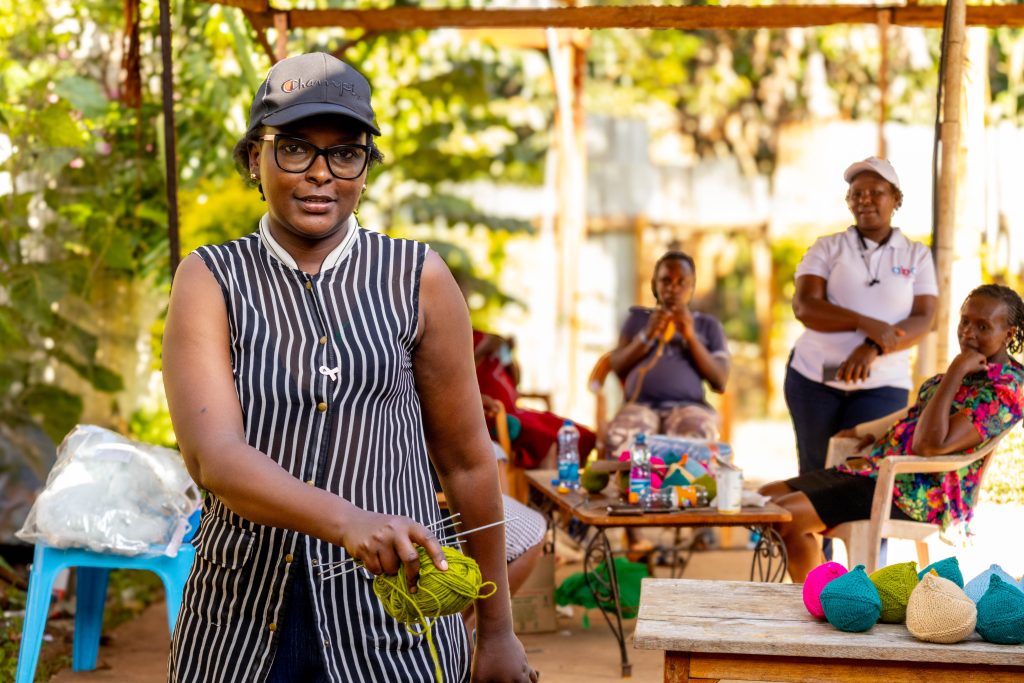Besides other side effects of treatment, like losing hair and vomiting after chemotherapy, I had the challenge of balancing with one breast– Dionisia Mugo
Collen Ndwiga, a single mother in her mid-30s from Embu County, was recently diagnosed with breast cancer and has already undergone a mastectomy—a surgical procedure to remove a breast, often used to treat breast cancer or, in some cases, prevent it in individuals with a high risk.
Ndwiga was diagnosed with Triple-negative Stage 3 breast cancer in June 2022. But she didn’t choose a mastectomy right away. Instead, her doctor recommended a lumpectomy—a surgery to remove the breast tumour and a small area of surrounding tissue while keeping the rest of the breast intact.

“When you get such sad news, you run to your mother or father, but sadly, I am an orphan, and I didn’t know where to go or what to do,” says Ndwiga, who began her treatment with the lumpectomy, coupled with chemotherapy, radiotherapy and immunotherapy. But alas! a repeat scan indicated the cancer had grown back, and she had to undergo a full mastectomy in August 2024.
More bad news followed: Ndwiga lost her job, where she was remotely supporting patients receiving treatment from abroad by billing insurance companies.
This devastated her, but her siblings, despite doing menial jobs, offered to take care of her young son.
“Right now, I am doing some manual jobs because as a mother, lazima ujitume (‘you have to push yourself’) because my son will ask what have I brought him. He has been my biggest reason to want to fight this so that he doesn’t grow up without a mother,” she says wistfully.
Ndwiga has been using breast prostheses from a team of women who help other breast cancer survivors who have undergone mastectomies. Some of her former colleagues were afraid to visit, with one confessing, “he had not seen a breast cancer survivor before, so the stigma is real.”
In her treatment and healing journey, Ndwiga has not been alone. Dionisia Mugo, also a breast cancer survivor, took her into the knitting group and taught her how to knit breast prostheses, besides helping with her upkeep.
Mugo was diagnosed with breast cancer in 2018 and also underwent a full mastectomy.
“Despite all the other side effects of treatment, like losing hair and vomiting after chemotherapy, I had the challenge of balancing with one breast,” she says.
She would then stuff rags in her socks and use them as a prosthesis because, then, a proper silicone prosthesis was expensive, considering she was also spending a lot of money on treatment. Someone sold her a silicone prosthesis for Ksh25,000, including a bra, but she bought it for Ksh22,000 after receiving a bra donation.

Mugo, however, didn’t wear it for two months as “It was too heavy. I was feeling uncomfortable because I didn’t pick the right size. So, I still ended up using the stuffed socks until I met someone who showed me the knitted ones that were so soft and easy to wear.”
This was how the idea of forming the knitting group was born. Mugo brought together almost ten women, including breast cancer survivors and caregivers, who have been knitting “boobies” and donating them to hospitals and women who need them.

Christine Wamaitha, a retired civil servant, is one of the beneficiaries. But on receiving news that her biopsy showed she had Stage 2 Breast cancer, “my blood pressure shot up. I was in denial.”
Wamaitha recalls setting her life “straight with God because I am waiting for death anyway” and it took a lot of convincing from a neighbour, after her young son shared the news, for her to agree to take up treatment, including a mastectomy, chemotherapy and radiotherapy in 2005.
Wamaitha was introduced to silicone breast prostheses before meeting the knitting team, where she is still learning how to knit.
For Rose Waruguru, a nurse, the knitting team has provided solace, encouragement and advice on the right diet during treatment and wound care.

She was first diagnosed with breast cancer in 2022 after she went for a thorough check-up following her partner’s succumbing to cancer.
“I had a lump on my left breast while in high school, but it was a fibroadenoma, a non-cancerous breast tumour that most often occurs in young women. It was removed, but recurred,” she says.
Several years after having her child, she noticed a lump in her right breast, and the test results showed it was breast cancer, for which treatment and a full mastectomy followed.
Waruguru, who is glad she found the knitting group, laments that “Reconstructive surgery is not pocket-friendly to many women because it is not covered under SHA.”
According to Global Cancer Statistics (GLOBOCAN 2020), breast cancer is the leading type of cancer in Kenya, accounting for 16.1 per cent. An estimated 6,799 cases were diagnosed in 2020, compared to 5,985 new cases in 2018. Deaths due to breast cancer rose from 2,553 in 2018 to 3,107 in 2020, making it the second-leading cause of all cancer deaths in Kenya.
Dr Karen Mbaabu, an Oncoplastic Breast Surgeon, says breast cancer is often diagnosed as a painless lump, a change in breast appearance or hardness, a swelling, or a change in the skin texture.
Dr Mbaabu explains that new patients are taken through triple assessment, and “The first one involves taking the history, to see if there are any risk factors such as early age at getting periods, later age at first birth, later age at menopause, family history of breast or ovarian cancer, use of alcohol or cigarettes beyond the recommended amount.”
GLOBOCAN 2020 data indicate that about 90 per cent of breast cancer cases occur sporadically, while five to 10 per cent can be attributed to genetic predisposition.
Also, invasive ductal carcinoma (IDC) is the most common histological type diagnosed, accounting for up to 75 per cent of all breast cancers. Breast ducts are the passageways where milk from the milk glands flows to the nipple. Invasive Ductal Carcinoma is a cancer (carcinoma) that happens when abnormal cells growing in the lining of the milk ducts change and invade breast tissue beyond the walls of the duct.
Dr Mbaabu explains that a physical examination is then done by assessing the breast lump, looking at any suspicious changes, hardness, skin texture, nipple discharge, and lymph nodes around the breast area.
The second part of the assessment is the radiological test, which could either be a mammogram or an ultrasound, used together or separately.
“A mammogram is recommended to women above 40 because the breast tissue and density begin to change at that age,” offers Dr Mbaabu. “The whiter it is, the more difficult it is to interpret the mammogram, unlike in younger women who have dense breasts, which is why we recommend an ultrasound for younger women, which is not going to show the white tissue.”
The third assessment is the biopsy, where a piece of tissue from the area of concern is lab tested to determine the kind and nature of the cells. After a diagnosis, the doctor then proceeds to staging, an investigation that looks for the spread of the cancer beyond the breast, either to the lungs, lymph nodes, or other organs like the brain, bones, or pelvic organs, which Dr Mbaabu says is done by a CT scan.
The World Health Organization (WHO) recently ranked Kenya Africa’s best country in breast cancer control, which Dr Mbaabu attributes to a multi-disciplinary team approach in handling breast cancer.
She explains that “Breast cancer is hardly ever treated by one person” and a specialist team—including medical and clinical oncologists, surgeons, radiologists, pathologists, breast care nurses, psychologists, and dieticians—works together to provide comprehensive treatment options for breast cancer patients. This has been “enhanced by telemedicine, having online meetings and sharing images.”
Dr Mbaabu also adds that Kenya has an increased diagnostic landscape and treatment with more facilities that offer mammograms, ultrasounds and more specialists who can interpret the tests than other African countries.
Kenya also has a policy network with bodies mandated to deal with cancer, like the National Cancer Institute and the National Cancer Network, which leverage government efforts.
Dr Mbaabu explains that breast cancer is treated in five main ways, often combined. These include a lumpectomy—a surgery to remove the breast lump while preserving the breast—followed by radiotherapy for the remaining tissue.
A mastectomy removes all breast tissue, with options for breast reconstruction or staying flat. Chemotherapy, an IV treatment, travels through the body to kill cancer cells. Radiotherapy uses invisible X-rays to target inoperable cancer areas. Hormonal methods treat hormone-sensitive tumours, identified through biopsy. Immunotherapy targets specific cancers based on their characteristics.
Like Mugo, many women skip breast reconstruction after a mastectomy due to the financial strain of cancer treatment. However, Dr Mbaabu notes that every woman is counselled and offered the choice of reconstruction—either right after the mastectomy or once treatment is complete. “A breast reconstructive surgeon may use tissue surrounding the breast or from the tummy wall, including the fat, skin, and blood vessels there, to form a breast-like shape, very similar to the natural breast, then connect the blood vessels to the ones that were supplying the breast originally,” explains Dr Mbaabu.
Young women often fear a mastectomy might impact fertility, but Dr Mbaabu clarifies that breastfeeding is still possible after a lumpectomy. For those concerned about chemotherapy or radiotherapy affecting fertility, egg preservation is an option, allowing for future pregnancy through implantation or a surrogate. She adds that past underreporting of breast cancer cases may have stemmed from limited data and the stigma faced by women, particularly those who underwent mastectomies, within their families and communities.

Dr Geoffrey Wango, a counselling psychologist, says a woman needs to accept herself first after a mastectomy and avoid self-stigmatisation. This helps in the healing process, even before taking up a breast prosthesis or breast reconstructive surgery, both of which boost her self-esteem.
“One can feel a void after a mastectomy, but she needs to understand it was done for her healing and not because of something she did or did not do. This way, she will heal from within,” explains Dr Wango, adding that partners of women who have undergone a mastectomy should accept, empathise and compliment like before, instead of reinforcing feelings of incompleteness.
Societal awareness of mastectomy is important, says Dr Wango, as some women reject it for fear of stigma and “Some women have gone through body-shaming, which can lead to lower self-esteem, trauma, and post-traumatic stress disorder, and can also lead to depression, and at worst, one can become suicidal.”