Microscopy TB tests, prone to human mood swings, would return false results, but Kenya is also adopting Artificial Intelligence- the smart partner who takes no Coffee Breaks
Sue Gakii, a Community Health Promoter in Imenti North, Meru County has been dealing with Tuberculosis patients almost on a daily basis, exposing herself to TB infection.
She has been helping in screening, active case finding and home visits for contract tracing from Giaki Sub-County Hospital where she’s also a Linkage Assistant.
Gakii’s worry about TB infection began three years ago when she started dealing with TB patients three years ago. Even more migraine-inducing were the prospects of infecting her family.

She explained her fears to the clinician at the hospital and a TB test was recommended. “I was asked to remove my sputum that was screened using the GeneXpert machine” and within two hours, she received an SMS to get her test results at the facility which turned negative.
Gakii was thus put on TB Preventive Therapy (TPT) for three months, taking her medication once a week without any side effects besides urine discolouration.
For donkey years, Tuberculosis diagnosis in Kenya has perennially been tested using sputum microscopy: sputum is taken and prepared on a slide with reagents. It is then checked under a microscope for bacteria which can be seen and counted. It could be, for instance, positive 1+, 2+ or 3+.
This method, also called Alcohol Acid Fast Bacilli (AFB), is still being used in many health facilities in Kenya, despite its many shortcomings.
According to John Mungai, the Project officer at AMREF in the Global Fund Program, the sputum microscopy test is prone to human errors leading to missing a lot of people with TB.
Mungai explains that human errors happen “during the slide preparation and using eyes to look at the microscope will depend on the mood of the person, they may be tired or bored and may end up not seeing the right thing.”
Mungai adds that even when done in the ideal settings, the AFB test can still miss diagnosing TB as the sensitivity of the test is low thus returning negative results.
Data from the National Tuberculosis, Leprosy and Lung Disease Program 2016 (NLTP) indicates that about 41 per cent of the people who had symptoms such as night sweats, fever and weight loss within two weeks of the test were missed and would continue transmitting TB in the community.
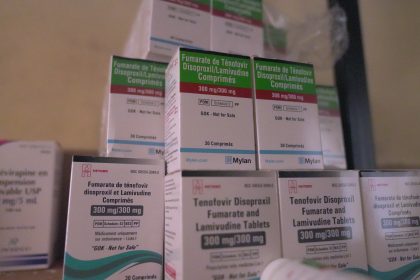
HIV tests are often done alongside TB tests because HIV weakens the immune system, increasing the risk of developing active TB. People with HIV are more likely to have TB, and TB is a leading cause of death among those with HIV. Early detection helps manage both conditions effectively.
The government thus came up with different measures and innovations to reach and identify the missing 40 per cent, following a recommendation to use World Health Organization (WHO)-approved molecular technology for testing TB.
Among these tools include; Ultra cartridge for GeneXpert testing, Truenat, Chest X-ray/CAD for TB, QuantiFERON test for latent TB diagnosis, LF Lam and TB-LAMP- for expanded access to diagnostic and screening services for Tuberculosis.
The GeneXpert test which returned Gakii’s results in record time, is one innovation Kenya adopted in 2011. It uses sputum or any other body fluid apart from blood using a cartridge and runs within two hours to produce the results.
Mungai says one of its advantages is the capacity of the GeneXpert to run several samples simultaneously within two hours to produce results.
“The GeneXpert is sensitive because it uses molecular technology by detecting the genetic material of the bacteria and even when the bacteria are few, the test can detect them,” he explains.
The other molecular test is the Truenat which is a Chip-based real-time micro-polymerase chain reaction (PCR) for detection of TB and Rifampicin-resistant TB from DNA extracted from sputum within an hour.
While the other machines are reliant on electricity, the Truenat is portable and can be used in remote areas without electricity. It has a rechargeable battery that can also be solar-powered.
According to the Centre for Health Solutions (CHS), there are 239 GeneXpert instruments as of June 2023 and 38 Truenat devices.
The other advantage of molecular technology over traditional tests are that they can test for drug-resistant tuberculosis. With previous use of microscopy, “one could not tell whether it was resistant or not and therefore, the patient was treated for two months and tested again to see whether the bacteria had disappeared,” explains Mungai. “If the bacteria are still active, treatment continues and after four or five months, they will get to know if the patient is resistant or not.”
Mungai says the only shortfall of the AFB test is that it can only test for Rifampicin resistance-which in TB happens when the bacteria change in a way that stops the drug from working, so the infection keeps growing even with treatment.
This is an advantage because a patient is not treated for five months for the medic to identify resistance to drugs meaning the patients gets the right drugs from the beginning.
Mungai says another advantage is that the AFB tests are less cumbersome, and have less contact with the sputum and thus minimal human interference. This results in fewer errors and the test requires one sample, unlike microscopy which requires several samples, (One in the morning and one on the spot)
Further, Mungai says despite the shortcomings of microscopy, it is still necessary because after two months under drugs, patients are tested again to see if they have become negative as most of the bacteria have been killed by the drugs in that period.
“This is done through microscopy because the new tests are looking for the genetic material of the bacteria and within two months, the genetic material will still be present and may indicate a false positive, but with microscopy, it will focus on the bacteria,” explains Mungai.
Mungai lists the challenges with the new technologies as expensive costs and reliance on donors raising sustainability issues.
Additionally, the machines are also fewer than the facilities and total Kenyan population, creating a logistic nightmare in collecting and transporting them to the facilities where machines are available.
Stockouts of the cartridges for GeneXpert and reagents for Truenat force the clinicians to revert to microscopy risking missing some cases.
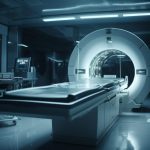
Another innovation is Artificial Intelligence (AI) in chest X-rays using Computer Aided Detection for Tuberculosis.
In 2016, the NLTP survey revealed that X-rays are powerful for screening for TB but were challenged by their availability in health facilities.
Mungai says low capacity of experts like radiologists to interpret the X-rays results in most being read by clinical officers or nurses who have learned on the job and thus subject to poor reporting or errors.
Kenya has therefore adopted AI as the next frontier in early Tuberculosis diagnosis to read the TB X-ray through the CAD which detects abnormalities.
He says that AI will work with digital X-ray machines and that a facility with digital X-ray machines can purchase the CAD and install it to read, interpret, and report in real-time.
It highlights heat maps by circling areas where there are problems in the X-ray films and gives a score, but would not identify if one is drug-resistant or not.
“Kenya has adopted a score of 0 per cent as the cut-off line and anybody scoring 60 and above is likely to have TB,” explains Mungai, adding that the clinician will do another test or initiate treatment, but the recommendation is to have a GeneXpert test to make further decisions.
The beauty of AI, says Mungai, is that it removes human errors and bridges the gap between a few radiologists to read the X-ray.
Additionally, AI can learn from reading a radiologist’s comments, and if doubtful, adjusts accordingly.
“AMREF has been doing targeted TB outreaches in far-to-reach areas, especially in communities with high TB prevalence and the portable CAD-enabled X-ray machine has been coming in handy,” Mungai says.
According to the Centers for Disease Control and Infection, another technology in the screening and diagnosis of Tuberculosis is the Interferon Gamma Release Assay (IGRA) which is a blood test that measures the body’s immune response to the bacteria that causes Tuberculosis.
IGRA tests for latent TB infection, not active TB disease. A negative IGRA result means it is unlikely the patient has TB, while a positive result means they have probably been infected in the past, and an unpredictable result means the test was invalid.
According to Jeremiah Ogoro, the Head of Diagnosis at the National Tuberculosis, Leprosy and Lung Disease Program (NLTP), there is a newer technology of using sequencing which is mostly for surveillance, identifying super-spreaders, and predicting undiagnosed cases in whole genome sequencing.
It can also be targeted for next-generation sequencing used to detect mutations associated with drug resistance to TB.
The government, he says, plans to procure a GeneXpert machine able to detect whether a person has TB, whether it is drug-resistant and identify the drug they are resistant to, unlike the current GeneXpert that can detect Rifampicin-resistant TB.
“One of the challenges with the innovations is that it is expensive to do capacity building, it takes people to adopt, meaning you have to train people, and it is also resource-dependent to install the technologies,” explains Ogoro.
Ogoro adds that integration of the National TB Data System (TIBULIMS) with machines like GeneXpert, Truenat and CAD streamlines data access and improves diagnostics besides utilizing data to meet continuous training and technical support needs.
Evaline Kibuchi, the Chief National Coordinator, of Stop TB Partnership-Kenya says recent statistics indicate that from 2019 to date, “we have reduced by half the TB-related mortality from 33, 000 in 2019 to 15, 000 in a recently released WHO report” and the only bottleneck in the way of sustaining that trajectory “is the low investment to TB both in the national government and the counties.”