Postpartum haemorrhage may be caused by a blood disorder or giving birth to a big baby, and the uterus does not contract after delivery
Picture this: You are a professional in the medical field. You know the danger signs, you clearly feel life oozing out, but there is nothing you can do.
This was the scenario in 2009 when Dr Eunice Atsali, a midwife and a lecturer at Kenyatta University, gave birth to her second child.
“I could feel doom, like I was dying. I even requested the nurse to bring my baby before I died. This was very scary,” she recalls.

Dr Atsali would have died had she not been attended to in good time due to postpartum haemorrhage- which is excessive bleeding after delivery, one of the leading causes of maternal mortality in Kenya.
She had delivered through a Caesarean Section and her obstetric and gynaecologist had given her a clean bill of health.
In fact, she was in the recovery area inside the theatre, but when she woke up after her anaesthesia had worn off, she felt severe abdominal pain and was bleeding.
“I immediately called the nurse who said she had noticed my blood pressure reducing, so she had added fluids, and when she lifted the sheet that was covering me, blood dropped to the floor, and she screamed PPH,” recalls Dr Atsali.
Obstetrics diagnosed her with disseminated intravascular coagulation, a condition that causes blood not to clot.
Lucky for her, she had delivered in a healthcare facility with specialists and enough blood and blood products and other drugs that help stop postpartum haemorrhage, which can happen to any woman for various reasons.
Dr Atsali was shocked, though, as her haemoglobin levels had been good throughout the pregnancy.

According to the World Health Organization (WHO), postpartum haemorrhage is the leading cause of maternal mortality, estimated at almost 30 per cent, which is 223 maternal deaths per 100,000 live births by 2020.
This remains above the Sustainable Development Goal target of 3.1 of not more than 70 maternal deaths by 2030.
According to Dr Atsali, also the National Secretary for the Midwife Association of Kenya, health facilities with delivery services need to be well equipped with the right resources and specialists. All mothers should be educated during antenatal clinics to identify danger signs during labour and after delivery.
According to the Ministry of Health, Kenya records about 1.4 million deliveries, and 5000 maternal deaths each year, and 20-30 per cent are a result of postpartum haemorrhage.
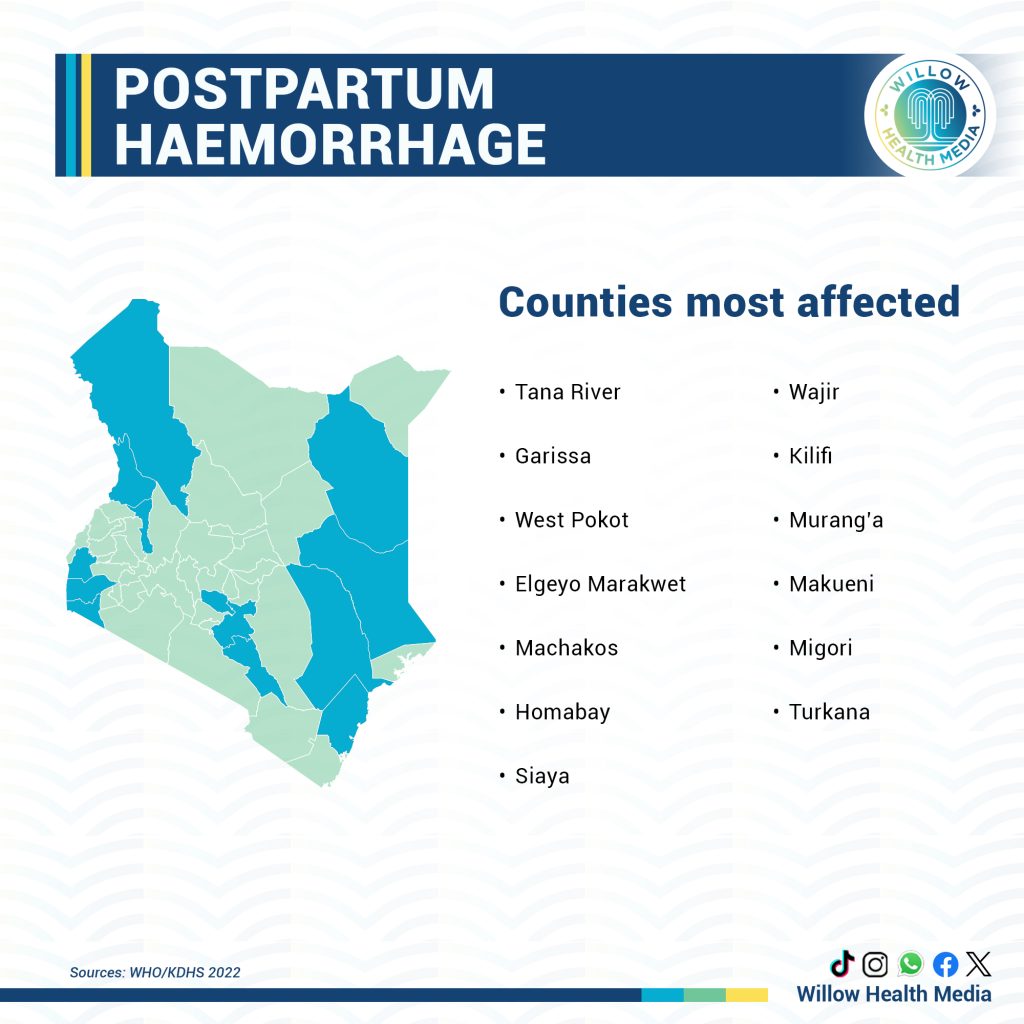
The most affected counties include Tana River, Garissa, West Pokot, Elgeyo Marakwet, Machakos, Homabay, Siaya, Wajir, Kilifi, Murang’a, Makueni, Migori, and Turkana.
Dr Atsali says the Midwives Association of Kenya is offering training on early signs for mothers to handle them or refer when not able to.
Prof Moses Obimbo, the Secretary of Kenya Obstetrics Gynaecological Society (KOGS), explains that postpartum haemorrhage is the loss of more than 500ml of blood within 24 hours of giving birth normally and more than one litre of blood after giving birth through Cesarean Section.
Prof Obimbo says that postpartum haemorrhage may be caused by uterine atony, where the uterus does not contract after giving birth.
“Usually when a woman delivers, the uterus contracts shutting off all the blood vessels, but when it sometimes fails to do so, it can lead to excessive bleeding,” explains the associate professor at the University of Nairobi.
He says a woman may bleed excessively due to trauma if she has a tear during delivery, such that when a baby is navigating through the system, it can result in tearing the walls of the uterus, cervix or vagina and lead to bleeding.
Retained tissue in the placenta could also cause excessive bleeding after delivery.
Some women may have blood disorders such that their blood cannot coagulate faster than expected, leading to excessive bleeding.

Prof Obimbo further explains that women with big babies and multiple pregnancies may expand the uterus, which may not contract very well after delivery.
Some women may have a small baby, but it does not navigate well, leading to tears, and others may have anaemia that may expose women to bleeding after delivery.
Further, women who have had a Cesarean Section before, while others may have placental disorders where the placenta appears to be in good shape, but could be extra low or have an additional segment which may not be seen during delivery, hence causing bleeding.
Prof Obimbo says postpartum haemorrhage leads to death if a woman “bled more than two litres of blood with no help in sight or blood for transfusion.”
This, in turn, leads to “cardiovascular shock, blood volume will go down, and the heart will beat faster to get the blood circulated to all the vital organs. She will get dizzy, then develop intravascular coagulopathy where blood coagulates into small pieces and destroys her vital organs like the kidney, liver and heart. This can cause ischemia to the brain and cause death,” he explains.

Additionally, Prof Obimbo explains that in the management of postpartum haemorrhage, prevention is key in identifying women at a higher risk, and this should start during the antenatal clinic.
Prof Obimbo advises women who suffer postpartum haemorrhage to get the Emotive Package- a life-saving intervention to reduce severe bleeding. It includes a calibrated blood-collection drape, a treatment bundle which includes uterine massage, medicines to contract the womb and stop the bleeding, intravenous fluid administration, examination and escalation to advanced care.
“The healthcare professional will massage the uterus and give uterotonic medication like oxytocin, which is the most commonly used or heat-stable Carbetocin, and if the uterus does not contract well, they will examine for possible tears and if found, they are repaired,” he adds.
If the tears are repaired and the bleeding continues, the medic will check if there is a retained product or tissue in the uterus, and it will be removed. If all that is done and the bleeding does not stop, then a blood test is done to check why it is not clotting.
Prof Obimbo says blood transfusion is also an idea, but if the bleeding does not stop, a balloon catheter is inflated inside the uterus to create pressure against the walls and stop it from bleeding.
If this does not work, the woman is taken into the theatre to suture the uterus and make it small to stop the bleeding or remove it completely.
Currently, Prof Obimbo is working on a five-year research project to end postpartum haemorrhage by 2030 via addressing four key strategic pillars: advocacy and awareness, strengthening research and evidence, innovating health systems and improving data.
This will help reduce maternal mortality through postpartum haemorrhage from 40 per cent to less than 10 per cent in five years and improve maternal health outcomes.

Dr Laura Oyiengo, UNICEF Health Specialist, says UNICEF is addressing postpartum haemorrhage in Kenya via introducing low-cost, effective, innovative products like the compression suit designed to apply external pressure to a woman’s lower body to reduce blood flow to the uterus and reduce shock.
Dr Laura says a woman can bleed to death within 30 minutes, but the pressure suit allows the patient to be transferred to a healthcare facility equipped to provide the right treatment for postpartum haemorrhage within 48 hours.
Dr Laura adds that UNICEF is strengthening primary healthcare by training Community Health Promoters to provide maternal and newborn care.
“For the many women who die due to postpartum haemorrhage up to 91 per cent of the cases are because they got suboptimal care, says Dr Rael Mutai, the County Director of Liverpool School of Tropical Medicine, which has been training healthcare workers to respond to emergency obstetrics and newborn care issues, including postpartum haemorrhage.
Emergency obstetrics and newborn care is a set of life-saving interventions that treat and manage the causes of maternal and newborn mortality.
According to Dr Mutai, “a healthcare worker should be able to give antibiotics, uterotonics, intramuscular anticonvulsant for pre-eclampsia, do manual removal of the placenta, do assisted vaginal delivery, neonatal resuscitation and refer the patient if the resources required are not available.”