorded cases in Kenya were among German and Belgian nationals who had travelled through Tanzania before testing positive upon returning to their home countries. HAT, commonly known as sleeping sickness, is a parasitic disease transmitted by infected tsetse flies. It begins with flu-like symptoms such as fever, headaches, and joint pain but progresses to severe neurological complications, including confusion, sleep disturbances, and behavioural changes, in its advanced stages.
While HAT is typically considered an adult disease due to children’s limited exposure to tsetse fly habitats, a rare paediatric case was documented in Busia County in October 1999. The African Journal reported the case of a two-year, eight-month-old boy from On’gariama sub-location in Teso District. He was admitted to the National Sleeping Sickness Referral Hospital in Alupe after suffering from persistent fever, respiratory distress, hepatosplenomegaly, and neurological symptoms for five months.
Initially misdiagnosed as pneumonia, the child’s condition worsened despite repeated treatments for malaria and typhoid. A veterinarian reviewing his X-rays noticed the late stage of the disease. Treatment led to temporary recovery, but the child relapsed three months later, leaving him with long-term complications, including speech and body movement disorders besides psychological trauma.
The average age of Sleeping Sickness patients was 32 years, with the majority under 40 years
A 2011 study, “Prevalence and types of coinfections in sleeping sickness (HAT) patients in Kenya between 2000 and 2009” dug into the details of HAT patients in public facilities. The study revealed that 31 patients—19 males and 12 females—were diagnosed with HAT during this period. Cases were reported in 2000 (12), 2001 (7), 2002 (10), 2006 (1), and 2009 (1). Tragically, two patients (6.4%) who were co-infected with HIV died, while the rest were successfully treated.
The average age of the patients was 32.5 years, with the majority (72.4%) under 40 years old. Of the cases, 29% were in the early stage of the disease, while 70% were in the late stage. Patients spent an average of 40 days in the hospital, with no significant difference in stay duration based on disease stage or gender, though females stayed slightly longer (41 days vs. 38 days for males).
Treatment for HAT was provided free of charge by WHO, but other costs—such as hospital beds, food, and treatment for additional ailments—averaged Ksh800 per day. Over the typical 40-day hospital stay, this amounted to Ksh32,000 per patient, which was covered by the Kenyan government. This study highlights the burden of HAT and the resources required to manage it, even as Kenya moves closer to eliminating the disease.
Kenya’s push for HAT-free certification builds on its 2018 success in eliminating Guinea Worm Disease, a milestone recognized by the WHO. Riding on this momentum, the country submitted a draft dossier in March 2020 seeking validation of HAT elimination as a public health problem.
Over four years later, Dickson Kioko, a leading sleeping sickness expert in the Ministry of Health in charge of monitoring and evaluating Vector Borne and Neglected Tropical Diseases Unit (VBNTDU), now tells Willow Health that Kenya is nearing the finish line.
“The process of applying for validation is well underway—it’s just a matter of time,” he says, emphasizing that Kenya has already “interrupted transmission” of the disease. This means new infections have been reduced to zero in endemic areas, with minimal risk of resurgence due to sustained intervention efforts.
Kioko further revealed that the WHO recently requested minor clarifications on Kenya’s surveillance system. “We have submitted the necessary documentation, and now we’re awaiting clearance, which could come sometime this year,” he noted.
For WHO to certify Kenya as having eliminated HAT as a public health concern, the country must demonstrate that cases have remained below the threshold of one per 10,000 inhabitants in endemic regions, particularly around the Lake Victoria Basin.
Historical outbreaks of Sleeping Sickness occurred in Homabay, Siaya, Bungoma and Busia Counties
The NTD distribution mapping conducted between 2000 and 2011 by the Ministry of Health identified Kenyan populations with over one per cent prevalence of NTDs, meeting the WHO’s threshold for public health concern. Parasitic infections such as schistosomiasis (SCH), soil-transmitted helminths (STH), lymphatic filariasis (LF), and leishmaniasis remain endemic in multiple counties, alongside bacterial infections like trachoma. Onchocerciasis, another parasitic disease, has an extremely low prevalence (<1%) in Kenya, rendering it insignificant as a public health threat. Meanwhile, zoonotic diseases such as rabies, HAT, and echinococcosis (hydatid disease) persist, though both HAT and hydatid disease are nearing elimination.
According to the Kenya NTD Master Plan, 2023-2027 Historical HAT outbreaks have occurred in Homabay, Siaya, Bungoma and Busia Counties and few reported cases in Migori and Narok counties.
It adds that the health facilities in the six formerly endemic counties lack the capacity to diagnose and manage HAT except the National Sleeping Sickness Referral Hospital (NSSRH) based at Alupe, Busia.
“The potential for recurring human sleeping sickness outbreaks is high in the Lake Victoria basin and the Serengeti-Mara region. The disease is fatal with high costs of medication and accompanying losses of manpower negatively affecting the economy. Human African Trypanosomiasis (HAT) affects the population and the productivity of the people. The cost of the disease is extremely difficult to quantify. According to WHO (2003), at least 60 million people are at risk of contracting the disease in Africa while 11 million Kenyans are at risk,” reads the Plan.
On a working tour in Busia County on December 10, 2024, Kenya Tsetse and Trypanosomiasis Eradication Council (KENTTEC) CEO Dr. Seth Onyango stated that tsetse flies affect 38 of Kenya’s 47 counties, spanning approximately 138,000 square kilometers. He noted that Busia, due to its proximity to the Lambwe Valley—an established tsetse fly hotspot—has historically struggled with heavy infestations across all seven sub-counties.
“Government interventions have however, successfully reclaimed infested areas, fostering a more suitable environment for livestock production and improving community livelihoods,” he said.
One key approach he said was the large-scale deployment of tsetse fly control measures, including insecticide-treated targets, traps, and aerial spraying in high-risk regions such as Busia, Lambwe Valley, and parts of western Kenya.
KENTTEC Board Chair Dr Geoffrey Mutai added that, since 2009, the World Health Organization and Kenya’s Ministry of Public Health have collaborated to position the country as a tsetse fly-free zone, with Busia playing a significant role in this achievement.
Kioko emphasizes that eradicating any neglected tropical disease requires time, meticulous planning, and strict adherence to WHO’s rigorous standards.
Kenya has successfully executed two consecutive NTD Master Plans (2011–2015 and 2016–2020), milestones that led to the elimination of Guinea Worm Disease and the interruption of transmission for both Onchocerciasis and HAT.
Kioko clarified that the strain of HAT found in Guinea—Trypanosoma brucei gambiense—is also prevalent in West and Central African countries. This form accounts for 92% of reported cases and progresses slowly, with infected individuals often remaining asymptomatic for months or even years. By the time symptoms manifest, the disease has typically advanced, affecting the central nervous system.
He explained that Kenya’s variant of HAT is caused by a parasite transmitted by tsetse flies (Glossina spp.) and other blood-sucking Diptera. The parasite affects both humans and animals, with the animal form known as Nagana or Animal African Trypanosomiasis (AAT).
“In Kenya, as well as in Eastern and Southern Africa, we have Trypanosoma brucei rhodesiense, which makes up only 8% of reported cases. Unlike the Gambian strain, it progresses rapidly. However, we have successfully interrupted its transmission and are now working toward WHO certification for elimination,” Kioko said.
WHO statistics indicate that the Eastern and Southern African strains of HAT present symptoms within weeks or months of infection. The disease progresses rapidly, leading to multi-organ invasion, including the brain.
On the eve of World Neglected Tropical Diseases Day, observed on January 30, the WHO commended Guinea for eliminating the gambiense form of HAT.
“Today’s announcement is both a testament to the global progress against neglected tropical diseases and a beacon of hope for nations still battling human African trypanosomiasis,” said Dr. Tedros Adhanom Ghebreyesus, WHO Director-General.
Guinea strengthened its diagnostic and treatment systems
This success is the result of a comprehensive approach that combined vector control, advancements in diagnostics and treatments, and active community engagement.
A key strategy was the use of “tiny targets”—small blue cloths treated with insecticide—to attract and kill tsetse flies, the insects responsible for spreading the Trypanosoma parasite. These targets were strategically placed in mangrove areas along the Fatala River, where tsetse flies are prevalent. The choice of blue cloth was based on scientific research showing that tsetse flies are highly attracted to this colour. This innovative method significantly reduced the tsetse fly population, leading to a noticeable decline in disease transmission in the targeted regions.
In addition to vector control, Guinea strengthened its diagnostic and treatment systems. The introduction of rapid diagnostic tests enabled quick and accurate detection of HAT cases, even in hard-to-reach areas. These tests allowed for immediate treatment, which helped curb the spread of the disease. Furthermore, the adoption of new oral medications, such as fexinidazole and acoziborole, simplified treatment protocols. Patients could now receive care at home, which improved adherence to treatment and overall outcomes.
Community engagement was another critical factor in this achievement. Local radio stations, such as Radio Rural de Forecariah, played a vital role in raising awareness about the disease, its symptoms, and prevention methods. Interactive radio programs encouraged community members to participate in control efforts and report suspected cases. This approach fostered a sense of ownership and responsibility among local populations, ensuring sustained participation in the fight against HAT.
Despite setbacks, such as the 2013 Ebola outbreak, which temporarily disrupted HAT control activities, Guinea’s unwavering efforts have led to a remarkable reduction in cases. From having the highest number of HAT cases in West Africa in the early 2000s, Guinea reported only 12 cases in 2024, marking a significant milestone in its public health journey.
Dr Matshidiso Moeti, WHO Regional Director for Africa, hailed Guinea’s achievement as a significant public health milestone. “With the elimination of HAT, vulnerable families and communities can now live free from the threat of this potentially fatal disease. I commend the government, health workers, partners, and communities for this crucial accomplishment. WHO remains steadfast in supporting nations striving to eliminate human African trypanosomiasis and other neglected tropical diseases in Africa.”
With Guinea, seven other countries have been validated by WHO for eliminating the gambiense form of HAT: Togo (2020), Benin (2021), Côte d’Ivoire (2021), Uganda (2022), Equatorial Guinea (2022), Ghana (2023) and Chad (2024). The rhodesiense form of the disease has been eliminated as a public health problem in one country, Rwanda, as validated by WHO in 2022.
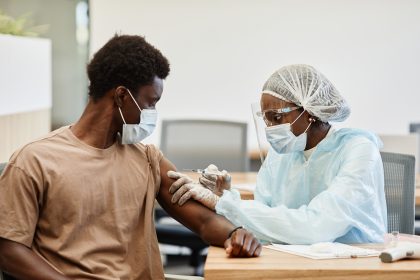
Kioko explains that diagnosing sleeping sickness involves a three-step process: initial screening for infection, microscopic confirmation of the parasite’s presence, and an assessment of disease progression through clinical examination—sometimes requiring cerebrospinal fluid analysis. Early detection is critical, as it prevents the disease from advancing to the neurological stage, where treatment becomes far more complex.
According to WHO, sustained control efforts like those done in Guinea have significantly reduced HAT cases, with reported infections dropping to a historic low—falling below 2,000 in 2017 and under 1,000 in 2018, a trend that has continued through 2022. During the 2016–2020 period, an estimated 55 million people remained at risk, though only three million faced a moderate to high risk of infection.




















Thanks for offering high quality reads 😀
Absolutely our pleasure! 😊 We’re thrilled you’re loving the reads—thanks for being part of the Willow community!