GBS is hiding in plain sight. The data does not show it. The mothers do not know it. But the newborns feel it. It is time to look closer.
Kenya recorded 37,400 meningitis cases and 4,270 deaths in 2021, but one hidden killer of newborns is missing from those numbers, according to the Meningitis Progress Tracker.
Group B Streptococcus (GBS), scientifically known as Streptococcus agalactiae, is a leading cause of neonatal sepsis and meningitis globally. In Kenya, however, it remains largely invisible. Evidence of its impact comes mainly from hospital-based studies rather than routine surveillance systems.
Without reliable numbers, GBS struggles to compete for attention and funding against better-known causes such as meningococcus and pneumococcus – yet its effect on families is profound, often beginning in the first days of life and extending into long-term disability.
This was the urgent message delivered last week at the 4th International Symposium on Streptococcus agalactiae Disease (ISSAD) conference in Nairobi, Kenya, where researchers and global health experts gathered to confront a pathogen that kills and disables at the very start of life.
Meningitis is the inflammation of the membranes surrounding the brain and spinal cord. It can be caused by bacteria, viruses, fungi, parasites, or non-infectious conditions. Bacterial meningitis is the most dangerous form, commonly caused by four pathogens: Neisseria meningitidis (meningococcus), Streptococcus pneumoniae (pneumococcus), Haemophilus influenzae, and Streptococcus agalactiae (GBS).
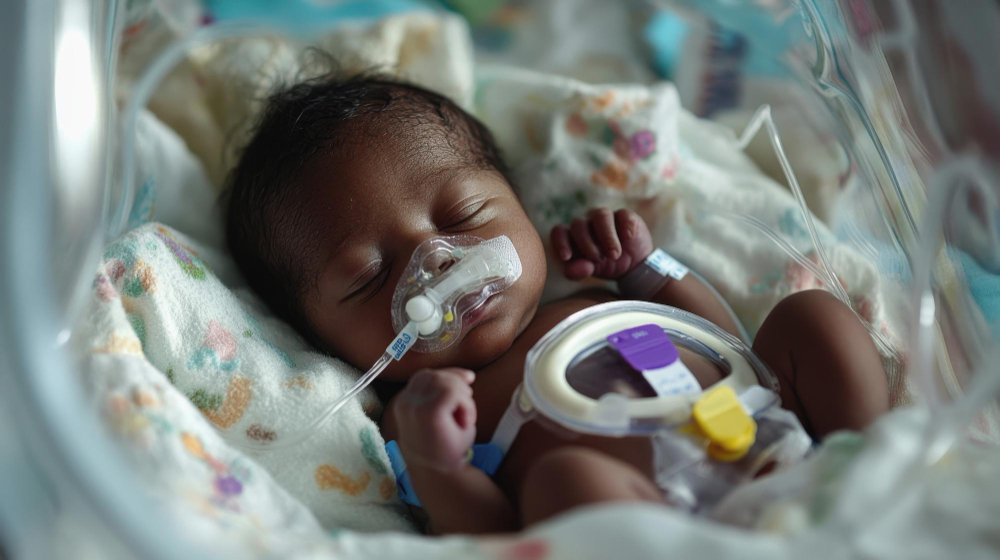
Newborns are particularly vulnerable to GBS because the bacterium commonly colonises the gastrointestinal and genital tracts of healthy adults, including pregnant women, without causing symptoms. Transmission can occur during labour or shortly after birth.
Officially, GBS does not exist in Kenya’s meningitis numbers, but is hiding in hospitals
In many high-income countries, routine screening during pregnancy identifies mothers who carry GBS, and antibiotics are given during labour to prevent transmission. In most low- and middle-income countries, including Kenya, this approach is not systematically applied, leaving prevention dependent on access to timely diagnosis and treatment after infection has already occurred.
Kenya’s national meningitis figures do not disaggregate reliably by pathogen, and GBS is rarely identified outside research settings. Limited laboratory capacity delayed lumbar punctures, and reliance on empirical treatment means that many cases are recorded as “unspecified bacterial meningitis” or “neonatal sepsis” without identifying the organism responsible.
Hospital-based studies tell a different story. Research titled “Clinical features to distinguish meningitis among young infants at a rural Kenyan hospital” found GBS among confirmed bacterial causes. A continent-wide scoping review published in BMJ Journals involving Kenyan institutions, “Group B streptococcus in pregnant women and neonates in Africa,” highlighted GBS as a persistent pathogen across Africa. These findings suggest that GBS is not rare — it is simply under-recognised.
Virginia Benassi, a Technical Officer based in Switzerland, told delegates at the ISSAD conference that this invisibility carries global consequences. “GBS is a leading cause of sepsis and meningitis in newborns and young infants worldwide. Mortality remains high, and many of those affected live with long-term neurodevelopmental consequences. The burden falls disproportionately on low- and middle-income countries.”
GBS does not cause epidemics, but its impact on newborns and their families is profound
She added that GBS does not attract the same urgency as epidemic-prone meningitis because it does not cause outbreaks. “Unlike meningococcal disease, GBS does not cause epidemics, so it is less visible. But its impact on newborns and their families is very profound. Without tackling GBS alongside other major causes, the global goals for meningitis cannot be fully achieved.”
The “Defeating Meningitis by 2030” global roadmap, developed by the World Health Organization (WHO) and global partners, is the first comprehensive strategy to address meningitis across the life course. Endorsed by the World Health Assembly, it sets three headline goals: to eliminate epidemics of bacterial meningitis; to reduce cases by 50 per cent and deaths by 70 per cent from vaccine-preventable bacterial meningitis; and to reduce disability while improving quality of life for survivors.
GBS is referenced in 41 of the roadmap’s 99 milestones, underscoring its centrality to achieving the 2030 targets. “The roadmap represents a global commitment, but its impact depends on implementation,” Benassi said. “It is the first comprehensive global strategy across the life course, guided by three global goals for 2030: eliminating epidemics, reducing cases and deaths from vaccine-preventable bacterial meningitis, and reducing disability and improving quality of life after meningitis from any cause.”
Prevention is the first pillar of the roadmap and includes the development and introduction of vaccines. For GBS, maternal vaccination is seen as a promising strategy because it protects the baby through antibodies transferred from the mother before birth. Global modelling suggests a maternal GBS vaccine could avert up to 17,900 cases of neurodevelopmental impairment associated with GBS disease – an impact that would extend far beyond preventing deaths, reducing the lifelong disability that follows meningitis in infancy.
Surveillance remains limited yet, GBS requires sustained and deliberate attention
“Maternal GBS vaccination represents a promising and achievable strategy,” Benassi said. “Vaccines are in development, but they are not yet available. Surveillance remains limited in many settings, and for these reasons, GBS requires sustained and deliberate attention.”
Ignacio Esteban, a paediatrician and epidemiologist, sees maternal immunisation as both feasible and strategic. “Maternal immunisation is considered a highly feasible and strategic approach to reducing neonatal mortality and disability, particularly for diseases like GBS and RSV. The feasibility of introducing such programmes is evaluated through multi-criteria decision analysis, which looks at factors ranging from supply chains to healthcare worker training.”
Countries already have experience with maternal tetanus vaccination, providing a platform for introducing newer vaccines. But Esteban emphasised that success depends on coordination. “We need strong integration and coordination between antenatal care and immunisation programmes to identify the best delivery strategy for each country.”
Under new global vaccine financing approaches, countries will increasingly work with a “one vaccine budget,” meaning they must prioritise introductions based on disease burden and evidence. “GBS could be an amazing investment when we look at the health impact. When we consider financial implications alongside health impact, it also shows a strong return on investment compared with other potential new vaccines,” Esteban said.
The second pillar of the roadmap focuses on diagnosis and treatment. In April 2025, WHO issued new guidelines on meningitis diagnosis, treatment, and care. Early recognition, lumbar punctures, and laboratory confirmation are essential to saving lives and choosing appropriate antibiotics.
Without laboratory confirmation, GBS remains under-counted and under-prioritised
“While we wait for vaccines, quality diagnosis and treatment save lives,” Benassi said. “High-quality diagnosis and treatment are essential both to save lives now and to generate the data needed to justify prevention strategies such as vaccination. Without laboratory confirmation, GBS remains under-counted and under-prioritised. And without data, prevention is delayed.”
Because GBS primarily affects newborns and young infants, the long-term consequences can shape an entire lifetime. “There is increasing recognition of the need to address disability and long-term consequences, but health systems are not yet fully prepared,” Benassi said. In Kenya, rehabilitation services are concentrated in a few urban centres, leaving rural families with few options and extending the social and economic costs of meningitis far beyond the initial illness.
Kenya has made progress in reducing under-five mortality, but neonatal deaths from infections such as sepsis and meningitis remain a major challenge. Addressing GBS therefore aligns directly with national goals on maternal and newborn health — and failing to do so would undermine Kenya’s contribution to global meningitis targets.
GBS may be a hidden pathogen, but its effects are not subtle. Bringing it into view through better data, stronger health systems, and eventual maternal vaccination could mean preventing thousands of deaths and up to 17,900 cases of lifelong neurodevelopmental impairment. For Kenya’s newborns, confronting GBS alongside other causes of meningitis could mean the difference between survival, disability, and death.