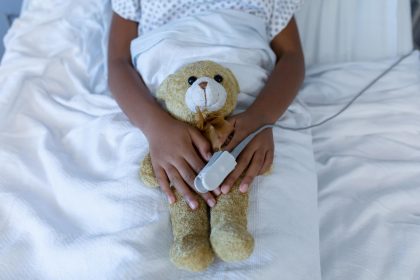
Group B Streptococcus (GBS) is Kenya’s silent killer: undetected, undocumented, and invisible to a health system too stretched to look for it. Even in death, it leaves no trace- but KEMRI is spearheading a vaccine.
“The baby was big,” recalls Julie Nyanchama of her 4.3-kilogram newborn, the kind that makes nurses smile, and mothers swell with pride.
Julie had delivered at St Mary’s Hospital in Nairobi in 2014, and despite a complicated birth marked by severe tearing and haemorrhage, her son seemed strong.
But by day three, he was burning with fever.

What followed was a maze Kenyan mothers know by heart. A trip to Makadara Health Centre, where medics, seeing a newborn only days old, referred him to Kenyatta National Hospital.
Fearing admission to Kenyatta would be costly owing to financial challenges at the time, Julie’s family, including her husband, “Felt that if I buy antibiotics, Amoxil and Flagyl, the baby will just be alright. So, I went back home with the baby,” she told Willow Health Media.
On day seven, the baby began convulsing and was rushed to the hospital. After testing, he was diagnosed and treated for Group B Streptococcus (GBS).
Overcrowded wards rarely have resources for blood cultures needed for a diagnosis
In Kenya, GBS often goes undetected because the health system does not routinely screen for it. Overcrowded wards rarely have the resources to perform the blood cultures needed for a diagnosis, which means the bacteria are frequently missed, even in fatal cases. This has left GBS largely invisible in the country’s health data.
On February 23, scientists from 37 countries gathered in Nairobi for the 4th International Symposium on Streptococcus agalactiae Disease, ISSAD 2026. It is the second time in the symposium’s history that it has been held in Africa, which bears the biggest burden.

Prof Ziyaad Dangor, a Clinical Research Director at the VIDA Research Unit, Wits University, told delegates that about 54 per cent of GBS cases globally occur in Africa, where they account for 65 per cent of deaths. About 1.12 babies in Africa develop invasive GBS disease for every 1,000 live births, a rate that could be up to four per 1,000 births in sub-Saharan Africa.
“Globally, around 400,000 babies develop invasive GBS disease every year. Of the estimated 90,000 who die, 55 per cent are in sub-Saharan Africa,” explained Prof Dangor. “A baby who contracts GBS in Africa faces a case fatality risk four times higher than a baby born in a wealthy country. In Africa, 23 per cent of babies with invasive GBS disease die,” he added.
When a newborn survives GBS, it is likely to have impairment
Survival does not guarantee escape. Studies from Denmark and the Netherlands, tracking millions of births, found that 10 to 25 per cent of GBS survivors develop neurodevelopmental impairment.
The picture darkens in low-income countries. In one five-country study, the rate of lasting neurological damage soared to between 70 and 80 per cent in some settings. In South Africa alone, more than 40 per cent of surviving infants showed impairment.
“When you survive it, you are likely to have impairment,” Prof Dangor said. “That is extremely worrying.”
Prof Dangor also told delegates that worldwide, roughly one in five pregnant women -18 to 20 million-carry the GBS bacteria in their rectum or vagina at any given time. Most feel nothing. Yet during birth, it can pass to the baby, colonising lungs, blood and brain with devastating speed.
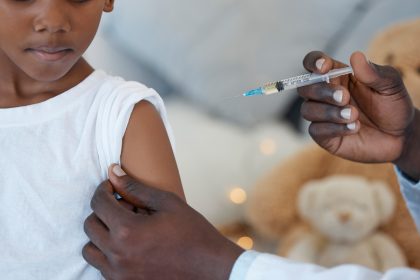
The only proven prevention is antibiotics for mothers who carry GBS
More than 80 per cent of early-onset GBS disease strikes within the first 24 hours of birth, because infection has already occurred in the womb, while membranes are still intact. By the time a baby is born symptomatic, the window for easy intervention has usually closed.
Experts say the only proven prevention is intrapartum antibiotic prophylaxis- antibiotics given during labour to mothers who carry GBS. In countries like the United States and the United Kingdom, universal screening identifies GBS-positive women before delivery, and the prophylaxis led to a sharp early drop in newborn infections.
But progress stalled. After the initial decline, infection rates plateaued, and for more than 20 years, little has changed, even in high-income settings.
In Kenya and much of sub-Saharan Africa, this prophylaxis is rarely used in any systematic way. Routine GBS screening is not offered in most antenatal clinics. Most women go through pregnancy without ever being tested. No test means no antibiotics. No antibiotics means no protection during delivery.
She chose an elective CS, the second baby was born healthy and infection-free
Julie knew the risk. She has thyroid disease, which weakens immunity and raises the chance of infection. In her next pregnancy, now insured and employed, she did things differently: treated her thyroid condition, chose an elective caesarean, and received proper care. Her second baby was born healthy and infection-free.
“When you have a woman who is empowered, when you have your own resources, you can make decisions independently,” she said, meaning the outcome of a baby’s first hours of life often hinges on a mother’s capacity to afford transport to a better hospital.
Prof Dangor presented data from the NEST 360 study showing a stark cascade: most septic newborns receive antibiotics, but vanishingly few receive a blood culture to confirm the cause. Without a culture, GBS remains undiagnosed—and what remains undiagnosed remains absent from the data. And what is absent from the data commands no urgency, no funding, and no policy.
“If you are not going to do the blood cultures, you are not going to detect the group B strep,” Prof Dangor said.
The babies were buried before anyone ever knew what killed them
Even when blood cultures are taken, they often fail to detect GBS. In South Africa, research found that 86 per cent of neonatal GBS deaths were only identified after death, on post-mortem. The babies were buried before anyone ever knew what killed them.
Molecular testing would improve detection rates substantially, but it is expensive, requires significant infrastructure and remains unavailable at most Kenyan facilities. The gap between what is happening and what is being recorded is not a small measurement error.
Dr Dorota Jamrozy of the Wellcome Sanger Institute presented data from the Juno project, the largest global genomic surveillance effort for GBS to date, encompassing over 22,000 bacterial genomes from 61 countries.
The findings revealed that one particular lineage dominates infant disease worldwide. Known as sequence cluster 3, it drives early-onset disease across most regions and is overwhelmingly dominant in late-onset disease globally.
In sub-Saharan Africa, this lineage has undergone what genomicists call clonal expansion, where a single bacterial strain proliferates rapidly through a population, clustering tightly in ways that suggest deep, sustained transmission across the region.
KEMRI getting ready to introduce maternal vaccines when available
The leading GBS vaccine candidates target serotype 3, among others. Based on current data, such a vaccine would cover the most common strains in Kenya and sub-Saharan Africa. With candidates in late-stage trials, licensure is closer than ever.
Preparations are already underway: KEMRI, through a network spanning nine African countries, is getting health systems ready to introduce maternal vaccines when they become available.

Marti Perhach, chief executive of Group B Strep International, tried to turn the statistics into something visceral. Her daughter was stillborn because of GBS.
“Each day, 1,200 babies are estimated to be infected by group B strep before birth through several months of age. Of those, 375 will die. 101 will have lifelong neurodevelopmental challenges. And 1,419 preterm births will be associated with maternal GBS colonisation,” she told the delegates.
Behind every number is a baby, family, professionals working under pressure
According to Jane Plumb, chief executive of the charity Group B Strep Support, whose son Theo passed away at just 15 hours old, these figures represent faces.
“Behind every number is a baby, a family, and a team of health professionals who are often working under pressure and without all the information that they need,” she said.
Julie Nyanchama is now a senior research scientist at KEMRI. She stood at the opening of a global scientific symposium and told her story: the panic, the financial calculation, the walk home with antibiotics that were not enough, the convulsions, the ambulance, the ward.
Her first child survived with a slight delay in milestones that eventually resolved. Her second child was born healthy. She is, by her own account, one of the fortunate ones. She is also, now, one of the people working to ensure that fewer mothers face the choice she faced in 2014: between a hospital bill they cannot pay and a baby who cannot wait.
“We are here as parents to voice our stories,” she said. “To really work together with all of you to ensure that no family goes through this.”
In Kenyan maternity wards, GBS remains largely invisible on charts and absent from most screening programmes.