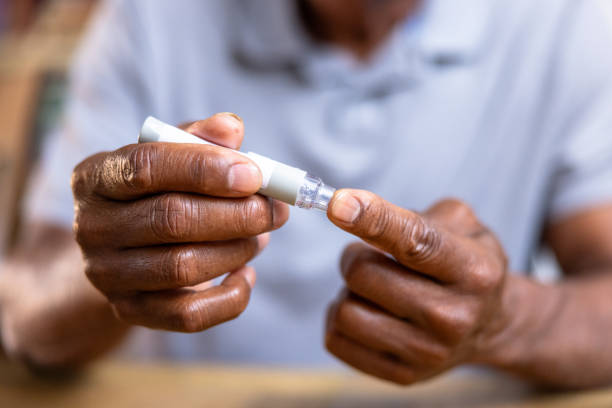
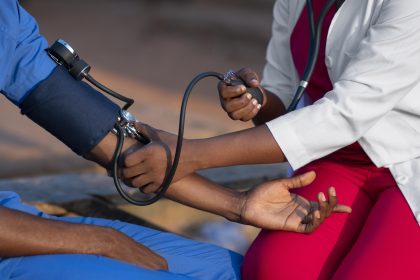
Maina’s struggle is a classic case of peripheral neuropathy—a serious complication of uncontrolled diabetes: phantom limb sensation and pain are known post-amputation experiences
For ten years, Maina managed his diabetes with discipline, never missing his medication. But he hardly attended clinic visits. Then, three months ago, something changed. He began feeling a bizarre, unbearable sensation—like insects crawling all over his face—along with numbness in his legs. Something was clearly wrong.
His medication might have needed adjusting based on his blood sugar levels. Yet, he couldn’t even remember the last time he had them checked. Then came an even bigger blow: his right leg had to be amputated a month ago.
“I still feel my leg—it’s like it’s there, but it burns, cramps, and stabs with pain,” he said, frustration filling his voice. He limped up and down, his agitation growing with every step. His exhausted expression made it clear—this was more than just a physical battle. The constant pain and phantom sensations were overwhelming. “Other diabetics keep telling me it’s normal, but how is this normal?” he snapped, his voice sharp enough to cut through the quiet hospital. Maina’s struggle is a classic case of peripheral neuropathy—a serious complication of uncontrolled diabetes. His phantom limb sensation and phantom pain are also well-known post-amputation experiences.
After an amputation, the brain can still “remember” the lost limb, making it feel as though it is still there
Peripheral neuropathy is one of the most common complications of diabetes. It occurs when prolonged high blood sugar damages nerves, especially those responsible for sensation, muscle control, and organ function. Symptoms include; numbness, tingling, burning pain, and unusual sensations—like insects crawling on the skin.
After an amputation, the brain can still “remember” the lost limb, making it feel as though it is still there. This is called phantom limb sensation. For some people, this illusion turns painful, leading to phantom pain—a burning, tingling or stabbing pain in the missing limb.
Uncontrolled diabetes damages nerves, especially in the feet and legs. Over time, this leads to numbness, making it easy for wounds and ulcers to go unnoticed. If these wounds get infected and don’t heal properly, amputation may become necessary to save the patient’s life. Even after amputation, the brain struggles to adjust, leading to phantom limb sensations and phantom pain.
Diabetes is a lifelong condition where the body struggles to control blood sugar levels. It causes symptoms such as: Excessive thirst, frequent urination, and unexplained hunger. According to the World Health Organization (WHO), the prevalence of diabetes in Kenya was 3.3% in 2023. This number is expected to rise to 4.5% this year, due to obesity due to sedentary lifestyles, lack of exercise, and poor diet. Globally, diabetes was the 9th leading non-communicable disease in 2019.
Sleep deprivation, fear of the unknown, loss of independence and isolation, increased risk of depression
Maina’s case clearly illustrates that the struggle following an amputation is not just physical but mental as well. Post-amputation complications, combined with sleep deprivation, fear of the unknown, loss of independence and isolation, significantly increase the risk of depression. Physical symptoms such as phantom pain, phantom limb sensations, and frequent urination further disrupt sleep, preventing the body and mind from resting and recovering.
This lack of sleep exacerbates emotional distress, making it harder for diabetics to manage daily life and increasing feelings of anxiety and hopelessness. As the sense of isolation deepens, and without proper support, individuals feel abandoned and misunderstood.
The worse the depression, the harder it becomes to maintain a self-care routine such as monitoring blood sugar levels and adhering to a healthy lifestyle. Poor diabetes management in turn worsens physical symptoms, increasing pain and further disrupting sleep – creating a vicious cycle that can be difficult to break.
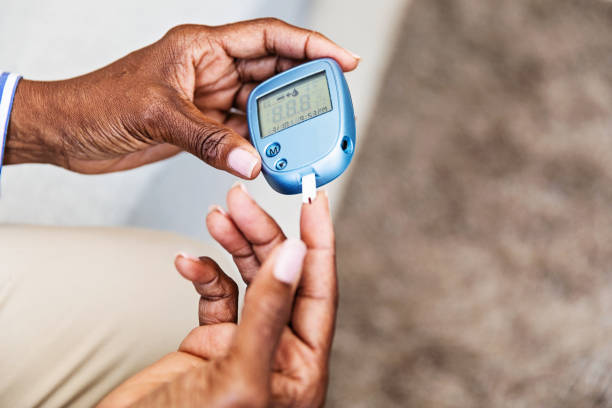
Checking blood sugar levels often and attending checkups help prevent complications.
Foot Care: Wear comfortable shoes and break in new ones gradually. Never walk barefoot—even indoors. Check your feet daily for cuts, blisters, redness, or swelling. Treat any injuries immediately.
Manage Mental Health: Improve sleep with relaxation techniques like deep breathing and meditation.
Join a support group or talk to a counsellor.
Stay active with safe exercises suited to your condition.
Maina’s journey is a harsh reality for many diabetics, but it doesn’t have to be yours. By controlling your blood sugar, taking care of your feet, and prioritizing mental health, you can avoid complications and live a fulfilling life. Diabetes is lifelong—but you can control it instead of letting it control you. Stay strong. Stay informed. Stay hopeful.
Dr Rachel Kerubo is the Resident Medical Officer – Department of Internal Medicine, Nyamira County Referral Hospital